ICU Management & Practice, Volume 21 - Issue 2, 2021
During the first year, the ICU director should take a snapshot of the ICU situation and invest time and resources to acquire good and real data that will drive priorities of care and management. After that, implementation of basic protocols and creating a programme to engage and protect the staff against burnout should be considered. Finally, we suggest integrating research and educational activities into the ICU routine.
Introduction
The role of an Intensive Care Unit (ICU) director represents both a tremendous opportunity and a huge responsibility. One important question is “how to prioritise actions” in case you were promoted in your own institution or if you were hired and don’t know much about your new team and the new environment. In this brief review, we suggest top five priorities for a new ICU director during the first year.
A snapshot: institutional culture, your introduction, a diagnosis of ICU structure, staff, process and outcomes
The institutional culture can be defined as the purposes, actions and values that drive the organisation to meet their goals. It is crucial that as a new manager you understand the organisation’s culture and are aligned with these values. After that, if you decide to go ahead, it is important to introduce yourself to the team. A formal meeting to present your goals focusing on transparency and tangible objectives is recommended. If you are new in the institution it is important to use the first weeks to observe and learn about the environment, the unit’s business and to create connections with key stakeholders and others institutional leaders (inside and outside the ICU) (Nguyen 2018).
The next step is to take a snapshot of the ICU. A “Donabedian” approach of structure, process and outcomes is a good framework. First of all, evaluate if the ICU accomplishes the minimum requirements for critical care departments according to your local regulations. Several intensive care societies as well legislative documents (e.g., Brazil – RDC 7) were published in the last decade and should be used as a baseline (Brazilian Health Surveillance Agency 2010). This evaluation starts with a careful check of ICU design, size, availability of equipment as well as profile and quantitative evaluation of the multidisciplinary staff. During this initial evaluation, it is important to assess the operational routine and expansion capability and if the ICU team is responsible for critical ward patients in routine situations or in catastrophes or surges such as in the SARS-Cov2 pandemic (Aziz et al. 2020). Map the existing main processes of care and available patients’ outcomes. Try to understand current admission and discharge criteria, levels of care, nurse and physician patient ratio. The knowledge of your case-mix, current length of stay and mortality and ICU-acquired infection rates are the initial main concerns. Again, some national intensive care societies recommend key structure, process and outcome quality indicators (Rhodes et al. 2012). Table 1 presents a suggestion of the minimum quality indicators to create an ICU snapshot.
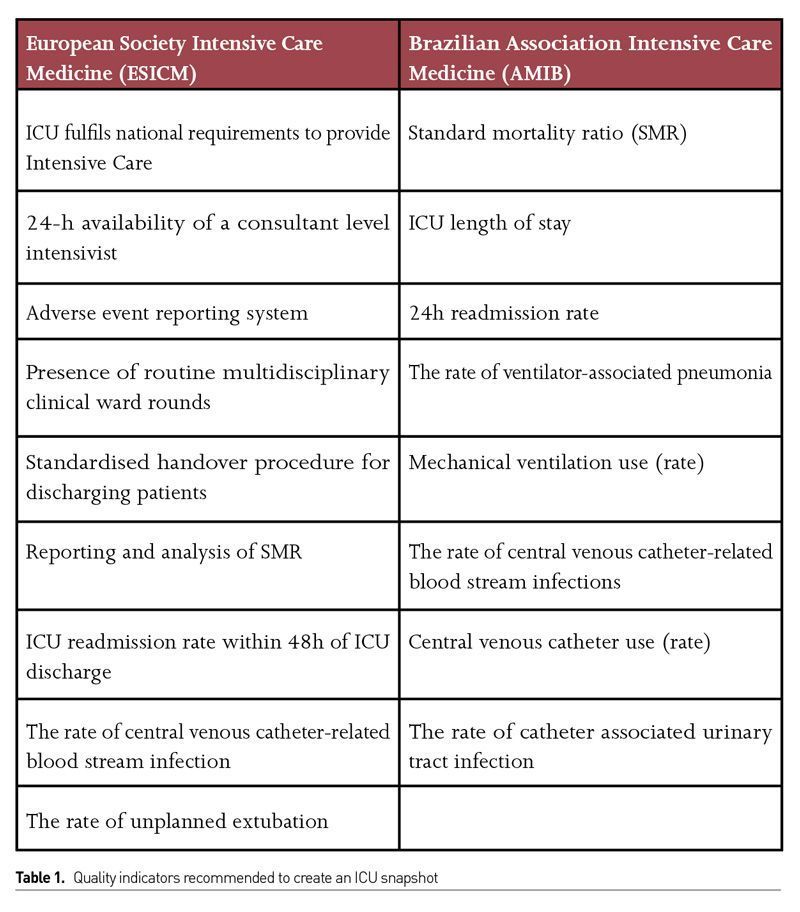
Create a minimum data-driven culture: establishing data collection and discussion based on data
A strong data driven culture is the foundation of modern ICU management. Although this statement may sound unattainable, there are several examples of widely implemented data-driven ICUs that rely on data abstraction and analysis as the basis of quality assurance and improvement (McClean et al. 2017, Zampieri et al. 2017).
