ICU Management & Practice, Volume 21 - Issue 1, 2021
COVID-19 patients present to the hospital with lung involvement and interstitial pneumonia eventually associated with lung collapse. The clinical picture is dominated by severe hypoxaemia without dyspnoea/tachypneoa and normal respiratory mechanics; this condition has been defined as silent hypoxia. The picture may evolve, and these patients may present with severe refractory hypoxaemia associated with dyspnoea/tachypnoea, use of accessory muscles of respiration, and respiratory mechanics impairment.
Silent hypoxia is linked to the mechanism of dyspnoea. Dyspnoea occurs due to a perceived mismatch between the outgoing efferent signals from the respiratory centre to the ventilatory muscles and incoming afferent signals from the lungs and the chest wall to the respiratory centre. These afferent signals may be triggered by hypercapnia or severe hypoxaemia, airway and interstitial inflammation and impaired lung mechanics. COVID-19 patients can have impairment of lung function, both at the alveolar level and at the intravascular level but a very low level of oxygenation (as low as 30 mmHg) needs to be reached to have dyspnoea, which is mediated by an increase in CO2, in minute ventilation and in the effort to breathe. In the beginning, patients can be treated with simple oxygen therapy followed by mechanical respiratory support as needed (Dhont et al. 2020).
Goals of Mechanical Respiratory Support in COVID-19 Patients
The most important goals of mechanical respiratory support are:
• To improve oxygenation
• To support the respiratory muscles
• To prevent additional lung injury
Noninvasive Support and Guidelines in Hypoxaemic Acute Respiratory Failure
Besides standard oxygenation techniques, different forms of non-invasive support can be used in hypoxaemic patients. These include Nasal High Flow (NHF), continuous positive airway pressure (CPAP), and non-invasive positive pressure ventilation (NIPPV). NHF delivers high gas flow and is a technique that can increase the airway pressure and can generate a positive end-expiratory pressure (PEEP). With CPAP, a single value of airway pressure is set and this pressure is usually higher than that provided by NHF. With NIPPV two levels of pressure are set: the lowest is maintained during expiration and the highest is reached during inspiration to support the respiratory muscles.
COVID-19 is a new disease. The ERS/ATS clinical practice guidelines for use of noninvasive ventilation in hypoxaemic acute respiratory failure should be referred to when dealing with this patient population. Several studies show conflicting results, and overall there is no effect of NIV on mortality. Given the uncertainty of evidence, the guidelines state that it was not possible to offer any reccomendation about the use of NIPPV in hypoxaemic patients (Rochwerg et al. 2017).
Results of a recent meta-analysis may further help to guide NIPPV use in hypoxaemic patients, including those with COVID-19. Findings show that, as compared with standard oxygen, NIPPV may reduce mortality, particularly when it is delivered with helmet. As compared with both face mask NIPPV and NHF, helmet NIPPV might give better results, thus being preferable in patients with hypoxaemic respiratory failure (Ferreyro et al. 2020).
New guidelines were released regarding the use of NHF in hypoxaemic respiratory failure. Based on the results of the meta-analysis, the panel gave a strong recommendation for the use of NHF compared to standard oxygenation in these patients (Rochwerg et al. 2020).
There are risks associated with noninvasive respiratory support. These include:
• Environmental contamination
• Intubation delay
• Patient self-inflicted lung injury, due to high respiratory drive (Brochard et al. 2017).
Sedation and Analgesia During NIPPV
Sedation can manipulate respiratory drive, typically very high in COVID-19 patients, when breathing spontaneously. However, it is important to remember that the results of using analgosedation are not always positive. A study by Muriel et al. (2015) suggests that compared to no sedation, use of analgesia, sedation or both was associated with an increase in NIPPV failure and 28-day mortality. Therefore, sedation in COVID-19 patients during NIPPV is not recommended, especially because many of these patients may not have dyspnoea. If the patient’s condition worsens, the only solution is to use intubation and invasive mechanical ventilation.
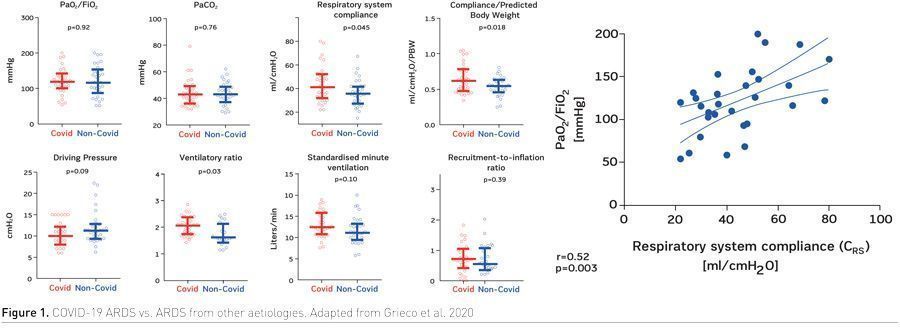
COVID-19 ARDS vs. ARDS From Other Aetiologies
It is being debated if COVID-19 ARDS is similar to traditional ARDS or different. At the beginning of the pandemic, these data were not available, but more data have been produced since then. In a study by Grieco et al. (2020), 30 patients with moderate to severe COVID-19 related ARDS were matched with 30 other patients with ARDS from other aetiologies. All patients were studied within 24 hours from intubation. Two PEEP levels were applied – 5 and 15 cmH20 to assess the response of these patients to PEEP and lung recruitability.
