ICU Management & Practice, Volume 17 - Issue 2, 2017
This article reviews the current evidence on prognostication after cardiac arrest.
Post-resuscitation care has developed and evolved significantly since 2003, following recommendations by the Advanced Life Support task force of the International Liaison Committee on Resuscitation to implement therapeutic hypothermia (TH) in unconscious survivors following out-ofhospital cardiac arrest (OHCA) (Nolan et al. 2003). The 2015 European Resuscitation Council (ERC) and European Society of Intensive Care Medicine (ESICM) guidelines on post-resuscitation care made strong recommendations to avoid severe hyperoxia (large amounts of oxygen) for patients following cardiac arrest (CA). This was primarily based on the evidence that severe hyperoxia is associated with increased in-hospital mortality (Kilgannon et al. 2011) and decreased survival to discharge (Elmer et al. 2015). Supplemental oxygen in absence of hypoxia is also associated with increased early myocardial injury and a large myocardial infarct size assessed at six months (Stub et al. 2015).
The ERC-ESICM guidance also recommended emergency cardiac catheterisation and immediate percutaneous coronary intervention for adult patients with return of spontaneous circulation (ROSC) after OHCA of suspected cardiac origin and ST segment elevation on the electrocardiogram (ECG) (Nolan et al. 2015). A large randomised control trial demonstrated no additional benefit in survival following TH at 33°C to targeted temperature management (TTM) of 36°C following CA (Nielsen et al. 2013). However, the current ERC-ESIM guidance strongly recommends temperature management between 32°C-36°C. These recommendations were reinforced to decrease the pathological and clinical impact caused by CA, known as ‘Post-Cardiac Arrest Syndrome’ (Nolan et al. 2008).
The four key components of Post-Cardiac Arrest Syndrome were identified as:
I. Post-cardiac arrest brain injury;
II. Post-cardiac arrest myocardial dysfunction;
III. Systemic ischaemic / reperfusion injury;
IV. Persisting precipitating pathology.
Despite advances in post-resuscitation care management, about 50% of resuscitated patients from CA die or have a poor neurological prognosis. One of the major causes of mortality following CA is severe neurological damage due to post-anoxic brain injury (Sandroni and Nolan et al. 2015;). It is therefore essential to have a prognostication model that can predict poor neurological outcome and enable physicians to consider early withdrawal of life supporting treatment.
The Quality Standards Subcommittee of the American Academy of Neurology published a review in 2006 on prediction of neurological outcome in the comatose patient following CA (Wijdicks et al. 2006). However, the patients included in this review did not undergo TH or TTM, which was recommended subsequently. In 2015, ERC-ESICM recommended a multimodal prognostication approach for comatose survivors following CA (Sandroni et al. 2014).
Prognostication Strategy
At the recently concluded annual 37th International Symposium on Intensive Care and Emergency Medicine (ISICEM), Brussels, experts, who presented and published original studies on post-resuscitation care, explained their strategies in the workshop, Prognostication in post-anoxic brain damage: my strategy (37th ISICEM)
The key principles to follow are:
• early communication with the family
• delay prognostication
• multimodal evaluation, and
• be patient.
Early Communication
It is essential that rapport and a good relationship is established with the next of kin or family members at the earliest opportunity. There should be attempts to provide meaningful information and for them to be made aware of the critical nature of the patient’s medical condition. This will also aid physicians to understand the expectations and goals of family members or patients. There should be regular interaction and it is vital for the family to understand that physicians will make the decision.
Delay Prognostication
The current evidence supports the practice of first assessment after 72 or 24 hours, depending on whether patients received or did not receive temperature control management, respectively. This will help guide further management, and further prognostication can be carried out 24-48 hours later. However, the phenomenon of ‘late awakening’ has been described; there is a small subset of patients who will defy the 5-7 day recovery period and may wake up late and will have full neurological recovery. This is where the experience of the treating physician comes into action.
Multimodal Evaluation
The modalities for evaluation were described in the 2013 review (Sandroni et al. 2013) and are as follows:
I. Clinical examination (brainstem reflex, motor response, myoclonus);
II. Electrophysiology (burst suppression, seizures, flat or low amplitude electroencephalogram (EEG), non-reactive EEG, EEG grading, somato-sensory evoked potential (SSEP));
III. Biochemical markers (neuron-specific enolase (NSE), S-100B);
IV. Brain imaging (computed tomography (CT), magnetic resonance imaging (MRI)). It will be even more effective if this is performed by an intensivist alongside a neurologist.
