What to Expect in Civilian vs. Military Contexts
Civilian blast injuries are not rare, but most are not due to military explosives, meaning extrapolation from military texts is often inappropriate. In civilian mass casualty events, emergency departments will see large patient numbers, but few require surgery or intensive care. Survivors of small civilian blasts rarely have blast wave injury and should be treated according to standard trauma principles.
Blast injuries are uncommonly encountered in civilian practice, but equally are not rare. For example, in the United States from 1983-2002, 36,110 civilian bombing incidents were reported (Kapur et al. 2005). The most common intent was homicide, not terrorism. Nonetheless, between 1991-2000, there were 29 worldwide terrorist attacks in which there were >30 casualties (Arnold 2004). Dwarfing numbers of criminal incidents, but less easily quantifiable, are accidental burns that involve a component of blast (for example from exploding fuel-air mixtures). Frequently, but erroneously, civilian clinicians turn to military texts (such as the Combat Casualty Care textbook (Savitsky and Eastridge 2012)), or are misled by civilian news sources that sometimes seek to sensationalise incidents. For example, an initial report in the New York Post of the 2013 Boston marathon bombing claimed “12 dead and nearly 50 injured” (Christopher 2013) —atypical for an open air blast. In reality only three were killed, but 264 were wounded, which conforms to historical data. Mistaken preconceptions of the medical consequences of blast can lead planners and managers to allocate resources incorrectly, and clinicians to focus attention away from the most likely pathology.
Blast Mechanisms of Injury
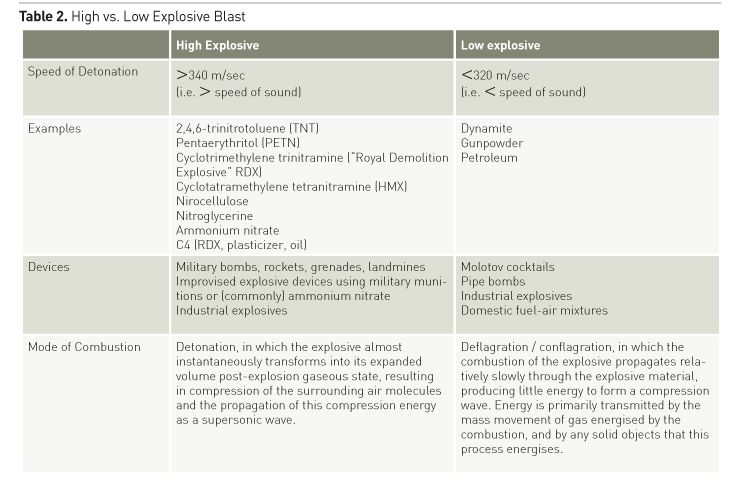
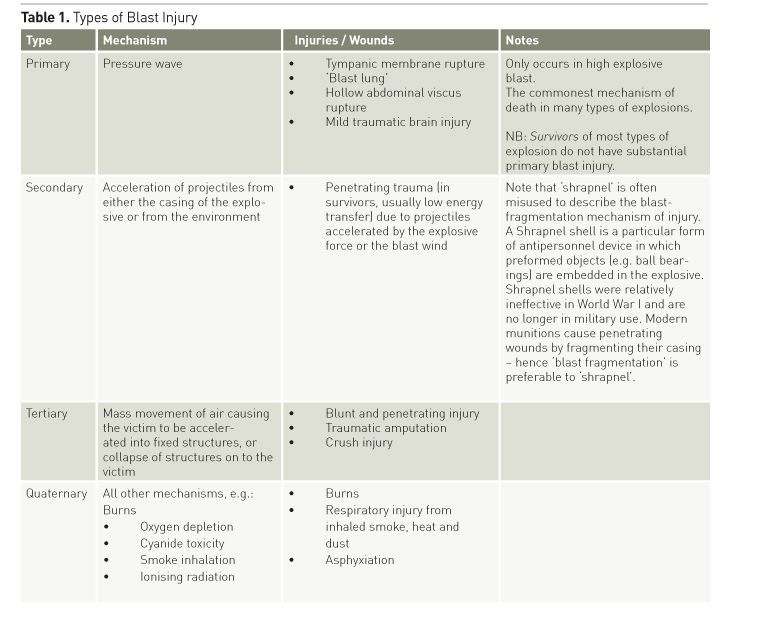
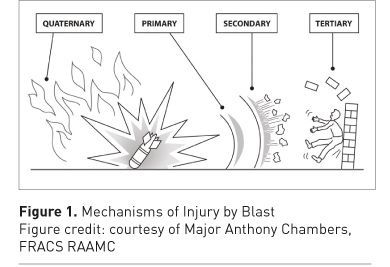
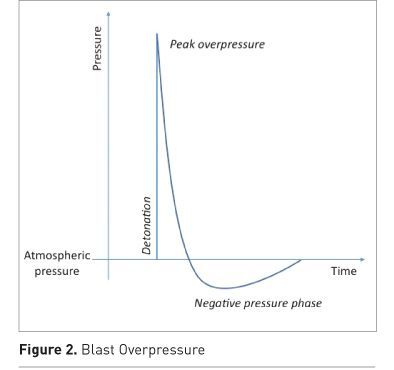
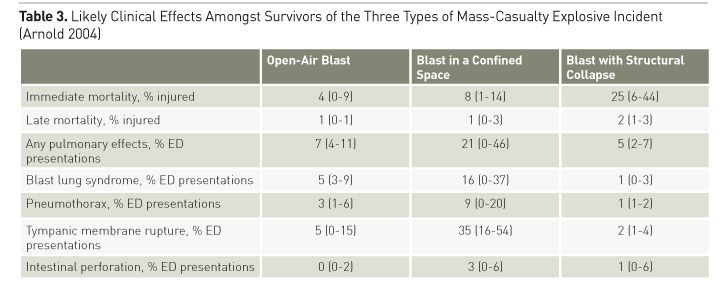
Table 1 and Figure 1 show the traditional classification of blast injuries. Primary blast injury is caused by a high-energy pressure wave. As measured at a single static point, the wave causes an abrupt increase, then decrease, in atmospheric pressure (see Figure 2). Like an ocean wave, there is no mass movement of gas; rather the peak pressure moves while the air molecules stay relatively static. In contrast, the ‘blast wind’ involves mass movement