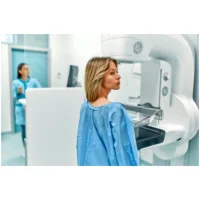
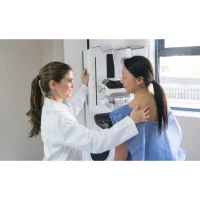
A large German study found that most women who participate in breast cancer screening prefer a reliable cancer diagnosis over avoiding false-positive findings. Dr Toni Vomweg, a radiologist at Radiologisches Institut in Koblenz, Germany, presented the research findings at RSNA 2021.
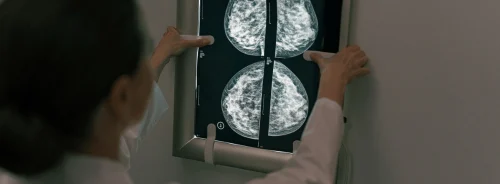
Mammography is the current standard of care for breast cancer screening, with MRI and ultrasound representing alternate screening methods. MRI carries a similar positive predictive value (PPV, the proportion of positive results that are true positives) to mammography, whereas ultrasound’s PPV is much lower. Due to its greater sensitivity, breast MRI produces 2-3 times higher true-positive diagnoses than mammography. This means MRI also gives 2-3 more false-positive diagnoses.
The medical community belabours the benefits and harms caused by over- and underdiagnosis regarding breast cancer screening. Thus, overdiagnosis, a criticism often applied to mammographic screening, applies more so to MRI because false-positive diagnoses cause damage. Conversely, underdiagnosis of breast cancers due to false-negative results carries an entirely different set of severe consequences.
Despite this ongoing debate, the preference of the women undergoing screening for false-positive vs false negatives diagnoses and the related screening methods is unclear. Thus, Dr Toni Vomweg and colleagues investigated women’s preferences at three German Mammography Screening Program sites.
Women, aged 50 to 69, received a letter explaining mammographic screening and its effectiveness, adverse effects, and the concept of overdiagnosis. Participants received a plain-language questionnaire explaining false-positive and false-negative diagnoses associated with screening.The survey asked whether the women preferred screening that avoids false-negative diagnoses, even if it increased the rate of false alarms (false positives). Or if they preferred the opposite, a method that avoids false-positives, but may fail to find cancer (false negative). Of 906 women that completed the survey, 93.1% (851) chose more sensitive breast cancer detection over avoiding false-positive findings. Only 6.1% (55) preferred preventing the possibility of more false alarms. These results did not depend on age or education level. However, the study can only be interpreted with the lens that only women who already chose to undergo screening were surveyed.
Dr Vomweg adds: ‘Currently, mammographic screening is criticized mainly because overdiagnosis, the effects of overtreatment, and the harm caused by false-positive diagnosis.’ He concludes: ‘If the decision were left up to the women themselves, 94% would prefer a more sensitive screening method, even aware it is not only more reliable at finding breast cancer, but also correspondingly more likely to cause a false alarm.'
Click here for the latest Women's Health news
Source:RSNA Daily Bulletin, RSNA


.jpg)