Be Patient
This attribute is key and it is important to have a process. The process involves looking at all the previously described pre-, peri- and post-arrest factors, and continuous delivery of timely optimal care. It is therefore vital to be patient and to follow this process over a period of a week, even if there is no obvious visual recovery in the patient.
In 2014, an advisory statement on prognostication in comatose survivors following CA was published by the ERC and the ESICM (Sandroni et al. 2014). This statement updated and summarised the available evidence on this topic including that of TH-treated patients. The robust analysis of evidence provided practical recommendations on the most reliable prognostication strategies, and formed the basis of the ERC guidelines on resuscitation published in 2015.
The key recommendations are summarised below:
1. Clinical examination
• Using the bilateral pupillary and corneal reflexes at 72 h or more from ROSC to predict poor outcome in comatose survivors from cardiac arrest, either TH or non-TH treated patients;
• Prolonging observation of clinical signs beyond 72 h when interference from residual sedation or paralysis is suspected, so that the possibility of obtaining false positive results is minimised;
• Not to use absent or extensor motor response to pain (M ≤ 2) alone to predict poor outcome as it has a high false-positive rate; it should be used in combination with other robust predictors.
2. Myoclonus and status myoclonus
• Using the term status myoclonus to indicate a continuous and generalised myoclonus persisting > 30 mins in comatose survivors of CA;
• Using the presence of a status myoclonus within 48 h from ROSC in combination with other predictors to predict poor outcome in comatose survivors of CA, either TH or non-TH treated;
• Evaluate patients with post-arrest status myoclonus off sedation whenever possible.
3. Bilateral absence of SSEP N20 wave
• Using bilateral absence of SSEP N20 wave at ≥72 h from ROSC to predict outcome in comatose survivors following CA treated with controlled temperature;
• There was suggestion to use SSEP at ≥ 24 h from ROSC to predict outcome in comatose survivors following CA not treated with controlled temperature.
4. Electroencephalogram (EEG)
• Absence of EEG reactivity to external stimuli, presence of burst suppression or status epilepticus at ≥ 72 h after ROSC to predict poor outcome in comatose survivors from CA;
• They should be used in combination along with other predictors as this criteria lacks standardisation and does not have very strong evidence.
5. Biomarkers
There is suggestion to use high NSE at 48-72 h from ROSC in combination with other predictors for prognosticating a poor neurological outcome in comatose survivors following CA, either TH or non-TH treated. However, no threshold enabling prediction with zero false-postive results can be recommended. Utmost care and preferably multiple sampling should be employed to avoid false positive results due to haemolysis.
6. Imaging
Using the presence of a marked reduction in grey matter/white matter ratio or sulcal effacement on brain CT within 24 hours after ROSC or presence of the extensive reduction in diffusion on brain MRI at 2-5 days after ROSC to predict a poor outcome in comatose survivors following CA both TH or non-TH treated. The brain CT or MRI should be used in combination with other predictors and only at centres where specific experience is available.
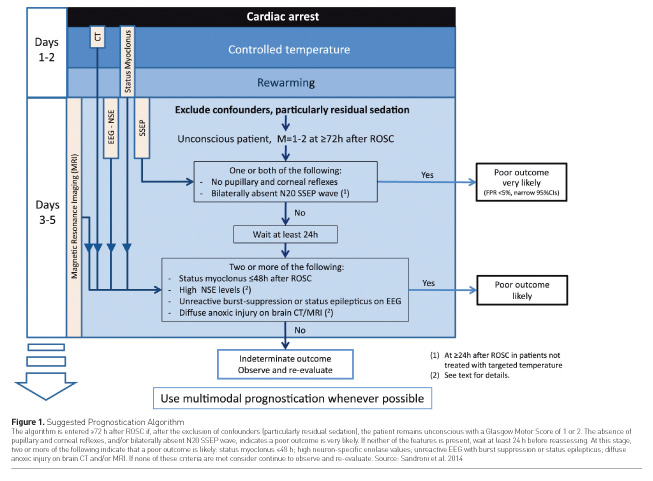
Figure 1 (Sandroni et al. 2014) suggests a prognostication algorithm approach. Point-of-Care Focused Echocardiography In a recent systematic review (Tsou et al. 2017), a total of 1695 patients in CA had point-of-care (POC) focused echocardiography performed during resuscitation. The study concluded POC focused echocardiography can be used to identify reversible causes and predict short-term outcome in patients with CA. In patients with a low pretest probability for ROSC, absence of spontaneous cardiac movement on echocardiography can predict a low likelihood of survival and guide the decision of resuscitation termination. It is very early to consider focused echocardiography, and it is currently not a part of prognostication strategies.
