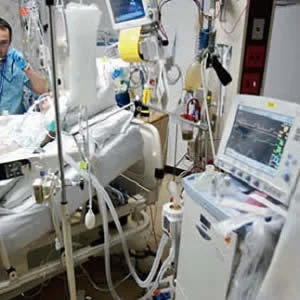
Mechanical ventilation is a life-saving strategy for critically ill patients. However, it can promote and/or exacerbate lung injury through several mechanisms, including alveolar overdistension and repetitive opening and closing of the alveoli and small airways. Positive end-expiratory pressure (PEEP) has been employed to prevent end-expiratory alveolar collapse and counteract mechanical strain. However, excessive PEEP can also worsen mechanical stress, leading to haemodynamic impairment.
Patients with ARDS are more at risk of ventilator-induced lung injury (VILI). The use of higher PEEP is associated with reduced mortality in patients with moderate to severe ARDS and those who respond better to the application of PEEP compared to patients with mild ARDS. Patients without ARDS may be exposed to increased risk of PEEP-related lung overdistension and haemodynamic compromise.
Evidence from the RELAx study suggests that a mechanical ventilation strategy using lower PEEP is non-inferior to a higher PEEP strategy in terms of ventilator-free days in patients without ARDS. However, another meta-analysis showed that higher levels of PEEP were not associated with lower in-hospital mortality or shorter duration of ventilation.
A systematic review and meta-analysis was conducted to assess the association of higher PEEP as opposed to lower PEEP, with hospital mortality in adult intensive care unit patients undergoing invasive mechanical ventilation for reasons other than ARDS.
Researchers identified 22 randomised clinical trials comparing higher PEEP with lower PEEP. Studies were published between 1975 and 2020. The patient population ranged from 15 to 969 patients. 10 studies enrolled post-cardiac surgery patients, six studies included patients with acute respiratory failure, four studies recruited patients with brain injuries and two studies included non-hypoxaemic patients.
Findings of the analysis show no statistically significant association between higher PEEP and hospital mortality. 284 patients out of 760 patients assigned to the higher PEEP group and 259 patients assigned to the lower PEEP groups died in the hospital. Higher PEEP was associated with better oxygenation, higher respiratory system compliance and lower risk of hypoxaemia and ARDS occurrence. In both groups, the length of stay, mortality in the ICU, barotrauma, hypotension and duration of ventilation were similar.
These findings show that higher PEEP compared with lower PEEP was not associated with mortality in patients without ARDS receiving invasive mechanical ventilation.
Source: Critical Care
Image Credit: Rcp.basheer