Several parameters were compared between COVID-19 and non-COVID-19 patients (Figure 1). From a clinical point of view, all measured parameters, including gas exchange, compliance, driving pressure, ventilatory ratio (a measure of deadspace), minute ventilation and the recruitment-to-inflation ratio (a measure of recruitability), were similar in COVID-19 and non-COVID-19 patients, although compliance and ventilatory ratio were statistically higher in COVID-19 patients. It is important to note that all these parameters showed a high variability both in COVID-19 and in non-COVID-19 patients. In COVID-19 patients, a direct correlation was also observed between compliance and oxygenation. Because compliance is an index of lung aeration, this correlation indicates that oxygenation improved with improving lung aeration, as it has been described in traditional ARDS (Grieco et al. 2020).
As far as response to PEEP is concerned, the results were similar in both COVID-19 and non-COVID-19 cohorts. High-level PEEP improved oxygenation in both cohorts. There was a similar response in terms of ventilatory ratio, compliance and driving pressure in both cohorts. High PEEP resulted in a greater improvement of oxygenation in COVID-19 patients compared to traditional ARDS, but the improvement in oxygenation was not related to the index of recruitability. Recruitability was correlated to a decrease in PCO2. Overall, findings from this study show that after the establishment of mechanical ventilation, patients with COVID-19 show a conventional ARDS phenotype (heterogeneity in respiratory mechanics, aeration loss related to the degree of hypoxaemia and inter-individually variable recruitability) and that clinicians treating COVID-19 patients should adhere to recent guidelines regarding standard ARDS management (Grieco et al. 2020).
These findings have been confirmed by another study conducted in 301 COVID-19 ARDS patients who were compared to 2634 traditional ARDS patients. In both groups, compliance was highly variable and values were very similar from a clinical perspective, although slightly higher in COVID-19 patients. Total lung weight was also similar. Authors also described lung thrombo-embolic events in COVID-19 patients, particularly when high compliance was associated with high levels of D-dimers, and these thrombo-embolic phenomena have been described also in traditional ARDS. Study authors concluded that patients with COVID-19 associated ARDS have a form of injury that, in many aspects, is similar to that of those with ARDS unrelated to COVID-19 (Grasselli et al. 2020).
Protective Ventilation in COVID-19 ARDS
Following the previous reasoning, it is important, also in COVID-19 related ARDS, to follow the official clinical practice guidelines of the American Thoracic Society (ATS), European Society of Intensive Care Medicine (ESICM), and Society of Critical Care Medicine (SCCM) (Fan et al. 2017), for the management of mechanical ventilation in ARDS, which recommend:
- To use low tidal volume (4-8 ml/kg PBW) and low plateau pressures (<30 cmH20)
- To use prone position in severe ARDS (>12 h/day) and suggest to use higher PEEP and recruitment manoeuvres in moderate-severe ARDS.
However, it is important to individualise ventilation strategies in both traditional and COVID-19 ARDS patients. This should be done taking into consideration the risks associated with aggressive mechanical ventilation, including shear stress, overdistention, or increase in intrathoracic pressure, which can further injure the lung and have been linked to the spillover of bacteria and inflammatory mediators from the lung into systemic circulation. This can cause damage to the distal organs leading to multi-organ failure (Slutsky and Tremblay 1998).
In fact, it is known that aggressive mechanical ventilation can have harmful effects on the patient. For example, a Brazilian study compared the use of an aggressive ventilator strategy, with lung recruitment manoeuvres and a high PEEP level, in patients with ARDS to a low/moderate PEEP level strategy. Findings from this study show that aggressive mechanical ventilation was associated with increased mortality and an increase in complications like pneumothorax, barotrauma and shock, suggesting that an aggressive mechanical ventilation strategy may have deleterious effects also at the cardiovascular level (Cavalcanti et al. 2017).
Sedation may be useful to limit another risk of mechanical ventilation, that is patient ventilator dyssynchrony. If there is a mismatch between the patient's breath and ventilator-assisted breaths, and the ventilator's flow delivery does not match the patient's flow demand, it can generate a dyssynchrony, i.e. double cycling, which can have a negative impact on the patient. This can be managed by sedation while ensuring no oversedation or undersedation.