of gases away from the point of explosion, following the pressure wave by an appreciable delay. ‘High explosive’ blast is defined as one that causes a supersonic (>340m/sec) pressure wave (see Table 2). Energy intensity dissipates according to the cube of the distance from the blast. The pressure wave can be reflected from solid surfaces, so explosions in closed environments cause more primary blast injury, as shown in Table 3. The potential of the pressure wave to cause injury is a function of its intensity, duration and the orientation of the victim. Military body armour offers no protection to the blast wave. Water propagates a blast wave more efficiently than air, while retarding energised fragments, meaning that underwater explosions are unique in causing injury entirely by primary blast. A particular type of ‘enhanced’ atmospheric blast involves a prolonged overpressure wave. This increases the chance of primary blast injury, even if exposed in the open. The military application is the thermobaric or fuel-air explosive, in which a vapour cloud of explosive is dispersed by an initial charge and ignited by a second. When they occur in an industrial context, these situations are the exception to the general rule that civilian open-air explosions rarely cause primary blast injury in survivors. Combustion of air/dust mixtures in grain storage silos or coal storage buildings, and boiling liquid-expanding vapour explosions (BLEVEs), which occur upon release of gases stored as liquids under pressure at temperatures above their boiling points (such as might occur when a liquefied petroleum gas (LPG) bottle is engulfed in fire), both mimic thermobaric munitions.
The relationship between blast intensity and effect is well characterised (e.g. in Gibson 1994), but the details are more relevant to weapons engineers than clinicians, as there is almost never sufficient data available upon which to predict injury patterns. The most important points for clinicians are:
a. low energy blast, such as that which accompanies most civilian explosive-burn injuries (see Table 2), does not cause primary blast injury.
b. to suffer primary blast injury from a high explosive device, it is necessary:
i. to be very close to the explosion, or
ii. be the victim of an ’enhanced’ blast, or
iii. be exposed to an underwater blast, or
iv. be in a confined space that reflects the overpressure wave.
