A multicentre study finds that early noninvasive ventilation, compared with oxygen therapy alone, did not reduce the risk of 28-day mortality among immunocompromised patients admitted to the ICU with hypoxaemic acute respiratory failure. The study is published by JAMA to coincide with its presentation at the 28th annual congress of the European Society of Intensive Care Medicine.
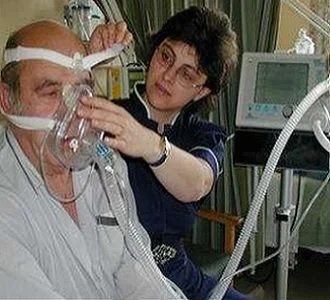
Noninvasive ventilation has been recommended to decrease mortality among immunocompromised patients with hypoxaemic (inadequate oxygenation of the blood) acute respiratory failure. The current study aimed to assess the effectiveness of this intervention in this type of patient population.
Elie Azoulay, MD, PhD, of Saint-Louis University Hospital, Paris, and colleagues had 374 critically ill immunocompromised patients randomly assigned to early noninvasive ventilation (n = 191) or oxygen therapy only (n = 183). Of these patients, 317 (85 percent) were receiving treatment for haematologic malignancies or solid tumours. The trial was conducted at 28 ICUs in France and Belgium. On day 28 after randomisation:
“In this multicentre randomised trial enrolling critically ill immunocompromised patients with acute respiratory failure, early noninvasive ventilation, compared with oxygen therapy alone, did not reduce the primary outcome of day-28 all-cause mortality, either overall or in any of the prespecified subgroups,” the authors write. “However, study power was limited.”
In an accompanying editorial, Bhakti K. Patel, MD, and John P. Kress, MD, of the University of Chicago, write: “With additional efforts to continue to reduce the percentage of critically ill patients who require invasive mechanical ventilation, alternative strategies for noninvasive ventilation that minimise face mask leak, improve oxygenation, and decrease work of breathing with alternative interfaces such as high-flow nasal cannula will need further investigation.”
Source: JAMA
Image credit: SlideShare
Noninvasive ventilation has been recommended to decrease mortality among immunocompromised patients with hypoxaemic (inadequate oxygenation of the blood) acute respiratory failure. The current study aimed to assess the effectiveness of this intervention in this type of patient population.
Elie Azoulay, MD, PhD, of Saint-Louis University Hospital, Paris, and colleagues had 374 critically ill immunocompromised patients randomly assigned to early noninvasive ventilation (n = 191) or oxygen therapy only (n = 183). Of these patients, 317 (85 percent) were receiving treatment for haematologic malignancies or solid tumours. The trial was conducted at 28 ICUs in France and Belgium. On day 28 after randomisation:
- 46 deaths (24 percent) had occurred in the noninvasive ventilation group vs. 50 (27 percent) in the oxygen group.
- Oxygenation failure occurred in 155 patients overall (41 percent), 38 percent in the noninvasive ventilation group and 45 percent in the oxygen group.
- There were no significant differences in ICU-acquired infections, duration of mechanical ventilation, or lengths of ICU or hospital stays.
“In this multicentre randomised trial enrolling critically ill immunocompromised patients with acute respiratory failure, early noninvasive ventilation, compared with oxygen therapy alone, did not reduce the primary outcome of day-28 all-cause mortality, either overall or in any of the prespecified subgroups,” the authors write. “However, study power was limited.”
In an accompanying editorial, Bhakti K. Patel, MD, and John P. Kress, MD, of the University of Chicago, write: “With additional efforts to continue to reduce the percentage of critically ill patients who require invasive mechanical ventilation, alternative strategies for noninvasive ventilation that minimise face mask leak, improve oxygenation, and decrease work of breathing with alternative interfaces such as high-flow nasal cannula will need further investigation.”
Source: JAMA
Image credit: SlideShare
References:
Azoulay E et al. (2015) Effect of Noninvasive Ventilation vs Oxygen Therapy on Mortality Among Immunocompromised Patients With Acute Respiratory Failure: A Randomized Clinical Trial. JAMA. Published online
October 07, 2015. doi: 10.1001/jama.2015.12402
Patel BK, Kress JP (2015) The Changing Landscape of Noninvasive Ventilation in the Intensive Care Unit. JAMA. Published online October 07, 2015. doi: 10.1001/jama.2015.12401
Patel BK, Kress JP (2015) The Changing Landscape of Noninvasive Ventilation in the Intensive Care Unit. JAMA. Published online October 07, 2015. doi: 10.1001/jama.2015.12401
Latest Articles
healthmanagement, acute respiratory failure, critically ill, oxygen therapy, oxygenation, mortality
A multicentre study finds that early noninvasive ventilation, compared with oxygen therapy alone, did not reduce the risk of 28-day mortality among immunocompromised patients admitted to the ICU with hypoxaemic acute respiratory failure.