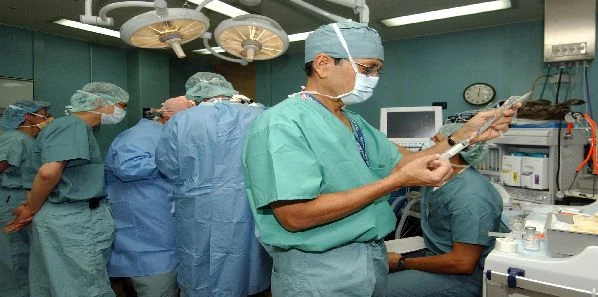
Anaesthesiologists play a vital role in perioperative care. In recent decades, the risks associated with anaesthetic care have been dramatically reduced. However, anaesthesia takes centre stage among acute healthcare services, and from a patient's perspective, anaesthesia-specific risks cannot be meaningfully isolated from perioperative and peri-interventional risks.
A new article reviews recent research results outlining the current trends of perioperative patient harm and summarises the evidence in favour of patient safety practices. Patient safety is defined as ‘the avoidance, prevention and amelioration of adverse outcomes or injuries stemming from the process of healthcare’, rather than from the patient's underlying medical condition.
Data on Perioperative Patient Harm
According to the seminal report ‘To Err is Human’ by the US-based Institute of Medicine in 2000, adverse events occur in 2.9 to 3.7 percent of hospital admissions, with 6.6 to 13.6 percent of adverse events leading to death. The report estimated 44,000 to 98,000 deaths per year due to medical errors in US hospitals, with 50 percent of these adverse events considered to be preventable.
A decade later, however, and using more sensitive research methods such as the ‘Global Trigger Tool' (GTT), adverse events were estimated to occur 10 times more often, and in 30 percent of hospital admissions. Even worse, more than 400, 000 deaths per year were estimated to be due to preventable adverse events, according to a review of studies from 2008 to 2011.
Analyses of large national US databases identified increasing trends of major in-hospital complications between 1998 and 2008. Further, adverse events were also found in 38.1 percent of hospital discharges from 2007 to 2011. Adverse events related to surgery represented the largest category (40.5 percent).
Recently, a Swedish study using the GTT confirmed these US findings. Adverse events, preventable in 71 percent of cases, were identified in 20.5 percent of discharges, and no decline was noted over four years. Hospital-acquired infections, almost always preventable, represented 47 percent of adverse events in surgical patients. In addition, a systematic review found that mostly preventable surgical and anaesthetic adverse events to contribute to 19.3–52.2 percent of unplanned ICU transfers.
Anaesthesia-Specific Mortality
Anaesthesia-specific mortality has been substantially reduced over the last decades and is estimated to be overall about 1:100,000 cases. According to the Fourth National Audit Project (NAP4) in the UK, 5.4 deaths per million general anaesthetics were estimated to result from airway complications. Because of underreporting, the true mortality rate may have been four times higher in this population. Regardless, the true airway-related mortality according to NAP4 (about 20 deaths per million general anaesthetics) would be double the traditional all-cause anaesthesia-specific mortality of 1:100,000.
This audit reveals important aspects of patient safety. Despite challenging situations, no ‘plan B’ had been made in most cases. Moreover, proven technologies (e.g., fibreoptic bronchoscopy, capnography) had been disregarded, and established protocols for airway management had not been followed.
Perioperative Safety: A Shared Responsibility of Surgery and Anaesthesiology
Both surgery and anaesthesia contribute to patient harm in the perioperative period. Accordingly, perioperative harm should largely be considered a shared responsibility of surgery and anaesthesia. A review supported by the US Department of Health and Human Services’ Agency for Healthcare Research and Quality examined 41 patient safety practices. Ten practices were ‘strongly encouraged’, and additional 12 practices were ‘encouraged’ for adoption. The study presented a selection of practices relevant for increasing safety issues in perioperative care.
Postoperative infections remain an area of concern in surgical patients, despite evidence for decreasing mortality from infectious complications. Increasing trends were noted for postoperative pneumonia, catheter-associated urinary tract infections, ventilator-associated pneumonia, and bloodstream infections and sepsis.
Analysis of a large perioperative database suggested an association between intraoperative hypotension below 55 mmHg mean arterial pressure, even for short periods of between one to five minutes, and the occurrence of postoperative acute kidney injury and myocardial injury. Hypotension has also been associated with the perioperative occurrence of stroke.
Although no absolute and generalisable lower limit of systemic blood pressure to avoid organ injuries has been defined yet, clinical working definitions are widely used and often represent institutional standards.
Improving Safety Culture and Communication
Safety culture, as measured by survey-based ratings of surgeons, nurses, and operating room administrators, has been reported to be associated with rates of serious surgical complications. Interventions to improve safety culture may target leadership, teamwork, or behaviour changes, examples of which include interdisciplinary rounding, team training and encouraging error reporting.
Also, a number of systematic reviews have documented the efficacy of surgical checklists to improve surgical mortality and morbidity, teamwork and communication in the operating room, and compliance with safety measures. In terms of perioperative patient safety, surgical checklists are just one piece of many in a comprehensive safety strategy and should not be regarded as a substitute for other important patient safety activities with comparable evidence for effectiveness.
Conclusions
Anaesthesia has low specific risk, but has an important impact on perioperative risk and outcomes. Evidence-based recommendations are available for many patient safety practices. Important practical targets include the prevention of perioperative infections, airway and respiratory management, maintenance of safety standards despite production pressure, and others.
Future research should provide more high-quality evidence about the effectiveness of patient safety practices, deeper insights into common patterns of preventable events, and implementation of surgical checklists and other practices.