The first step is to establish a core dataset and while it is tempting to cover all aspects of case-mix, outcomes and process of care, it may become an impossible task if attempted all at once. Thus, establish a core dataset based on local regulations for quality of care (Flaatten 2012) or on a well-established set of indicators such as those proposed by Rhodes (Rhodes et al. 2012). The use of electronic platforms for data entry, especially if coupled with integration with the electronic medical record (EMR) and other data sources, is a key factor to ensure timely and secure data entry (Zampieri et al. 2017). If the ICU has already an established model and database, focusing on the traditional “Donabedian” approach allows insightful analysis of efficiency and case-mix based on indicators of structure, process and outcomes (Salluh et al. 2017). Once the dataset and indicators are defined, it is crucial to democratise access to data. At this point, data availability (through online dashboards and printed reports available to the team) should be inserted in the routine of the ICU. Discussing results in specific sessions is useful, however, even more useful is to illustrate the daily rounds and patients’ cases with data from the ICU. This becomes a source of reflection and quality improvement for the team. The discussion of “actionable indicators”, i.e. usually those associated with process of care measures that can be modified by increasing the adherence to evidence-based practices, is particularly thought-provoking (Roos-Blom et al. 2015; Salluh et al. 2018). When local indicators are compared to benchmarks from top performing ICUs or the recommendations from guidelines, this allows ICU managers to use data to induce an audit-feedback loop. In this loop, data obtained from audits in the ICU are measured against benchmarks and discussed within the context of a particular patient situation (i.e. - non-adherence to DVT prophylaxis or low tidal volume ventilation) or a failure to achieve a local ICU indicator (i.e. - VAP rates or elevated SMRs or SRUs indicated lower efficiency). This can start a virtuous cycle of quality improvement that may be shaped with the PDSA (Plan, Do, Study and Act) approach.
Identifying and selecting the basic protocols for treatment and prevention
One of the responsibilities, as the new head of the ICU, is to ensure patient safety and deliver the best care. In order to accomplish this in a coordinated and sustainable way, the development and implementation of protocols are essential. The main objective of clinical protocols is to achieve a reduction of care variability. This is associated with better outcomes; and the simplification of complex tasks, which may be hindered by poorly defined workflows. Additionally, it is worth pointing out that changes always start by changing the structure and processes of care (Sinuff et al. 2013).
In order to begin protocol implementation, it is necessary to understand the case-mix and outcomes of the ICU as well as the team that will deliver the care. Besides that, it is important to identify institutional and sectorial clinical protocols already in execution and their results (Kerlin et al. 2021).
After this initial evaluation, one should define the stages of implementation of a protocol, as it will facilitate the process. As a recommendation, these stages must contemplate: a literature review about the issue; identification and the involvement of all stakeholders; a draft of the process, describing each stage and its goal; definition of indicators and results; a training plan; and the disclosure of metrics achieved for the team, which will allow for the reevaluation of possible points, thus generating improvement cycles. The perfect balance is found when the ICU does not reinvent the wheel, but rather tailors existing evidence-based medicine recommendations to fit the ICU’s case-mix and workflow.
