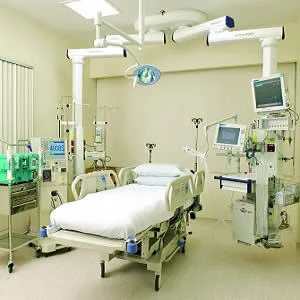
Intensive Care Units are an integral part of the healthcare system. Approximately 164,000 patients are admitted to ICUs in England, Wales and Northern Island each year. Similarly, there are around 4 million ICU admissions per year in the U.S. While ICUs' are a regular feature in all high, middle and low income countries, disparities still exist in terms of capacity and quality of care. For example Boston, U.S. has 45 times as many ICU beds per population as Kumasi in Ghana.
The fact is that the definition of an ICU bed varies around the world and even within a single healthcare system. That is why In 2014, the World Federation of Societies of Intensive and Critical Care Medicine (WFSICCM) convened a task force with the specific objective of answering this question: "What is an ICU" in a manner that was internationally meaningful and to stratify ICUs on the basis of the intensity of care they provide.
For this purpose, they analysed peer-reviewed and grey literature and after discussion among various task force members, presented this definition of an ICU:
"An ICU is an organised system for the provision of care to critically ill patients that provides intensive and specialised medical and nursing care, an enhanced capacity for monitoring, and multiple modalities of
physiologic organ support to sustain life during a period of life-threatening organ system insufficiency. While an ICU is based in a defined geographic area of a hospital, its activities often extend beyond the walls of the physical space to include the emergency department, hospital ward, and follow-up clinic."
ICUs were classified on the basis of the following parameters: availability of skilled medical and nursing personnel, respiratory therapists, physiotherapists, pharmacists, nutritionists etc; capacity to monitor acutely ill patients; resources to support failing organ function; design and structure of physical space; integration with ICU outreach services; formal educational and professional development services; a dedicated house staff and centre for training expert personnel; focus on research and quality improvement; referral service for the hospital, community and the country; and the ability to scale up services when needed.
See also: The ICU Specialist: WFSICCM Task Force Report
The report also defines levels of ICU:
- Primary (Level One) ICU can provide oxygen, noninvasive monitoring, and more intensive nursing care than on a ward.
- Secondary (Level Two) ICU can provide invasive monitoring and basic life support for a short period of time.
- Tertiary (Level Three) ICU can provide a a full spectrum of monitoring and life support technologies and can also serve as a regional resource for the critically ill. In addition, a Level Three ICU can play an active role in further advancing intensive care through research and education.
The WFSICCM report thus concludes that an ICU is not just a geographic locale but is a dedicated area in a hospital that provides care to the sickest patients and is managed by a specialised multidisciplinary professional team. The proposed stratification in this report is a guideline for discussion and may be used as a template to better utilise healthcare resources and to enhance care of critically ill patients worldwide.
Source: WFSICCM
Image Credit: Flickr
Latest Articles
ICU, WFSICCM, intensive care, life support, critically ill
In 2014, the World Federation of Socieites of Intensive and Critical Care Medicine (WFSICCM) convened a task force with the specific objective of answering this question: "What is an ICU" in a manner that was internationally meaningful and to stratify ICU