Conclusion
The current evidence suggests a delayed (post 72 h), multimodal prognostication approach for unconscious survivors who receive postresuscitation care following cardiac arrest.
Conflict of Interest
Mena Farag declares that he has no conflict of interest. Shashank Patil declares that he has no conflict of interest.
Abbreviations
CA cardiac arrest
ECG electrocardiogram
EEG electroencephalogram
ERC European Resuscitation Council
ESCIM European Society of Intensive Care Medicine
NSE neuron-specific enolase
OHCA out-of-hospital cardiac arrest
ROSC return of spontaneous circulation
SSEP somatosensory evoked potential
TH therapeutic hypothermia
TTM targeted
temperature management
References:
37th International Symposium on Intensive Care and Emergency Medicine. Square - Brussels Meeting Centre. March 21-24, 2017.
Elmer J, Scutella M, Pullalarevu R et al. (2015) The association between hyperoxia and patient outcomes after cardiac arrest: analysis of a high-resolution database. Intensive Care Med, 41 (1): 49-57.
Kilgannon JH, Jones AE, Shapiro NI et al. (2010) Association between arterial hyperoxia following resuscitation from cardiac arrest and in-hospital mortality. JAMA, 303 (21): 2165-71.
Nielsen N, Wetterslev J, Cronberg T et al. (2013) Targeted temperature management at 33°C versus 36°C after cardiac arrest. N Engl J Med, 369 (23): 2197-206.
Nolan JP, Morley PT, Vanden Hoek TL et al. (2003) Therapeutic hypothermia after cardiac arrest: an advisory statement by the advanced life support task force of the International Liaison Committee on Resuscitation. Circulation, 108 (1): 118-21.
Nolan JP, Neumar RW, Adrie et al. (2008) Postcardiac arrest syndrome: epidemiology, pathophysiology, treatment, and prognostication. A Scientific Statement from the International Liaison Committee on Resuscitation; the American Heart Association Emergency Cardiovascular Care Committee; the Council on Cardiovascular Surgery and Anesthesia; the Council on Cardiopulmonary, Perioperative, and Critical Care; the Council on Clinical Cardiology; the Council on Stroke. Resuscitation, 79 (3): 350-79.
Nolan JP, Soar J, Cariou A et al. (2015) European Resuscitation Council and European Society of Intensive Care Medicine 2015 guidelines for post-resuscitation care. Intensive Care Med, 41 (12): 2039-56.
Sandroni C, Cavallaro F, Callaway CW et al. (2013) Predictors of poor neurological outcome in adult comatose survivors of cardiac arrest: a systematic review and meta-analysis. Part 2: Patients treated with therapeutic hypothermia. Resuscitation, 84(10): 1324-38.
Sandroni C, Cariou A, Cavallaro F et al. (2014) Prognostication in comatose survivors of cardiac arrest: an advisory statement from the European Resuscitation Council and the European Society of Intensive Care Medicine. Intensive Care Med, 40 (12): 1816-31.
Sandroni C, Nolan JP (2015) Neuroprognostication after cardiac arrest in Europe: new timings and standards. Resuscitation, 90: A4-5.
Stub D, Smith K, Bernard S et al. (2015) Air versus oxygen in ST-segment-elevation myocardial infarction. Circulation, 131(24): 2143-50.
Tsou PY, Kurbedin J, Chen YS et al. (2017) Accuracy of point-of-care focused echocardiography in predicting outcome of resuscitation in cardiac arrest patients: A systematic review and metaanalysis. Resuscitation, 114: 92-9.
Wijdicks EF, Hijdra A, Young GB et al. (2006) Practice parameter: prediction of outcome in comatose survivors after cardiopulmonary resuscitation (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology, 67 (2): 203-10.








