ICU Management & Practice, Volume 18 - Issue 1, 2018
Their inability to communicate effectively whilst he had a tracheostomy on the intensive care unit (ICU), had such a profound impact on Duncan Buckley and his wife, Lisa-Marie, that they developed a concept for a novel interactive communication device, called ‘ICU CHAT’. Together, they have been embedded within the multidisciplinary ICU research team at the Queen Elizabeth Hospital Birmingham (QEHB), supported by the Human Interface Technologies team from the University of Birmingham, and funded by the National Institute of Health Research Surgical Reconstruction and Microbiology Research Centre, to further develop their prototype for clinical trial.
You might also like: Over Half of ICU Patients on Ventilators Able to Communicate
Lisa-Marie Buckley: Wife of Duncan, University Hospitals Birmingham (UHB) ICU survivor.
Communication in the ICU
Patient communication in the ICU is a widely recognised challenge, causing frustration for patients, relatives and staff (ten Hoorn et al. 2016). Due to the presence of artificial airway devices, such as a tracheostomy, patients are often voiceless as airflow bypasses the vocal cords and inhibits speech. This is often combined with the profound weakness or injury associated with critical illness, therefore limiting other non-verbal forms of communication, such as writing or lip-reading (Muthuswamy et al. 2014). ‘Voicelessness’ is considered to have both short- and long-term consequences for the patient, including stress, anxiety and social isolation, which are predisposing traits of post-traumatic stress amongst ICU survivors (Wade et al. 2012). It is therefore necessary that methods of communication are developed in order to improve the patient experience in the ICU in addition to patient outcomes.
Augmented and alternative communications (AAC) devices in the ICU
AAC is a broad term for any method, technology or tool used to overcome barriers to communication. Although there are a range of AAC devices available on the market, none of those identified in the literature have been designed specifically for use in the ICU and therefore have limited transferability to this complex and challenging environment (ten Hoorn et al. 2016). Low technology AAC, such as alphabet boards, are often easily accessible and low cost. However, despite their convenience, low-tech AAC have variable success depending on the physical and cognitive ability of the patient recovering from critical illness and the time constraints and skill of staff (Patak et al. 2004). High technology AAC is a broad and advancing area, yet the available literature identifies practical and financial limitations to use in the ICU (ten Hoorn et al. 2016). The current literature does not explore factors relating to AAC requirements or usability specifically for alert and transiently voiceless tracheostomy patients in the ICU.

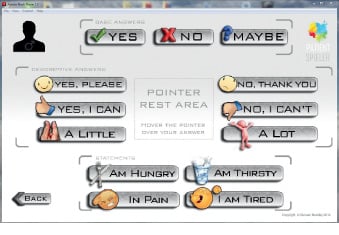
Patient-centred design process
The novel ‘ICU CHAT’ software design, developed by Duncan and Lisa-Marie, has been developed for use by ICU tracheostomy patients, with restricted upper limb function. The use of facial gestures enables the user to control an on-screen cursor with their head movement, selecting phrases with vocal output. This novel and exciting idea was immersed by the Human Interface Technologies team from the University of Birmingham, alongside the ICU multidisciplinary research team at QEHB. By combining usability assessment with multidiscipinary team qualitative appraisal, the appropriateness of the system components were developed to ensure safety, practicality and low cost for use in the ICU. Following a human-centred design process and rigorous bench testing, the ICU CHAT device was developed (BSI 2010; IEC 2007).
ICU CHAT feasibility study
The multidisciplinary ICU research team at QEHB developed a clinical trial protocol to evaluate the usability and user acceptance of ‘ICU CHAT’ by patients, staff and relatives at QEHB’s ICU. The mixed methods trial design aims to collect quantitative data on usage and performance alongside qualitative appraisal to explore user experiences. The trial Feasibility of the use of a novel interactive communication device, ICU-CHAT, for patients with tracheostomy on the ICU has secured Health Research Authority permissions and is open to recruitment at QEHB. This early translational research demonstrates the ability of clinical and academic teams to support potential patient innovators, whose reflections on experiences during their ICU stay enable technology development to be truly patient-centered.
References:
IEC (2007) IEC 62366: 2007 Medical devices–Application of usability engineering to medical devices. Geneva. International Electrotechnical Commission.
Muthuswamy MB, Thomas BN, Williams D et al. (2014) Utility of optical facial feature and arm movement tracking systems to enable text communication in critically ill patients who cannot otherwise communicate. Burns, 40 (6): 1189-93.
Patak, L, Gawlinski A, Fung I et al. (2004) Patients’ reports of health care practitioner interventions that are related to communication during mechanical ventilation. Heart Lung, 33 (5): 308-20.
Hoorn S, Elbers PW, Girbes AR et al. (2016) Communicating with conscious and mechanically ventilated critically ill patients: a systematic review. Crit Care, 20 (333): 1-14.
Wade DM, Howell DC, Weinman JA et al. (2012) Investigating risk factors for psychological morbidity three months after intensive care; a prospective cohort study. Crit Care, 16 (5):192.