Most victims in the open who are sufficiently close to the explosion to experience a primary blast effect will die almost immediately.
c. Patients exposed to the same blast event at similar distances may have very different injury patterns, depending on the orientation of their bodies to the blast.
Penetrating ballistic injuries in survivors of blast are usually low energy, causing tissue damage by laceration and crushing rather than the cavitation of high-energy gunshot wounds. Glass debris commonly causes penetrating injuries in urban environments. Injury to multiple body locations is typical. Eye damage is particularly common (10%) (Centers for Disease Control and Prevention 2003), and early on may be overlooked if the eyes are not examined.
Pathogenesis of Primary Blast Injury
Blast pressure waves establish shear forces at tissues of different densities — with the greatest effects at the air-tissue interfaces of the lung, tympanic membrane and gastrointestinal tract. Other than bodily disruption, the arterial gas emboli caused by shear forces at the alveolar-capillary barrier are the main cause of very early death (from stroke or myocardial infarction). Survivors may develop ‘blast lung’, typically 24-72 hours after exposure, which is clinically indistinguishable from other causes of ARDS. Pneumothorax and haemothorax are also common. The tympanic membrane is even more sensitive to blast, but the influence of head orientation at the time of injury makes this an unreliable screening tool for pulmonary injury: in one study tympanic membrane disruption was present in only 50% of patients with other significant blast injury (Harrison et al. 2009). Gastrointestinal blast injury presents as delayed (up to 14 days) bowel rupture due to ischaemic necrosis. Mild traumatic brain injury is common after high explosive blast (59% in a U.S. military series (Savitsky and Eastridge 2012)), and, while less in civilian trauma (36% in a series of 89), was frequently missed (in 36% of patients who presented with a Glasgow Coma Scale (GCS) of 15) (Bochicchio et al. 2008).
Epidemiology of Civilian Blast Events: Implications for Planning and Response
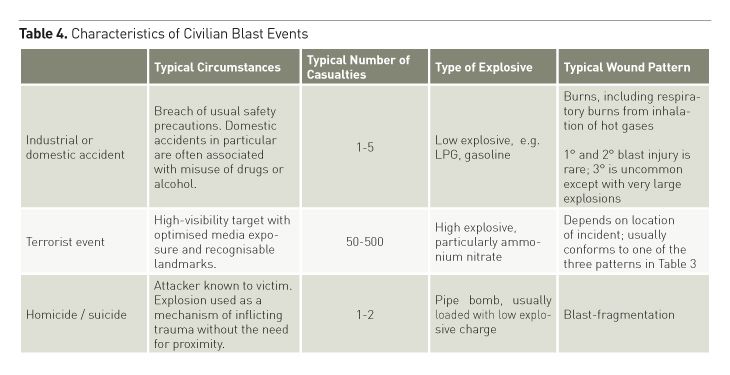
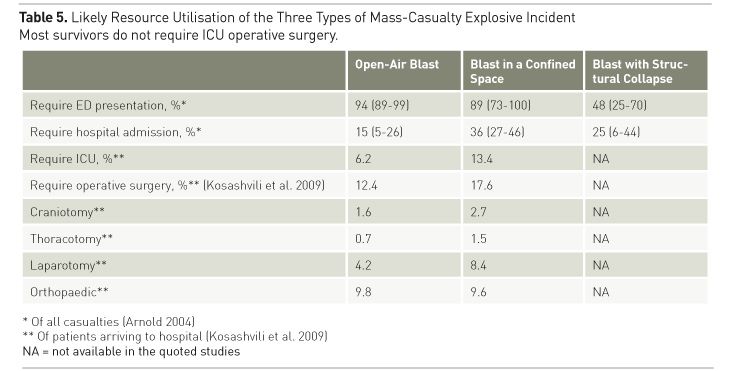
Civilian blast trauma occurs in one of three main patterns (see Table 4). Terrorist explosions injure few people compared to explosive accidents. Most victims either die almost immediately, or do not have life-threatening injuries; only 10-15% require life-saving interventions (Savitsky and Eastridge 2012). The immediate mortality of terrorist blast involving structural collapse (such as the Oklahoma City bombing in 1995, which killed 168 and injured 680) is high (typically 25%; see Table 3), but only 25% of survivors require hospital admission (see Table 5). Most are not directly affected by blast, and are managed as for any other blunt trauma. Blast in an open space is an effective terror tactic if it is caught on film (such as in the Boston marathon bombing in 2013), but immediate mortality is low, and although most victims present to hospital, few need admission. Blast in a confined space (such as the London Underground bombings in 2005 or the Madrid train bombing in 2004) has a lower mortality than that involving structural collapse, but there is a comparatively high chance survivors will be affected by primary blast. While 39% require hospital admission, only 13% require ICU care and 18% require surgery (Kosashvili et al. 2009) The number of patients arriving near-simultaneously is the biggest problem: structural collapse can result in hundreds to thousands (median 359) presenting, while bombings in confined spaces result in a median of 53 presentations and open-air bombings, 76 (Arnold et al. 2004). Effective triage is essential, especially as the least affected patients usually arrive at hospital first (Hogan et al. 1999). A key consideration is to defer non-urgent imaging and manage minor injuries as outpatients. In large cities where terrorist events are most likely, effective prehospital casualty regulation should mean that surgical and critical care capacity is not overwhelmed.
