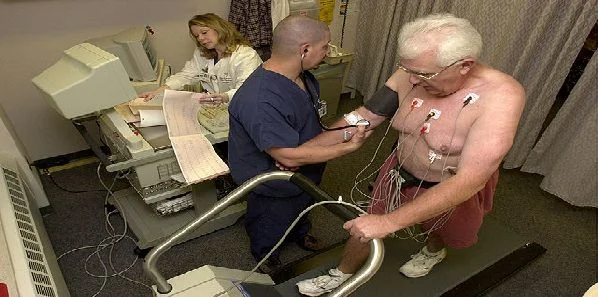
Researchers from the New York University Langone Medical Center (New York, NY, USA) found that overuse of cardiac stress testing using advanced imaging technology has led to increasing healthcare costs in the US and unnecessary radiation exposure for patients. Their study, believed to be the first comprehensive investigation of trends in cardiac stress testing utilising imaging, also showed that there are no significant racial or ethnic health disparities in its use. Results of the study have been published in Annals of Internal Medicine.
Cardiac stress testing with imaging has been the focus of debate about inappropriate use, patient safety in the context of radiation exposure and rising healthcare costs. The research team, led by Joseph Ladapo, MD, PhD, assistant professor in the departments of medicine and population health at NYU Langone, sought to determine whether US trends in cardiac stress testing with imaging may be attributable to population shifts in demographics, risk factors, and provider characteristics. They also assessed whether racial/ethnic discrepancies exist in physician decision making.
The team examined data from the US National Ambulatory Medical Care Survey (NAMCS) and US National Hospital Ambulatory Medical Care Survey (NHAMCS) from 1993 to 2010. Patients included in the study were adults without coronary heart disease who were referred for cardiac stress tests. The study's key findings include:
The authors concluded the national growth in cardiac stress testing can be attributed mostly to population and provider characteristics, but the use of imaging cannot. They also noted that physician decision making about cardiac stress testing does not result in racial/ethnic disparities in cardiovascular disease.
Cardiac stress testing is an important clinical tool, said Dr. Ladapo, “but we are over using imaging for reasons unrelated to clinical need." This is causing preventable harm and increasing healthcare costs, he emphasised. "We estimate that about 500 people get cancer each year in the US from radiation received during a cardiac stress test when, in fact, they most probably didn’t need any radiological imaging in the first place. While this number might seem relatively small, we must remember that 'first, do no harm' is one of the guiding principles in medicine.”
When unnecessary cardiac stress testing with imaging is reduced, this will also decrease the incidence of radiation related cancer. Dr. Ladapo therefore suggested greater use of stress testing without radiological imaging, such as regular exercise treadmill tests or stress testing with ultrasound imaging as opposed to CT [computed tomography] imaging. “More efforts, such as clinical decision support, are needed to reduce unnecessary cardiac stress testing,” the doctor explained.
As to why specific racial and ethnic minorities have poorer rates of treatment for cardiovascular disease and generally have poorer cardiovascular health outcomes compared to white patients, Dr. Ladapo noted that no one has really explored whether there could be disparities in cardiac stress testing, which is a mainstay of diagnosing patients with heart disease in this country. “Perhaps one contributing reason they have poorer outcomes is because we are not testing them appropriately,” he said.
Source: MedImaging.net
Image Credit: Wikimedia Commons
Cardiac stress testing with imaging has been the focus of debate about inappropriate use, patient safety in the context of radiation exposure and rising healthcare costs. The research team, led by Joseph Ladapo, MD, PhD, assistant professor in the departments of medicine and population health at NYU Langone, sought to determine whether US trends in cardiac stress testing with imaging may be attributable to population shifts in demographics, risk factors, and provider characteristics. They also assessed whether racial/ethnic discrepancies exist in physician decision making.
The team examined data from the US National Ambulatory Medical Care Survey (NAMCS) and US National Hospital Ambulatory Medical Care Survey (NHAMCS) from 1993 to 2010. Patients included in the study were adults without coronary heart disease who were referred for cardiac stress tests. The study's key findings include:
- Between 1993–1995 and 2008–2010, the yearly number of ambulatory visits in the US in which a cardiac stress test was prescribed or performed rose by more than 50 percent.
- Cardiac stress tests with imaging comprised a rising percentage of all of these tests, increasing from 59 percent in 1993–1995 to 87 percent in 2008–2010. At least 34.6 percent (one million tests) were probably inappropriate, the researchers concluded, with associated annual costs of $501 million and 491 future cases of cancer.
- There was no evidence of a lower likelihood of black patients receiving a cardiac stress test with imaging (odds ratio, 0.91 [95 percent CI, 0.69 to 1.21]) than their white counterparts; however, some slight evidence of disparity in Hispanic patients was found (odds ratio, 0.75 [CI, 0.55 to 1.02]).
The authors concluded the national growth in cardiac stress testing can be attributed mostly to population and provider characteristics, but the use of imaging cannot. They also noted that physician decision making about cardiac stress testing does not result in racial/ethnic disparities in cardiovascular disease.
Cardiac stress testing is an important clinical tool, said Dr. Ladapo, “but we are over using imaging for reasons unrelated to clinical need." This is causing preventable harm and increasing healthcare costs, he emphasised. "We estimate that about 500 people get cancer each year in the US from radiation received during a cardiac stress test when, in fact, they most probably didn’t need any radiological imaging in the first place. While this number might seem relatively small, we must remember that 'first, do no harm' is one of the guiding principles in medicine.”
When unnecessary cardiac stress testing with imaging is reduced, this will also decrease the incidence of radiation related cancer. Dr. Ladapo therefore suggested greater use of stress testing without radiological imaging, such as regular exercise treadmill tests or stress testing with ultrasound imaging as opposed to CT [computed tomography] imaging. “More efforts, such as clinical decision support, are needed to reduce unnecessary cardiac stress testing,” the doctor explained.
As to why specific racial and ethnic minorities have poorer rates of treatment for cardiovascular disease and generally have poorer cardiovascular health outcomes compared to white patients, Dr. Ladapo noted that no one has really explored whether there could be disparities in cardiac stress testing, which is a mainstay of diagnosing patients with heart disease in this country. “Perhaps one contributing reason they have poorer outcomes is because we are not testing them appropriately,” he said.
Source: MedImaging.net
Image Credit: Wikimedia Commons
Latest Articles
CT, Imaging, Radiation, Cardiovascular, cardiac stress test
Researchers from the New York University Langone Medical Center (New York, NY, USA) found that overuse of cardiac stress testing using advanced imaging tec...