Some general protocols are applicable to most ICUs and cause a huge impact on the clinical outcomes. We suggest the following protocols:
- Analgesia, sedation and delirium protocol: it is known that excessive use of sedatives is responsible for longer periods of mechanical ventilation and higher rates of healthcare-associated infections (HAI) that negatively impacts clinical outcomes (Brook et al. 1999);
- Alarm adjustment protocol: several adverse events occur in ICUs, either due to inadequate monitoring or alarm fatigue, therefore having an established routine of adjustments and actions mitigates failures and increases patient safety;
- Orotracheal intubation protocol: airway management is one of the most critical procedures in intensive care. Having a described protocol that preferably uses a safety checklist considerably decreases the odds of adverse events in this context;
- HAI prevention protocol: the infections resulting from the use of invasive devices (i.e. central venous catheter) are preventable most of the time, mainly due to unnecessary and prolonged use (Pronovost et al. 2006);
- Weaning from mechanical ventilation protocol: liberating the patient from ventilatory support has to be one of the main goals of the team. In order for this to be safe and performed at the right clinical moment, it is fundamental to prepare the team (Krishnan et al. 2004).
Caring for those who care: staff management, professional development, burnout avoidance
Assess the work conditions of your staff, develop an integration programme for the new members and create a continuum medical education programme with scientific meetings and simulation training, ICU quality and safety indicators, and morbimortality meetings.
Career development is important to keep and engage new talents. Try to understand the real situation and create a plan to avoid staff turnover. Regularly conduct individual feedback meeting to understand their interests and ambitions. Identify faculty with more interests in academic research, management, quality and safety. The job in ICU allows a lot of “Y” career development options (Figure 1). An individual programme development could help staff to identify the area that they have more interest.
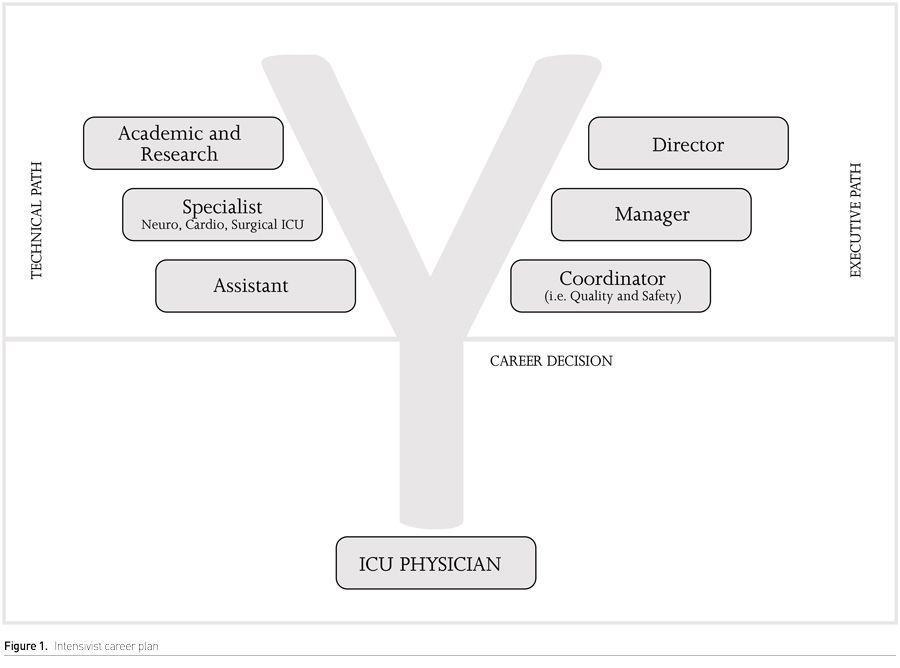
The routine work in ICU demands from ICU staff technical knowledge and soft skills (i.e. communication, negotiation, resilience). Despite technical training most of ICU staff do not have a formal soft skills education. In the last years several studies demonstrated high levels of burnout, anxiety and depression among ICU workers (Merlani et al. 2011). The recent SARS-CoV-2 has had a devastating psychological impact on intensivists and increased the psychological burden for ICU staff. Evaluate the emotional and engagement of ICU staff and map the foremost problems to develop a plan to support and alleviate the stress (Azoulay et al. 2020).
