HealthManagement, Volume 19 - Issue 2, 2019
An overview of recent advances showing the value of using AI in medical imaging.
Soon every medical imaging machine will be connected to the cloud where AI algorithms will analyse data and help human doctors screen, assess, and diagnose patients. The potential impact of implementing AI to analyse medical images is huge.
The world's first AI Precision Health Institute
The world's first AI Precision Health Institute at the University of Hawai‘i Cancer Center uses AI to analyse medical images to assess health and predict risk of disease. The AI-PHI is located at the UH Cancer Center in Honolulu in one of the most beautiful settings in the world overlooking the Pacific Ocean. The six story 150,000 square foot UH Cancer Center is one of only 69 NCI designated cancer centers in the United States and the only one in Hawai‘i and all of the Pacific Islands. The NCI designation signifies the depth and quality of the research they're doing.
The UH Cancer Center is a state of the art facility that has the ability to attract the best scientists to research cancer. Their research is unique because they research how cancer affects people with different ethnic, cultural and environmental characteristics. UH researchers conduct population based and laboratory based cancer research. Since Hawai‘i has one of the most diverse populations in the world, it's an ideal place to study why some ethnic populations are more susceptible to certain cancers and how genetic susceptibility interacts with environmental factors in producing cancer risk.

Research at UH has shown that certain ethnic populations have higher abdominal fat even if they are not obese. This abdominal fat leads to an increased incidence of liver cancer. They are researching ways to treat and prevent the accumulation in abdominal fat in these groups to reduce the risk of liver cancer.
Research in breast cancer at UH has revealed differences in survival rates among women from different ethnic backgrounds. Japanese women have the highest survival probability, followed by Chinese and Caucasian women. Native Hawaiian and Filipino women have lower survival rates. Researchers are studying factors including environment, diet, genetics, weight, and hormonal statuses that could help explain these differences.
John Shepherd, PhD founder and director of the AI-PHI and his colleagues created the first Hawai‘i and Pacific Islands Mammography Registry and are designing a study that will analyse mammograms from 5 million women on 5 continents using deep learning. Dr. Shepherd is developing novel biomarkers and conducting research in the following four areas:
- Bone density and body composition: Researching the combination of DXA and bioimpedance measures to describe fat and muscle status in athletes and other individuals where hydration may vary.
- Breast Cancer: Improving the ability of mammography to detect cancer and to offer quantitative risk of cancer, and using deep learning models for reading mammograms to reduce recall rates and unnecessary biopsies for women.
- Body Shape: 3D optical whole body scanning for quantifying body shape as a risk factor for metabolic diseases, and monitoring lifestyle interventions.
- Frailty: Researching the best way to describe frailty and function using quantitative composition measures.
Recently the AI-PHI partnered with QUIBIM a top tier AI company based in Spain. The AI-PHI is using the QUIBIM Precision Platform to centrally manage, store and quantitatively analyse medical images and algorithms. They are creating large scale imaging repositories with automated extraction of imaging biomarkers to characterise patients’ status. The QUIBIM platform will be the central repository for the AI-PHI's mammography studies, which over time will include mammograms from over 5 million women on 5 continents. The AI-PHI will also use QUIBIM to integrate AI algorithms to detect cancer without the need of radiologists in a first-read. QUIBIM applies AI enhanced methodologies to detect changes produced by diseases and drug treatments and provides accurate quantitative information to doctors, clinicians and researchers. QUIBIM has developed AI algorithms for many types of cancer including brain, breast, and prostate, as well as non-Hodgkin's Lymphoma, and other diseases.
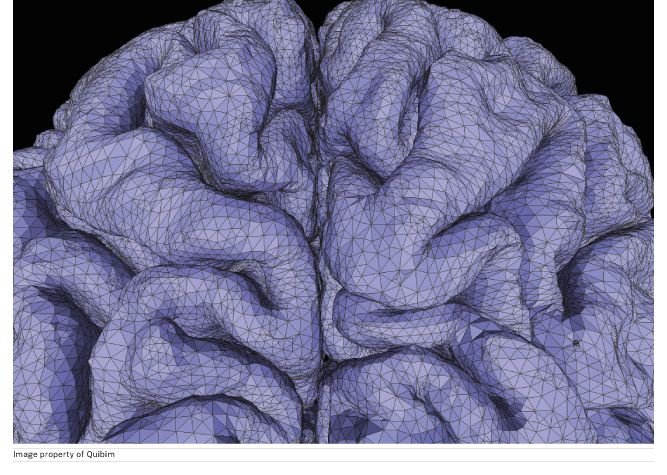
This is a close-up image of human brain sulci, reconstructed in 3D after processing a T1 MRI brain scan with QUIBIM Precision platform. This allows us to extract volumes from different brain regions and calculate the thickness of the gray matter cortex. With the surface extraction of grey matter, we can analyse important aspects such as neuronal density and grey matter thickness which are related to neurodegeneration. Since many neurodegenerative diseases occur as a result of these processes, this analysis can help to diagnose diseases such as Alzheimer's, Multiple Sclerosis, Parkinson's, and Amyotrophic Lateral Sclerosis.
