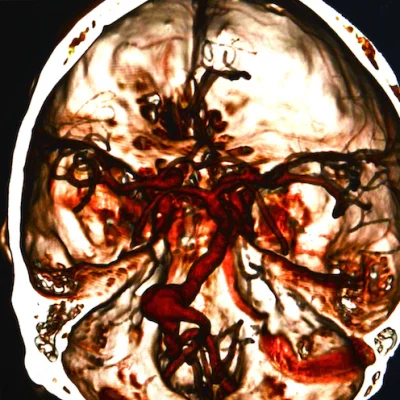
In a new study, a team of researchers from the Massachusetts General Hospital (MGH) Department of Radiology created an artificial intelligence (AI) powered system that successfully detects acute intracranial haemorrhage (ICH) and also categorises five ICH subtypes from unenhanced head computed-tomography scans (CT).
In the report published online in Nature Biomedical Engineering the investigators explain how the system using machine-learning could provide not only a quick diagnosis and classification of brain haemorrhages but most importantly substantiate its findings providing a basis of its decisions eventhough it drew information from a small pool of image datasets.
You may also like: Teaching radiologists machine learning - AI
The results of the study illustrate how this system can provide hospital emergency departments with a crucial solution to help detect and provide fast and accurate treatment to patients that present with symptoms of potentially deadly stroke.
The terms 'machine-learning' and 'deep-learning' are rapidly becoming part of the radiology vernacular. Advances in expanding the range of computing and analysing capabilities and the recent releases of large datasets further fuel artificial intelligence algorithms to 'learn' how to recognise patterns in vast amounts of data and eventually be able to perform tasks independant of a human operator. While the improvements in image recognition using deep-learning and machine-learning algorithms may potentially be used to automate medical diagnoses that can inform clinical decision-making, important problems in the process make this scenario far from feasible in the near future.
The most prevalent issues to the prevention of clinical implementation of similar high-performance deep learning systems are the requirement of vast and high-quality training datasets from which the algorithms can 'learn'; and the 'black box' issue which is the inability of a system to provide a basis of how they generate the results from the inputed data. The U.S. Food and Drug Administration requires any decision support system to provide information allowing users to review the reasons behind its findings.
The team from MGH used a relatively small dataset of only 904 CT scan cases for training their system- each of separate images that five MGH neuroradiologists had evaluated as presenting, or not presenting, one of five subtypes of haemorrhaging based on where the findings were located in the brain. The investigators reported that their system performed similar to the expert radiologists in two independent test datasets containing 200 cases (sensitivity of 98% and specificity of 95%) and 196 cases (sensitivity of 92% and specificity of 95%).
The team led by Dr. Synho Do, director of the MGH Radiology Laboratory of Medical Imaging and Computation and an assistant professor of Radiology at Harvard Medical School built in the system an attention map and a prediction basis retrieved from training data to enhance explainability, as well as an iterative process of steps that mimics the workflow of how radiologists analyse images. The steps include to adjust contrast and brightness enhancing differences not clearly visible and to scroll through adjacent CT scan segments to determine if a finding is a real issue or an insignificant artefact.
"It is somewhat paradoxical to use the words 'small data' or 'explainable' to describe a study that used deep learning," said in a statement Hyunkwang Lee, Harvard School of Engineering and Applied Sciences, one of the two lead authors of the study. "However, in medicine, it is especially hard to collect high-quality big data. It is critical to have multiple experts label a dataset to ensure consistency of data. This process is very expensive and time-consuming."
Dr. Sehyo Yune, co-lead author of the study from MGH Radiology said, "Some critics suggest that machine learning algorithms cannot be used in clinical practice, because the algorithms do not provide justification for their decisions. We realized that it is imperative to overcome these two challenges to facilitate the use in health care of machine learning, which has an immense potential to improve the quality of and access to care."
The researchers addressed the 'black box' problem by having their system review and save the images from the training dataset that represented clear classic features of the five separate haemorrhage subtypes. Using this roadmap the system can present a group of images similar to the CT scans being analysed so as to document the basis of its results.
"Rapid recognition of intracranial haemorrhage, leading to prompt appropriate treatment of patients with acute stroke symptoms, can prevent or mitigate major disability or death," said in a statement co-author Dr. Michael Lev,MGH Radiology. "Many facilities do not have access to specially trained neuroradiologists- especially at night or over weekends- which can require non-expert providers to determine whether or not a haemorrhage is the cause of a patient's symptoms. The availability of a reliable, 'virtual second opinion' - trained by neuroradiologists - could make those providers more efficient and confident and help ensure that patients get the right treatment."
Dr. Shahein Tajmir, co-author, MGH Radiology said, "In addition to providing that much needed virtual second opinion, this system also could be deployed directly onto scanners, alerting the care team to the presence of a haemorrhage and triggering appropriate further testing before the patient is even off the scanner. The next step will be to deploy the system into clinical areas and further validate its performance with many more cases. We are currently building a platform to allow for the widespread application of such tools throughout the department. Once we have this running in the clinical setting, we can evaluate its impact on turnaround time, clinical accuracy and the time to diagnosis."
The research team reports that their approach to algorithm development can facilitate the development of deep-learning systems for a variety of clinical applications and accelerate their adoption into clinical practice.
Image credit: iStock
References:
Latest Articles
Radiology, CT scans, Artificial Intelligence, AI, deep-learning algorithm, ICH, datasets, acute intracranial haemorrhage, machine-learning, clinical decision-making, neuroradiologists
In a new study, a team of researchers from the Massachusetts General Hospital (MGH) Department of Radiology created an artificial intelligence (AI) powered system that successfully detects acute intracranial haemorrhage (ICH) and also categorises five ICH