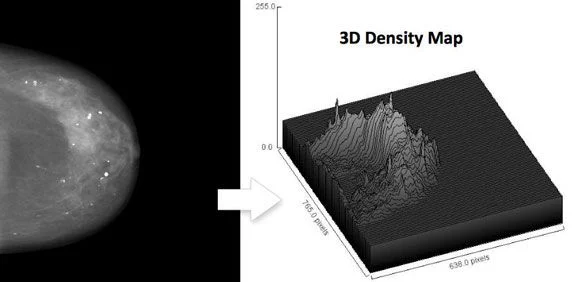
Seven Abstracts Accepted for Presentation at ECR Demonstrate Benefit of Volumetric Breast Care Imaging and Analytics Data
The ability of volumetric breast imaging data to provide actionable intelligence to guide screening of women with dense breasts with 2D and 3D mammography are among the key abstracts accepted for presentation at the European Congress of Radiology (ECR) meeting, March 6-10, 2014. According to Volpara Solutions, seven abstracts highlight the use of quantitative breast imaging software tools to provide Enterprise-wide breast care imaging and informatics, including volumetric density, patient-specific dose, and applied pressure.
The company will showcase the role of its suite of volumetric software tools in a number of large clinical trials, national breast cancer screening programs and hospitals across Europe. (ECR2014 - First level gallery, booth 619).
In the scientific exhibit titled, “Comparing personalized mean glandular dose estimates between x-ray systems over time in mammography” (C-0360), Dr. Ralph Highnam, CEO of Volpara Solutions and a co-author, demonstrates that patient-specific estimates of Mean Glandular Dose (MGD) could be used to help standardise dose monitoring for patients undergoing routine screening on different x-ray systems. The results indicate that the patient-specific estimates of MGD, which incorporate the individual glandularities of the women and use a standard dose algorithm, differ from, but correlate well with the reported doses from GE and Hologic systems. Compared to patient-specific estimates, the mammography systems tended to underestimate MGD.
In the study, “Volumetric breast density estimation on conventional mammography versus digital breast tomosynthesis” (C-0363) VolparaDensity was used to compare the assessment of volumetric breast density of conventional 2D mammograms to assessment of digital breast tomosynthesis (DBT) volumetric density. Results show that there was no significant difference between volumetric breast density, breast volume, and fibroglandular volume estimates from conventional mammograms or the DBT projections. The Volpara generated BI-RADS density scores matched for 19 out of 20 cases, indicating that there was very good agreement between density assessed from the DBT projections and the conventional mammograms. The results suggest that automated volumetric breast density methods are a promising alternative to visually assessed breast density assessments, and produce reliable and objective breast density estimations from both raw conventional mammograms and raw DBT projections.
“While only a few studies have investigated breast density results derived specifically from tomosynthesis, studies have shown significant differences in the density results from 2D and 3D mammography. The current study, using automated volumetric breast density estimations showed very good correlations between the 2D and 3D mammograms, as you might expect given the volumetric nature of the measurement. These results have additional implications for those wanting to monitor longitudinal changes in breast density or for studies looking at breast density as a breast cancer risk factor. Additionally, for sites wanting to implement the C-View module, to replace conventional mammography, automated volumetric methods like VolparaDensity can ensure consistency in breast density measures,” said Dr. Highnam.
Breast cancer screening programs strive to achieve an optimal balance between sensitivity and recall rates. The interpretation of screening mammograms is often challenging and highly variable, but the addition of multiple readers can improve cancer detection rates. While numerous variations in screening protocols have been studied, they have largely sought to apply one protocol across entire populations. In the study, “Effect of independent double and multiple reading of screening mammograms by breast density,” (C-0358) Professor Nico Karssemeijer et al of Nijmegen investigated the effect of increasing the number of independent readers on mammography sensitivity, for dense versus non-dense cases.
“In the United States, breast screening typically comprises annual mammography and single reading with CAD, whereas European guidelines recommend biennial mammography with independent double reading. Double interpretation of mammograms is a proven, effective strategy to improve cancer detection rates,” noted Professor Karssemeijer. “The benefit of additional readers on sensitivity was more pronounced in dense cases, suggesting that tailored screening based on breast density has the potential to improve breast cancer detection rates for this population of women. The allocation of multiple readers to mammograms that may be difficult to interpret offers a relatively simple and effective approach for improving screening performance on women with dense breasts, especially with automated density assessment systems and density-based workflow tools.”
In the study, “Mammographic Density Estimation by Volpara software: Comparison with Radiologists’ visual assessment and relationship with BI-RADS category” (C-1957) Professor L. Han Na of Seoul Korea, compares the automated volumetric breast density measurement with BI-RADS breast density assessed by radiologists’ visual estimates and analyze the clinico-radiologic factors that affect the disagreement. Results demonstrate that the automated volumetric breast density measurement shows good agreement with radiologists’ visual assessment of BI-RADS density category, with differences occurring more often when there were bilateral differences in density.
Cleared by the FDA, HealthCanada, the TGA and CE-marked, VolparaDensity is used by radiologists to objectively assess density from both digital mammography and tomosynthesis images and help evaluate who might benefit from additional screening. Highly correlated to breast MR assessments, VolparaDensity is a reliable tool which automatically generates an objective, automatic measurement of volumetric breast density and a FDA cleared BI-RADS breast density category. To date, more than 2 million women have had their volumetric breast density analysed using VolparaDensity.
Source: Volpara Solutions
27 February 2014
Latest Articles
Mammography, Radiology, IT solutions, Breast density, BI-RADS, digital mammography, breast cancer screening, Volpara Solutions
Seven Abstracts Accepted for Presentation at ECR Demonstrate Benefit of Volumetric Breast Care Imaging and Analytics Data The ability of volumetric brea...