At the end of your first year with more information about your unit and staff, prepare a meeting with clinical champions and other leaders to create a strategic plan for the next three years.
Advanced management: integrating teaching and research into the ICU routine
The challenge of integrating teaching and research into the ICU routine is to conciliate these activities with evolving demands to provide safe and high-quality care. Intensive care physicians face time pressure, high volume of patients, increasing demand for patient satisfaction scores, and administrative responsibilities daily (Joyce et al. 2017).
Bedside teaching is one of the most frequently used methods for medical training, despite the lack of a clear standardised approach to critical care education (Santhosh et al. 2018). Thus, the instructor characteristics and competencies have to receive considerable attention. The member of the support staff who leads the process has a key role in determining the success of clinical teaching in the ICU routine. Residents and fellows have a tendency to mirror the behaviour of instructors they feel are professional and competent (Natesan et al. 2020). Organisational aspects and process of care can impact the clinical management and also are important for consideration. Ensuring the application of evidenced-based practices and standardised process of care are closely link to good clinical teaching (Natesan et al. 2020).
Strategies for increasing efficiency and effectiveness in ICU education have been described, including tips for teaching under time pressure (Joyce et al. 2017, Santhosh et al. 2018). It is worth mentioning that some practical approaches can be incorporated into the routine without disrupting workflow or compromising the safety and quality of patient care (Joyce et al. 2017). ICU rounds, the application of ICU checklists, invasive procedures, handover and family communications can be used for teaching practices. The participation of the entire team in the ICU rounds ensuring the application of protocols and checklists represents a learning opportunity, and can improve teamwork, safety climate (Writing Group for Brazilian Research in Intensive Care et al. 2016) and is associated with improved patient outcomes (Kim et al. 2010, Soares et al. 2015).
The involvement of multidisciplinary team is also important to research (Francois et al. 2016). The principal investigator may not have enough time to complete all essential tasks. Sharing responsibilities with all ICU care providers is a way to incorporate clinical research as a part of daily routine care. Nurses, residents, fellows or any other healthcare worker willing to participate can be involved in the inclusions, monitor interventions and events. Specific training, local research meetings and effective communication are strategies to ensure motivation and commitment (Francois et al. 2016).
Conclusion
The role of an ICU director comes with many challenges. Being able to address these challenges is essential to create a safe and healthy working environment. The introduction and development of a data-driven culture and clinical research is recommended as it is associated with increased ICU efficiency, improved patient outcomes and staff satisfaction.
Conflict of Interest
Dr da Silva Ramos, Dr Pacheco, Dr Freitas and Dr Machado report no conflicts of interest. Dr Salluh is founder and holder at Epimed Solutions, the provider of a cloud-based healthcare analytics and performance evaluation software.
References:
Aziz S, Arabi YM, Alhazzani W et al. (2020) Managing ICU surge during the COVID-19 crisis: rapid guidelines. Intensive Care Med., 46(7):1303-1325.
Azoulay E, De Waele J, Ferrer R et al. (2020) Symptoms of burnout in intensive care unit specialists facing the COVID-19 outbreak. Ann Intensive Care, 10(1):110.
Brazilian Health Surveillance Agency (2010) Resolutionution Nº 7. Available from bvsms.saude.gov.br/bvs/saudelegis/anvisa/2010/res0007_24_02_2010.html.
Brook AD, Ahrens TS, Schaiff R et al. (1999) Effect of a nursing-implemented sedation protocol on the duration of mechanical ventilation. Crit Care Med., 27(12):2609-2615.
Flaatten H (2012) The present use of quality indicators in the intensive care unit. Acta Anaesthesiol Scand., 56(9):1078-1083.