Many lives could be saved worldwide every year if disease is detected and treated early. Using AI to analyze medical images is the most efficient and cost effective way to screen and help diagnose many diseases and the impact would be huge. Efforts have already begun in this direction. This is why AI in medical imaging may make the biggest impact in healthcare worldwide.
The following are recent advances showing the value of using AI in medical imaging:
- In a study at Stanford one algorithm named CheXNeXt (med.stanford.edu) read chest X-rays for 14 different pathologies. In this study the algorithm matched expert radiologists in accuracy and was much more efficient. The radiologists took an average of 4 hours to read an image; the algorithm read them in less than 2 minutes with the same level of accuracy.
- In China, NovaVision Group used AI (cnbc.com) to screen for over 1,000 diseases by analysing one image of the eye. They are able to find disease with 97% accuracy.
- Researchers at University of Warwick have developed an AI algorithm that can reduce the processing time for abnormal chest X-rays from 11 days 3 days. The study “Automated Triaging of Adult Chest Radiographs with Deep Artificial Neural Networks,” was published in Radiology on Jan 22 2019 (Mauro et al. 2019).
- In a study, published in Radiology (Yiming et al. 2018), AI was able to detect Alzheimer’s (ucsf.edu) disease in brain scans 6 years prior to diagnosis with 98% accuracy. Radiologists have used brain scans to try to detect Alzheimer’s by looking for reduced glucose levels across the brain. However, because the disease is a slow progressive disorder, the changes in glucose are very subtle and difficult to spot with the naked eye.
- In this study on cervical cancer (cancernetwork.com) by the National Cancer Institute's Division of Cancer Epidemiology and Genetics, AI was more accurate at identifying pre-cancer than a human expert reviewer of PAP tests under the microscope. The AI performed better than all standard screening methods at identifying cases of cervical cancer.
- Researchers at Osaka University used AI to analyse microscopic images to identify cancer cell types (photonics.com). Using a convolutional neural network based system they were able to automatically distinguish between different types of cancer cells. Being able to accurately identify cancer cells helps doctors choose the most effective treatment.
- Half a million women die every year from breast cancer. In a study led by researchers at UCSF and Mayo Clinic, computers equalled radiologists in assessing breast cancer risk (Fernandez 2018). This study was published May 1 2018, in the Annals of Internal Medicine (Kerlikowske et al. 2018)
- CardioLogs is a Paris-based startup building deep learning algorithms to analyse ECGs. Emergency room doctors used Cardiolog's algorithm and it outperformed the conventional algorithm for emergency department electrocardiogram interpretation (Stephen et al. 2019).
- Google has developed an AI system that can grade prostate cancer cells with 70% accuracy (venturebeat.com). This is important because human pathologists who grade prostate cancer cells disagree up to 53% of the time. According to the paper Development and Validation of a Deep Learning Algorithm for Improving Gleason Scoring of Prostate Cancer, the AI was 70% accurate whereas human pathologists were only 61% accurate (Kunal et al. 2018).
- Scientists at Stanford have developed a deep learning algorithm (news.stanford.edu) that can diagnose 14 types of heart rhythm defects, called arrhythmias, better than cardiologists. The algorithm, detailed in an arXiv paper, performs better than trained cardiologists, and has the added benefit of being able to sort through data from remote locations where people don’t have access to cardiologists (Pranav et al. 2017).
- Researchers at USC applied machine learning to measure changes linked to cardiovascular disease (viterbischool.usc.edu). Their study was published in Nature Scientific Reports (Tavallali et al. 2018).
- In a study published in Clinical Cancer Research, deep learning was used to analyse a large set of mammograms to distinguish images with malignant diagnosis from benign lesions (Wu et al. 2018). Deep learning distinguished recalled-benign mammograms from malignant and negative images. This study showed that there are imaging features unique to recalled-benign images that deep learning can identify to help radiologists in decision making to help reduce unnecessary recalls.
- Researchers at the Lawrence J. Ellison Institute for Transformative Medicine are developing a platform leveraging machine learning to analyse tissue samples to diagnose breast cancer and assess response to treatment (ellison.usc.edu).
- Samsung has applied its AI algorithms to assist diagnosis in each of its imaging modalities increasing the accuracy of diagnosis from 83% to 87% for doctors with four years or less experience (zdnet.com).
