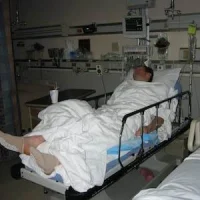
A conservative protocol for oxygen therapy for intensive care patients led to lower ICU mortality, in a randomised controlled trial that was terminated early after difficulties in enrolment.
The Normal Oxygenation Versus Hyperoxia in the Intensive Care Unit (ICU) (OXYGEN-ICU) trial was conducted in one centre in Italy between March 2010 and October 201. Patients admitted to the medical-surgical ICU of Modena University Hospital who were expected to stay 72 hours or longer were included.
Due to enrolment difficulties, the study stopped after 480 patients were enrolled, rather than the planned 660.
434 patients received either:
1) oxygen therapy to maintain PaO2 between 70 and 100mmHg or arterial oxyhemoglobin saturation (SpO2) between 94% and 98% (conservative group, n=216)
2) standard ICU practice, to allow PaO2 values up to 150mmHg or SpO2 values between 97% and 100% (conventional control group, n=216).
Results
Conservative group:Mortality: 11.6%
Daily time-weighted PaO2 averages: median PaO2, 102mmHg [IQR,
88-116])
Shock: 3.7%
Liver failure: 1.9%
Bacteraemia: 5.1%
Conventional group:
Mortality: 20.2%
Daily time-weighted PaO2 averages: median PaO2, 87mmHg [IQR, 79-97]
Shock: 10.6%
Liver failure: 6.4%
Bacteraemia: 10.1%
The researchers acknowledge that the early termination of the trial may have exaggerated the effect size. Although patients were randomised, patients in the conventionally treated group were more severely ill at baseline. They recommended a larger multicentre trial to evaluate the potential benefit of conservative treatment versus conventional treatment.
In an accompanying editorial Niall Ferguson, Toronto General Hospital, Canada, writes that until further trials are done, “there is little downside in the careful titration and monitoring of supplemental oxygen in the ICU to achieve physiologically normal levels of PaO2 while avoiding potentially dangerous hyperoxia.”
Source: JAMA
Image credit: Wikimapia
References:
Girardis M, Busain S, Damianai E, Donati A, Rinaldi L, Marudi A, Morelli
A, Antonelli M, Singer M (2016) Effect of conservative vs conventional oxygen therapy on mortality among patients in an intensive care unit.
JAMA, doi:10.1001/jama.2016.11993, published online October 5, 2016.
Ferguson ND (2016) Oxygen in the ICU: too much of a good thing? JAMA, doi:10.1001/jama.2016.13800, published online October 5, 2016.
Ferguson ND (2016) Oxygen in the ICU: too much of a good thing? JAMA, doi:10.1001/jama.2016.13800, published online October 5, 2016.
Latest Articles
oxygen therapy, mortality
A conservative protocol for oxygen therapy for intensive care patients led to lower ICU mortality, in a randomised controlled trial that was terminated early after difficulties in enrolment.