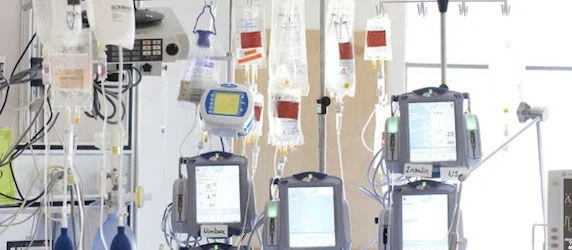
Findings of a study published in the March 19 issue of JAMA show that following their hospital discharge, critically ill patients receiving mechanical ventilation had a higher prevalence of prior psychiatric diagnoses and an increased risk of a new psychiatric diagnosis and medication use.
As medical care advancements lead to a larger number of critical illness survivors, these patients are exposed to stress that may impact subsequent mental health. Contributing factors include respiratory distress, pain, and delirium.
According to background information in the article, the extent of psychiatric illness prior to critical illness, as well as the magnitude of increased risk of psychiatric illness following critical illness, is unclear.
Together with her team of colleagues, Hannah Wunsch, MD, MSc, of New York’s Columbia University, led the assessment of psychiatric diagnoses and medication prescriptions before and after critical illness.
Including critically ill patients in Denmark from 2006-2008 with follow-up through 2009, the study matched comparison groups of hospitalised patients and the general population. Critical illness was defined as intensive care unit (ICU) admission with mechanical ventilation.
Of the over 24,000 critically ill patients included in the study, 6.2% had 1 or more psychiatric diagnoses in the 5 years prior to critical illness, compared to the 5.4% of hospitalised patients and 2.4% of the general population. The proportion of 5-year preadmission prescriptions for psychoactive drugs (defined as those affecting mental functioning such as mood, behavior, or thinking processes) were similar to those for hospitalised patients (48.7 percent vs 48.8 percent) but higher than those for the general population (33.2 percent).
The absolute risk of new psychiatric diagnoses was low among the roughly 10,000 critical illness survivors who had no psychiatric history, but it was higher than that for hospitalised patients (0.5 percent vs 0.2 percent over the first 3 months) and the general population group (0.02 percent).
New psychoactive medication prescriptions were given to a higher proportion of patients in the first 3 months (12.7 percent vs 5.0 percent for the hospital group) and 0.7 percent for the general population, however this difference had largely resolved by the end of the first year of follow-up.
In their commentary the authors described their study as providing vital data both on the burden of psychiatric illness among critically ill patients who require mechanical ventilation, as well as on the risks of psychiatric diagnoses and treatment with psychoactive medications in the year following the patients’ ICU discharge.
They suggested that discharge planning for these patients necessitated broader discussion of follow-up psychiatric assessment, as well as the caregivers and other family members’ education with regards to the patient’s potential psychiatric needs.
In concluding their report, the team stated that despite the absolute risks being low, considering the strong association between psychiatric diagnoses (such as depression) and poor outcomes after acute medical events, such as myocardial infarction and surgery, their data suggested the prompt evaluation and management of psychiatric symptoms could be an important focus for future interventions in this high-risk group.
19 March 2014
Latest Articles
ICU, Psychiatry, mechanical ventilation, Critical Care, mental disorders, discharge readiness, delirium
Findings of a study published in the March 19 issue of JAMA show that following their hospital discharge, critically ill patients receiving mechanical vent...