When hospital patients outside the ICU become unstable, many facilities have medical emergency teams (MET) in place to rapidly respond. But are events warranting MET calls more common in a radiology department (RD) than in a general ward? Lora Ott, PhD, RN, Assistant Professor, Indiana University of Pennsylvania, and colleagues have published the results of their research into this area in the Journal of Radiology Nursing. And the finding that such events are more common in the RD, when adjusted to length of stay, have led to increased awareness by imaging department staff of the potential for patient instability in the RD, Ott told HealthManagement.org. Previous research by Ott and colleagues found that risk factors for MET calls in the RD included being transported from a non-ICU, a greater number of comorbidities, and recent vital sign changes.
This study retrospectively analysed MET calls in 2009 in a U.S. tertiary hospital Rates were calculated as calls per hour per 1000 admissions, and adjusted for length of stay. Length of stay was calculated from patient transport data as time elapsed in hours from when the patient left the ward for the RD until return to the ward. For patients requiring a MET call, length of stay was time from leaving the ward until the MET call was made. The researchers also calculated MET calls for each imaging modality.
Results
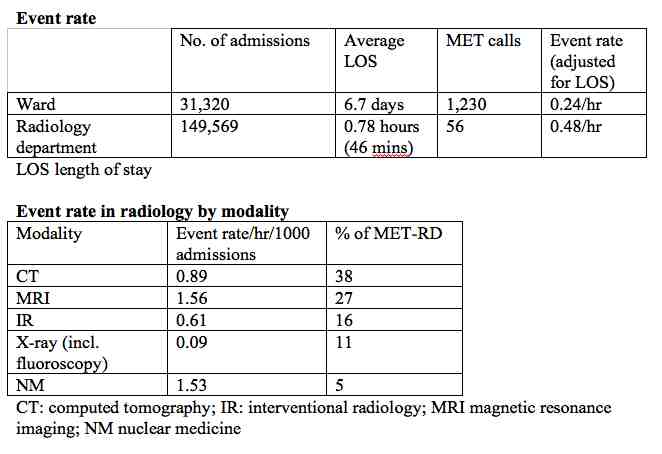
When events in the radiology department were analysed by modality, CT, MRI and IR rates ranged from 3.7 to 6.5 times higher than emergency calls on wards.
The researchers conclude that these findings suggest that radiology department patients are at increased risk for a medical emergency team call when time at risk is considered in comparison to patients on the ward. They recommend more study to find out the reasons for different event rates across modalities, and if increased patient surveillance would make a difference.
Dr. Ott noted in an email to HealthManagement.org that “the hospital has developed an "off monitor" protocol to give nurses more autonomy in the decision of whom to send off the hospital units without monitoring surveillance.” She added that there was “increased awareness that off unit travel was a potential patient safety risk and that patients were not being properly identified for nursing resources. The nurses in our imaging department are planning a QI project to prospectively track the use of this policy as it affects the patients who become unstable in radiology to determine if the decision tree is being properly implemented and to gain insight into its effectiveness.”
Claire Pillar
Managing editor, HealthManagement.org
Claire Pillar
Managing editor, HealthManagement.org
References:
Ott LK, Pinsky MR, Hoffman LA et al. (2012) Medical emergency team calls in the radiology department: patient characteristics and outcomes. BMJ Qual Saf, 21(6): 509-18.
Ott LK, Pinsky MR, Hoffman LA et al. (2015) Patients in the radiology department may be at increased risk of developing critical instability. J Radiol Nurs, 34(1): 29-34.
Ott LK, Pinsky MR, Hoffman LA et al. (2015) Patients in the radiology department may be at increased risk of developing critical instability. J Radiol Nurs, 34(1): 29-34.
Latest Articles
patient emergencies, radiology, CT, MRI, IR, RD, MET
When hospital patients outside the ICU become unstable, many facilities have medical emergency teams (MET) in place to rapidly respond. But are events warranting MET calls more common in a radiology department (RD) than in a general ward? Lora Ott, PhD, R