The number of
thymic tumour patients is increasing rapidly in Japan because of the abundance
of computed tomography (CT) scanners in the country that makes the examination
easily accessible, as a result of which the prevalence of this condition is now
better recorded.
Speaking on diagnostic imaging of thymic tumours at the “ESR Meets Japan” symposium during the European Congress of Radiology (ECR2016) in Vienna, Professor Noriyuki Tomiyama from the Graduate School of Medicine, Osaka University, said that surgeries of thymic carcinoma have increased five-fold, from 500 in 1986 to 2,500 today.
He said that the Japanese Association for Research on the Thymus (JART) is in research cooperation with the International Thymic Malignagy Group (ITMIG), a body headed by Prof Frank Detterbeck of Yale University, that aims to promote the advancement of clinical and basic science pertaining to thymic and other mediastinal malignancies and related conditions.
Tomiyama said that the three areas of interest are thymic cyst, thymoma and thymic carcinoma.
Progress in thymic malignancies has been slow, according to ITMIG. Although a few centres are recognised for their experience in thymic conditions, there has been a general sense that because little is known about these diseases, it is acceptable for a physician with very limited experience to do whatever he or she thinks is best when treating an occasional patient.
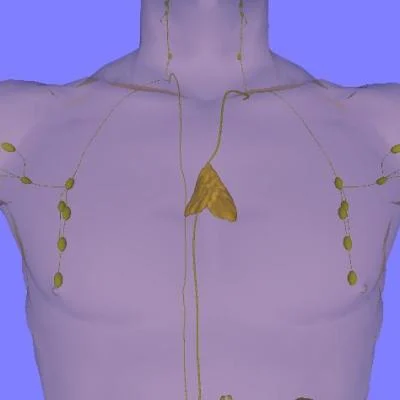
The thymus is a specialised primary lymphoid organ of the immune system. It is composed of two identical lobes and is located anatomically in the anterior superior mediastinum, in front of the heart and behind the sternum.
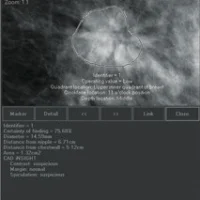
“The differences between CT and magnetic resonance imaging (MEI) is that CT produces higher detection results in thymic carcinoma, while the MR results high on thymic cysts,” Tomiyama said.
“The most important thing we need to find out is if that is a true tumour or a cyst. Sometimes it is difficult to differentiate by using CT alone, so, I think we should be using MR more.”
“If we find a small thymoma, should we continue and proceed with surgery? It is also easier for us to treat a big thymoma, but if we find a small thymoma of less than 1cm we seem to have difficulty on how to manage them,” Tomiyama concluded.
The thymus is largest and most active during the neonatal and pre-adolescent periods and two primary forms of tumours originate in the thymus:
Thymomas – the thymic epithelial cells are found in 10-15 percent of patients with myasthenia gravis where symptoms are sometimes confused with bronchitis or a strong cough.
Lymphomas – originating from the thymocytes occur in people with an enlarged thymus, particularly children, who were treated with intense radiation in the years before 1950.
Surgical thymectomy for the removal of the thymus is conducted to gain access to the heart for surgery to correct congenital heart defects in the neonatal period. In neonates, but not older children or adults, the relative size of the thymus obstructs surgical access to the heart. Removal of the thymus in infancy results in immunodeficiency by some measures.