- A team at Stanford University used deep learning convolutional neural networks to reduce the dosage of gadolinium, a heavy metal used in contrast material for MRI that is often left in the body after an MRI exam (news-medical.net).
- In Mexico they are using an AI solution by Lunit INSIGHT for chest radiography and mammography (itij.com). It has an accuracy level of 97-99% for chest X-rays and 97% for mammography.
- Zebra Medical Vision AI algorithms help identify patients at risk of osteoporotic fractures and AI algorithms to help identify patients at risk of cardiac events (itnonline.com).
- In November 2018, the FDA cleared MaxQ AI Accipio Ix intracranial hemorrhage detection software. This software uses AI to detect brain bleeds (medgadget.com).
- In April 2018 the FDA approved marketing of the first medical device to use AI to detect the eye disease in adults who have diabetes. The software uses an AI algorithm to analyse images of the eye (fda.gov).
- The NIH and NVIDIA are developing AI tools to support clinical trials. The AI tools will provide precision medicine to patients with brain and liver cancers (beckershospitalreview.com).
- A team at Stanford developed an AI algorithm to help radiologists accurately diagnose MRI scans of knee injuries. Doctors diagnosed fewer false positives using the algorithm (scopeblog.stanford.edu).
- Bayer and Merck have won a breakthrough device designation from the FDA for software they are jointly developing. The software uses AI to analyse image findings from cardiac, lung perfusion and pulmonary vessels (pharmaphorum.com).
- Researchers at Imperial College London and Bayer Pharmaceuticals have formed a partnership to research using machine learning to analyse 3D heart imaging, genetic information, and health data to accelerate drug discovery for heart disease (imperial.ac.uk).
- A team at Massachusetts General Hospital in Boston is using AI to diagnose and classify brain haemorrhages using small image data sets. This AI system is as accurate in detecting and classifying intracranial haemorrhages as human radiologists (economictimes.indiatimes.com).
- The FDA has cleared IDx-DR, an AI diagnostic system used at the University of Iowa Hospitals and Clinics to AI to analyse images of the retina for signs of diabetic retinopathy. When the AI detects signs of diabetic retinopathy, the AI recommends a follow-up with an ophthalmologist. If it detects no signs of the condition, the system recommends a follow-up screening in one year (darkdaily.com). Another AI based diagnostic system for the detection of diabetic retinopathy, detailed in Nature, achieved 87.2% sensitivity and 90.7% specificity in the detection of diabetic retinopathy (Abramoff et al. 2018).
Key Points
- AI algorithms are sometimes more effective and efficient at identifying disease than human experts.
- AI will help increase access to care in places where radiologists are inaccessible
- AI will help improve workflow and efficiency
- Using AI to analyse medical images is the most efficient and cost effective way to screen and help diagnose many diseases and the impact would be huge
Next Article: Future of ultrasound: where are we going?
References:
Abramoff MD et al. (2018) Pivotal trial of an autonomous AI-based diagnostic system for detection of diabetic retinopathy in primary care offices. Digital Medicine 1(39). Available from nature.com/articles/s41746-018-0040-6
AI-Based System Uses Microscopic Images to Identify Cancer Cell Types (2018) Photonics Media. Available from photonics.com/Articles/AI-Based_System_Uses_Microscopic_Images_to/a64242
AI, doctors team up to improve, expedite diagnoses (2018) SCOPE. Available from scopeblog.stanford.edu/2018/11/27/ai-doctors-team-up-to-improve-expedite-diagnoses/
A.I. will equalize health care in China, NovaVision CEO says (2018) CNBC. Available from cnbc.com/2018/11/28/artificial-intelligence-will-equalize-healthcare-in-china-ceo-says.html
Artificial Intelligence Can Detect Alzheimer’s Disease in Brain Scans Six Years Before a Diagnosis (2019) UCSF. Available from ucsf.edu/news/2018/12/412946/artificial-intelligence-can-detect-alzheimers-disease-brain-scans-six-years
AI could reduce gadolinium dosage in MRI scans (2018) Stanford Medical. Available from news-medical.net/news/20181126/AI-could-reduce-gadolinium-dosage-in-MRI-scans.aspx
AI Promising in Predicting Chronic Conditions From CT Scans (2018). Imaging Technology News. Available from itnonline.com/content/ai-promising-predicting-chronic-conditions-ct-scans
Artificial intelligence rivals radiologists in screening X-rays for certain diseases (2018) Stanford Medicine. Available from med.stanford.edu/news/all-news/2018/11/ai-outperformed-radiologists-in-screening-x-rays-for-certain-diseases.html