Blast due to criminal acts or accidents is typically not a mass casualty event, therefore presenting more of a problem to clinicians than health planners and managers. A much higher proportion (59%) require surgery and ICU admission (Kulla et al. 2015).
Individual Patient Care
Tympanic membrane rupture requires antibiotic drops (e.g. ciprofloxacin and dexamethasone 4 drops tds [3 times a day]) for 7 days, but only uncommonly (10-20%) requires surgical repair (Chait et al. 1989). Hearing loss is usually not permanent (30% in one series) (Chait et al. 1989). The capillary disruption and diffuse alveolar haemorrhage of blast lung are pathologically different to other forms of ARDS, but have no specific treatment. Therapy is entirely supportive, involving protective lung ventilation and all other standard measures. Theoretically, high peak airway pressures should be avoided due to the risk of air embolus. Bowel rupture is treated in the same manner as any other form of ischaemic bowel necrosis. The main therapeutic priority in blast mild traumatic brain injury (mTBI) is to reduce the risk of re-exposure, as further insults appear multiplicative rather than additive. Various treatments for the headache, insomnia and mood changes that characterise this syndrome have been attempted, but none is yet supported by large controlled trial evidence. Penetrating trauma due to secondary blast is usually low-energy transfer and so does not require wide excision of wound tracts. Foreign bodies are often multiple, and should only be removed if lodged in joints or the subarachnoid space (to prevent lead toxicity), if they become the source of systemic infection, if they lie next to an internal organ that presents a risk of subsequent erosion, or if they cause persistent pain. Superficial blast fragmentation wounds only require sharp debridement if they are >1-2cm, present >24 hours after wounding, or are associated with fractures or vascular injury (Bowyer 1997). Otherwise, a simple chlorhexidine scrub is sufficient. All potentially contaminated wounds are left open until it is clear that no further debridement is required. IV antibiotic prophylaxis should start as soon as possible, ideally in <3hours. Various recommendations exist, but cefazolin 2g IV q6-8hr (+metronidazole 500mg bd for oesophageal, abdominal or central nervous system (CNS) wounds) is accepted by U.S. and allied military hospitals.
Special Considerations
Patients affected by both blast and burn injury should have particularly careful fluid resuscitation. The U.S. military now advocates the ‘rule of tens’ (10ml/% burn/hr), which is generally a mid-point between the Parkland and modified Brooke formulae (i.e. between 2 and 4 ml/ kg/% in the first 24hr). However, this should be titrated to both respiratory function and circulatory adequacy. Traumatic amputation in survivors of terrorist blasts features in popular media reports, perhaps due to its perceived frequency in recent combat. However, of >55,000 US casualties in Iraq and Afghanistan, only 1,645 had major limb amputations (Fischer 2015); civilian bombings only rarely result in traumatic limb amputation. Heterotopic ossification was first described in military casualties 1000 years ago, and is common in substantial trauma caused by blast — for example in 80% of a small sample of London bombing casualties (Edwards et al. 2015). Management involves excision followed by radiotherapy and nonsteroidal anti-inflammatory drugs (NSAIDs).
