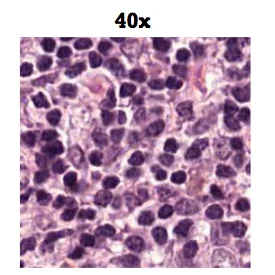
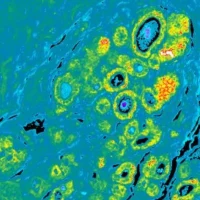
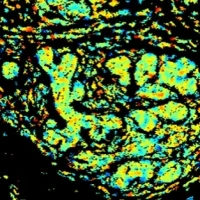
A combination of the decades-long practice of diagnosing illnesses by manually reviewing images under a microscope and artificial intelligence (AI), can help doctors improve accuracy of breast and other cancer diagnosis to a rate of 99.5 percent.
A research team from Beth Israel Deaconess Medical Center (BIDMC) in Boston and Harvard Medical School (HMS) recently developed AI methods aimed at training computers to interpret pathology images, with the long-term goal of building AI-powered systems to make pathologic diagnoses more accurate.
“Our AI method is based on deep learning, a machine-learning algorithm used for a range of applications including speech recognition and image recognition,” explained pathologist Andrew Beck, MD, PhD, Director of Bioinformatics at the Cancer Research Institute at BIDMC and an Associate Professor at Harvard Medical School.
The Beck lab’s approach was recently put to the test in a competition held at the annual meeting of the International Symposium of Biomedical Imaging (ISBI), which involved examining images of lymph nodes to decide whether or not they contained breast cancer. The research team of Beck and his lab’s post-doctoral fellows placed first in two separate categories, competing against private companies and academic research institutions from around the world. The research team posted a technical report describing their approach to the arXiv.org repository, an open access archive of e-prints in physics, mathematics, computer science, quantitative biology, quantitative finance and statistics.
“Peering into the microscope to sift through millions of normal cells to identify just a few malignant cells can prove extremely laborious using conventional methods. We thought this was a task that the computer could be quite good at – and that proved to be the case,” said Beck.
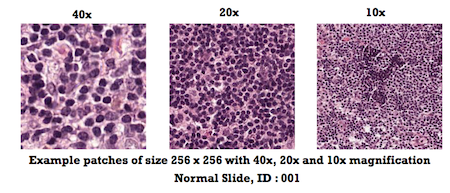
In an objective evaluation in which researchers were given slides of lymph node cells and asked to determine whether or not they contained cancer, the team’s automated diagnostic method proved accurate approximately 92 percent of the time, that nearly matched the success rate of a human pathologist, whose results were 96 percent accurate.
“But when we combined the pathologist’s analysis with our automated computational diagnostic method, the result improved to 99.5 percent accuracy,” said Beck. “Combining these two methods yielded a major reduction in errors.”
The team trained the computer to distinguish between cancerous tumour regions and normal regions based on a deep multilayer convolutional network.
“There have been many reasons to think that digitising images and using machine learning could help pathologists be faster, more accurate and make more accurate diagnoses for patients,” Beck added.
Jeroen van der Laak, PhD, who leads a digital pathology research group at Radboud University Medical Center in the Netherlands and was an organiser for the competition, said, “when we started this challenge, we expected some interesting results. The fact that computers had almost comparable performance to humans is way beyond what I had anticipated. It is a clear indication that artificial intelligence is going to shape the way we deal with histopathological images in the years to come.”