Image Credit: Wikipedia
A new article reviews recent research results outlining the current trends of perioperative patient harm and summarises the evidence in favour of patient safety practices. Patient safety is defined as ‘the avoidance, prevention and amelioration of adverse outcomes or injuries stemming from the process of healthcare’, rather than from the patient's underlying medical condition.
Data on Perioperative Patient Harm
According to the seminal report ‘To Err is Human’ by the US-based Institute of Medicine in 2000, adverse events occur in 2.9 to 3.7 percent of hospital admissions, with 6.6 to 13.6 percent of adverse events leading to death. The report estimated 44,000 to 98,000 deaths per year due to medical errors in US hospitals, with 50 percent of these adverse events considered to be preventable.
A decade later, however, and using more sensitive research methods such as the ‘Global Trigger Tool' (GTT), adverse events were estimated to occur 10 times more often, and in 30 percent of hospital admissions. Even worse, more than 400, 000 deaths per year were estimated to be due to preventable adverse events, according to a review of studies from 2008 to 2011.
Analyses of large national US databases identified increasing trends of major in-hospital complications between 1998 and 2008. Further, adverse events were also found in 38.1 percent of hospital discharges from 2007 to 2011. Adverse events related to surgery represented the largest category (40.5 percent).
Recently, a Swedish study using the GTT confirmed these US findings. Adverse events, preventable in 71 percent of cases, were identified in 20.5 percent of discharges, and no decline was noted over four years. Hospital-acquired infections, almost always preventable, represented 47 percent of adverse events in surgical patients. In addition, a systematic review found that mostly preventable surgical and anaesthetic adverse events to contribute to 19.3–52.2 percent of unplanned ICU transfers.
Anaesthesia-Specific Mortality
Anaesthesia-specific mortality has been substantially reduced over the last decades and is estimated to be overall about 1:100,000 cases. According to the Fourth National Audit Project (NAP4) in the UK, 5.4 deaths per million general anaesthetics were estimated to result from airway complications. Because of underreporting, the true mortality rate may have been four times higher in this population. Regardless, the true airway-related mortality according to NAP4 (about 20 deaths per million general anaesthetics) would be double the traditional all-cause anaesthesia-specific mortality of 1:100,000.
This audit reveals important aspects of patient safety. Despite challenging situations, no ‘plan B’ had been made in most cases. Moreover, proven technologies (e.g., fibreoptic bronchoscopy, capnography) had been disregarded, and established protocols for airway management had not been followed.
Perioperative Safety: A Shared Responsibility of Surgery and Anaesthesiology
Both surgery and anaesthesia contribute to patient harm in the perioperative period. Accordingly, perioperative harm should largely be considered a shared responsibility of surgery and anaesthesia. A review supported by the US Department of Health and Human Services’ Agency for Healthcare Research and Quality examined 41 patient safety practices. Ten practices were ‘strongly encouraged’, and additional 12 practices were ‘encouraged’ for adoption. The study presented a selection of practices relevant for increasing safety issues in perioperative care.
Postoperative infections remain an area of concern in surgical patients, despite evidence for decreasing mortality from infectious complications. Increasing trends were noted for postoperative pneumonia, catheter-associated urinary tract infections, ventilator-associated pneumonia, and bloodstream infections and sepsis.
- Evidence for effectiveness to reduce postoperative pneumonia has been found for a multidisciplinary, multiform pulmonary care programme and for neuraxial blocks when used instead of general anaesthesia or in combination.
- Effective strategies to reduce surgical site infections (SSIs) include timely administration of the correct prophylactic antibiotic, maintenance of normothermia, hand hygiene, and bundles to prevent venous access infections, checklists, and standardisation.
- Central line-associated bloodstream infections have been successfully reduced by a number of safety practices, approaches, and technologies.
Analysis of a large perioperative database suggested an association between intraoperative hypotension below 55 mmHg mean arterial pressure, even for short periods of between one to five minutes, and the occurrence of postoperative acute kidney injury and myocardial injury. Hypotension has also been associated with the perioperative occurrence of stroke.
Although no absolute and generalisable lower limit of systemic blood pressure to avoid organ injuries has been defined yet, clinical working definitions are widely used and often represent institutional standards.
Improving Safety Culture and Communication
Safety culture, as measured by survey-based ratings of surgeons, nurses, and operating room administrators, has been reported to be associated with rates of serious surgical complications. Interventions to improve safety culture may target leadership, teamwork, or behaviour changes, examples of which include interdisciplinary rounding, team training and encouraging error reporting.
Also, a number of systematic reviews have documented the efficacy of surgical checklists to improve surgical mortality and morbidity, teamwork and communication in the operating room, and compliance with safety measures. In terms of perioperative patient safety, surgical checklists are just one piece of many in a comprehensive safety strategy and should not be regarded as a substitute for other important patient safety activities with comparable evidence for effectiveness.
Conclusions
Anaesthesia has low specific risk, but has an important impact on perioperative risk and outcomes. Evidence-based recommendations are available for many patient safety practices. Important practical targets include the prevention of perioperative infections, airway and respiratory management, maintenance of safety standards despite production pressure, and others.
Future research should provide more high-quality evidence about the effectiveness of patient safety practices, deeper insights into common patterns of preventable events, and implementation of surgical checklists and other practices.
Image Credit: Wikipedia
References:
Wackera J, Staender S (2014) The role of the anaesthesiologist in
perioperative patient safety. Curr Opin Anaesthesiol. Dec 2014; 27(6):
649–656. PMCID: PMC4232292 doi: 10.1097/ACO.0000000000000124
Latest Articles
Communication, Surgery, anaesthesia, perioperative care, patient safety
Anaesthesiologists play a vital role in perioperative care. In recent decades, the risks associated with anaesthetic care have been dramatically reduced. H...