Conclusion
Most survivors of blast injury do not have clinically significant primary (blast wave) trauma. Civilian terrorist bombing survivors mainly present with penetrating low-energy transfer blast fragmentation wounds, or crush injury due to structural collapse. The main things that distinguish these civilian victims from non-blast trauma patients are the numbers of patients presenting (necessitating triage) and the number of body parts involved in each patient. In the low explosive blasts that typify accidental or homicidal civilian blast wounds, the commonest injuries are burn and low energy penetrating trauma — the management of which follows conventional principles. Treating such patients effectively is well within the scope of civilian trauma hospitals. The principles outlined here have been summarised conveniently by the
U.S. Centers for Disease Control in a mobile application (2014).
See Also:
Mobile Critical Care
Arnold JL (2004) Mass casualty terrorist bombings: a
comparison of outcomes by bombing type. Ann Emerg Med, 43(2): 263-73.
Bochicchio GV, Lumpkins K, O'Connor J et al. (2008) Blast
injury in a civilian trauma setting is associated with a delay in diagnosis of
traumatic brain injury. Am Surg, 74(3): 267-70.
Bowyer GW (1997) Management of small fragment wounds in
modern warfare: a return to Hunterian principles? Ann R Coll Surg Engl, 79(3):
175-82.
Centers for Disease Control and Prevention (2003) Explosions
and blast injuries: a primer for clinicians. [Accessed: 24 October 2015]
Available from cdc.gov/masstrauma/ preparedness/primer.pdf
Centers for Disease Control and Prevention (2014) CDC Blast
Injury Mobile Application [Accessed: 31 October 2015] Available from
emergency.cdc.gov/masscasualties/ blastinjury-mobile-app.asp
Chait RH, Casler J, Zajtchuk JT (1989) Blast injury of the
ear: historical perspective. Ann Otol Rhinol Laryngol Suppl, 140: 9-12.
Edwards DS, Clasper JC, Patel HD (2015) Heterotopic
ossification in victims of the London 7/7 bombings. J R Army Med Corps, pii:
jramc-2014-000370. doi: 10.1136/jramc2014-000370. [Epub ahead of print].
Fischer H (2014) A guide to US military casualty statistics.
Washington: Congressional Research Service.
Gibson PW (1994) Blast overpressure and survivability
calculations for various sizes of explosive charges. Natick, MA: United States
Army Natick Research, Development and Engineering Center.
Harrison CD, Bebarta VS, Grant GA (2009) Tympanic membrane
perforation after combat blast exposure in Iraq: a poor biomarker of primary
blast injury. J Trauma, 67(1): 210-1.
Hogan DE, Waeckerle JF, Dire DJ et al. (1999) Emergency department impact of
the Oklahoma City terrorist bombing. Ann Emerg Med, 34(2): 160-7.
Kapur GB, Hutson HR, Davis MA et al. (2005) The United States twenty-year
experience with bombing incidents: implications for terrorism preparedness and
medical response. J Trauma, 59(6): 1436-44.
Kosashvili Y, Loebenberg MI, Lin G et al.(2009) Medical
consequences of suicide bombing mass casualty incidents: the impact of
explosion setting on injury patterns. Injury, 40(7): 698-702.
Kulla M, Maier J, Bieler D et al. (2015) [Civilian blast
injuries: an underestimated problem?:
Results of a retrospective analysis of the TraumaRegister DGU®].
Unfallchirurg, 2015 Aug 19. [Epub ahead of print].
Savitsky E, Eastridge B, Don Kotz et al. (2012) Combat
casualty care: lessons learned from OEF
and OIF. Fort Detrick, MD: Office of the Surgeon General, United States Army.
[Accessed: 24 October 2015] Available from
archive.org/details/CombatCasualtyCare