Francois B., Clavel M, Vignon P et al. (2016) Perspective on optimizing clinical trials in critical care: how to puzzle out recurrent failures." J Intensive Care, 4:67.
Joyce MF. Berg S, Bittner EA (2017) Practical strategies for increasing efficiency and effectiveness in critical care education. World J Crit Care Med., 6(1):1-12.
Kerlin MP, Costa DK, Kahn JM (2021) The Society of Critical Care Medicine at 50 Years: ICU Organization and Management. Crit Care Med., 49(3):391-405.
Kim MM, Barnato AE, Angus DC et al. (2010) The effect of multidisciplinary care teams on intensive care unit mortality. Arch Intern Med., 170(4):369-376.
Krishnan JA, Moore D, Robeson C et al. (2004) A prospective, controlled trial of a protocol-based strategy to discontinue mechanical ventilation. Am J Respir Crit Care Med., 169(6):673-678.
McClean K, Mullany D, Huckson S et al. (2017) Identification and assessment of potentially high-mortality intensive care units using the ANZICS Centre for Outcome and Resource Evaluation clinical registry. Crit Care Resusc., 19(3):230-238.
Merlani P, Verdon M, Businger A et al. (2011) Burnout in ICU caregivers: a multicenter study of factors associated to centers. Am J Respir Crit Care Med., 184(10):1140-1146.
Natesan S, Bailitz J, King A et al. (2020) Clinical Teaching: An Evidence-based Guide to Best Practices from the Council of Emergency Medicine Residency Directors. West J Emerg Med., 21(4):985-998.
Nguyen HB, Thomson CC, Kaminski N et al. (2018) Leadership Primer for Current and Aspiring Pulmonary, Critical Care, and Sleep Medicine Academic Division Chiefs. Ann Am Thorac Soc., 15(6):655-661.
Pronovost P, Needham D, Berenholtz S et al. (2006) An intervention to decrease catheter-related bloodstream infections in the ICU. N Engl J Med., 355(26):2725-2732.
Rhodes A, Moreno RP, Azoulay E et al. (2012) Prospectively defined indicators to improve the safety and quality of care for critically ill patients: a report from the Task Force on Safety and Quality of the European Society of Intensive Care Medicine (ESICM). Intensive Care Med., 38(4):598-605.
Roos-Blom MJ, Dongelmans D, Arbous MS et al. (2015) How to Assist Intensive Care Units in Improving Healthcare Quality. Development of Actionable Quality Indicators on Blood use. Stud Health Technol Inform., 210:429-433.
Salluh JIF, Chiche JD, Reis CE et al. (2018) New perspectives to improve critical care benchmarking. Ann Intensive Care, 8(1):17.
Salluh JIF, Soares M, Keegan MT (2017) Understanding intensive care unit benchmarking. Intensive Care Med., 43(11):1703-1707.
Santhosh L, Brown W, Ferreira J et al. (2018) Practical Tips for ICU Bedside Teaching. Chest, 154(4):760-765.
Sinuff T, Muscedere J, Adhikari NK et al. (2013) Knowledge translation interventions for critically ill patients: a systematic review. Crit Care Med., 41(11):2627-2640.
Soares M, Bozza FA, Angus DC et al. (2015) Organizational characteristics, outcomes, and resource use in 78 Brazilian intensive care units: the ORCHESTRA study. Intensive Care Med., 41(12):2149-2160.
Writing Group for the, C.-I. C. U. I., N. the Brazilian Research in Intensive Care, Cavalcanti AB, Bozza FA, Machado FR et al. (2016) Effect of a Quality Improvement Intervention With Daily Round Checklists, Goal Setting, and Clinician Prompting on Mortality of Critically Ill Patients: A Randomized Clinical Trial. JAMA, 315(14):1480-1490.
Zampieri FG, Soares M, Borges LP et al. (2017) The Epimed Monitor ICU Database(R): a cloud-based national registry for adult intensive care unit patients in Brazil. Rev Bras Ter Intensiva, 29(4):418-426.