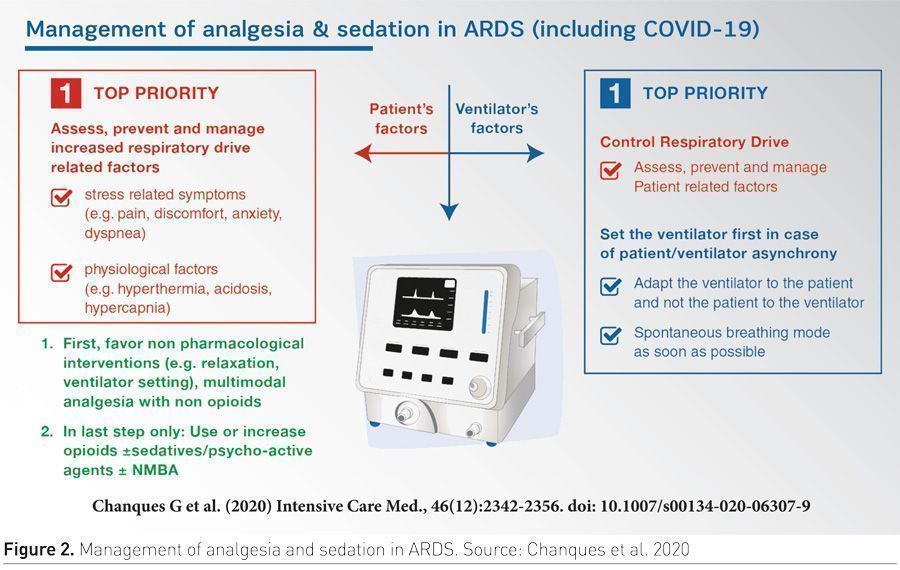
There is a relationship between ventilatory management and sedation management. A recent review of analgesia and sedation management in ARDS, including patients with COVID-19, highlights the importance of optimising sedation. As per this review, the most important priorities are to manage increased respiratory drive, and to optimise ventilation to avoid ventilator dyssynchrony (Chanques et al. 2020).
In conclusion, the primary reasons for sedation in COVID-19 patients include improving patient comfort (pain, anxiety and dyspnoea), enhancing patient safety (during special manoeuvres such as proning), facilitating lung-protective mechanical ventilation, and treating ventilator dyssynchrony by controlling the respiratory drive. Also, aims of sedation in all ARDS patients, including those with COVID-19, are to maintain patient interaction with staff and family and to promote early physical and cognitive recovery.
Key Points
- NIPPV should be applied on an individual basis when managing COVID-19 patients, paying attention not to delay intubation if required.
- Sedation during NIPPV is generally not needed in COVID-19 patients.
- Patients with COVID-19 show a conventional ARDS phenotype and should be treated using guidelines regarding standard ARDS management.
- There is a relationship between ventilatory management and sedation management and the priorities should be to manage increased respiratory drive, to optimise ventilation and to avoid ventilator dyssynchrony.
References:
Brochard L et al. (2017) Mechanical Ventilation to Minimize Progression of Lung Injury in Acute Respiratory Failure. Am J Respir Crit Care Med.,15;195(4):438-442.
Chanques G et al. (2020) Analgesia and sedation in patients with ARDS. Intensive Care Med.,46(12):2342-2356.
Dhont S et al. (2020) The pathophysiology of 'happy' hypoxemia in COVID-19. Respir Res., 21(1):198.
Fan E et al. (2017) American Thoracic Society, European Society of Intensive Care Medicine, and Society of Critical Care Medicine. An Official American Thoracic Society/European Society of Intensive Care Medicine/Society of Critical Care Medicine Clinical Practice Guideline: Mechanical Ventilation in Adult Patients with Acute Respiratory Distress Syndrome. Am J Respir Crit Care Med., 195(9):1253-1263.
Ferreyro BL et al. (2020) Association of Noninvasive Oxygenation Strategies With All-Cause Mortality in Adults With Acute Hypoxemic Respiratory Failure: A Systematic Review and Meta-analysis. JAMA.324(1):57–67.
Grasselli G et al. (2020) Pathophysiology of COVID-19-associated acute respiratory distress syndrome: a multicentre prospective observational study. Lancet Respir Med., 8(12):1201-1208.
Grieco DL et al. (2020) Respiratory physiology of COVID-19-induced respiratory failure compared to ARDS of other etiologies. Crit Care 24, 529.
Muriel A et al. (2015) Impact of sedation and analgesia during noninvasive positive pressure ventilation on outcome: a marginal structural model causal analysis. Intensive Care Med 41:1586–1600.
Rochwerg B et al. (2017) Official ERS/ATS clinical practice guidelines: noninvasive ventilation for acute respiratory failure. Eur Respir J., 31;50(2):1602426. doi: 10.1183/13993003.02426-2016.
Rochwerg B et al. (2020) The role for high flow nasal cannula as a respiratory support strategy in adults: a clinical practice guideline. Intensive Care Med 46, 2226–2237
Slutsky AS, Tremblay LN (1998) Multiple system organ failure. Is mechanical ventilation a contributing factor? Am J Respir Crit Care Med.,157(6 Pt 1):1721-5.
Writing Group for the Alveolar Recruitment for Acute Respiratory Distress Syndrome Trial (ART) Investigators, Cavalcanti AB et al. (2017) Effect of Lung Recruitment and Titrated Positive End-Expiratory Pressure (PEEP) vs Low PEEP on Mortality in Patients With Acute Respiratory Distress Syndrome: A Randomized Clinical Trial. JAMA, 318(14):1335-1345.







