A simple and easy to use nomogram can predict the likelihood of
readmission to surgical intensive care using just 7 common variables
already collected for critical care patients, according to research
presented at the 2016 Clinical Congress of the American College of
Surgeons.
Luke A. Martin, MD, a general surgery research resident and the study’s presenting author, in an email to ICU Management & Practice, said: “The novel aspect to our nomogram compared to prior tools/studies is that it is so simple and easy to use. Prior tools require collection of tens of variables on each patient and oftentimes some complex calculations—they just aren’t that practical for clinical practice. Our nomogram uses 7 variables that are available in virtually all ICU patients and then rapidly and easily calculates a numeric risk for ICU readmission.”
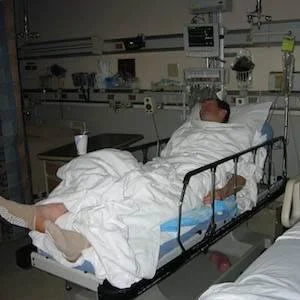
Martin and his fellow researchers from the University of Utah School of Medicine, Salt Lake City, developed the risk prediction tool or nomogram to determine a patient's risk level for returning to the surgical intensive care unit (SICU) within 72 hours after discharge. Martin outlined the benefits of this approach - namely avoiding patient care transitions between general wards and the SICU, when the risk of adverse events and errors is high. Readmissions rate are already used to measure quality, and the Centers for Medicare and Medicaid Services reduces reimbursements to hospitals that have excess 30-day readmission rates.
See Also: Is ICU Readmission Associated with Higher Severity of Illness Scores?
In their study, Dr. Martin and his colleagues evaluated the medical records for all SICU admissions at the University of Utah Hospital between April 2010 and July 2015. From among 3,109 SICU admissions, the investigators found that 141 patients were readmitted to the SICU within 72 hours of discharge. The patients had been admitted for trauma, general surgical, vascular and transplant procedures, but cardiac patients were not included, as the hospital has a separate cardiac ICU. From 179 possible demographic, clinical and laboratory measures that could contribute to risk of readmission, the researchers used statistical methods to reduce these to just seven:
A total of 40 points (the minimum that an ill SICU patient would likely have, Dr. Martin explained) to 79 points represented a 1 to 5 percent chance, or low risk, for SICU readmission, according to the study abstract. A 6 to 20 percent chance--medium risk--of readmission was 80 to 114 points, and a 21 to 50 percent chance--or high risk--was 115 to 150 points total. The nomogram was validated using data from 577 additional SICU patients.
"The risk prediction model has a moderately good ability to predict readmission to the surgical ICU and takes only about a minute to calculate for each patient," Martin said. "This nomogram allows for a quick and easy assessment of the surgical ICU patient's readiness to leave the SICU."
Martin said that the researchers are studying the accuracy of the nomogram by specific category of surgical procedure, starting with vascular surgical procedures. They are also currently in the process of implementing a protocol to use this tool in all of their ICU patients, and they will study the impact it has on our readmission rate. They plan to validate the tool at other institutions in the future.
Dr. Martin's co-investigators from the University of Utah are Ragheed Al-Dulaimi, MD, MPH; Mary C. Mone, RN; Joseph E. Tonna, MD; Richard G. Barton, MD, FACS; and Benjamin S. Brooke, MD, PhD, FACS, senior investigator.
Souce: American College of Surgeons
Image credit: Wikimedia Commons
Luke A. Martin, MD, a general surgery research resident and the study’s presenting author, in an email to ICU Management & Practice, said: “The novel aspect to our nomogram compared to prior tools/studies is that it is so simple and easy to use. Prior tools require collection of tens of variables on each patient and oftentimes some complex calculations—they just aren’t that practical for clinical practice. Our nomogram uses 7 variables that are available in virtually all ICU patients and then rapidly and easily calculates a numeric risk for ICU readmission.”
Martin and his fellow researchers from the University of Utah School of Medicine, Salt Lake City, developed the risk prediction tool or nomogram to determine a patient's risk level for returning to the surgical intensive care unit (SICU) within 72 hours after discharge. Martin outlined the benefits of this approach - namely avoiding patient care transitions between general wards and the SICU, when the risk of adverse events and errors is high. Readmissions rate are already used to measure quality, and the Centers for Medicare and Medicaid Services reduces reimbursements to hospitals that have excess 30-day readmission rates.
See Also: Is ICU Readmission Associated with Higher Severity of Illness Scores?
In their study, Dr. Martin and his colleagues evaluated the medical records for all SICU admissions at the University of Utah Hospital between April 2010 and July 2015. From among 3,109 SICU admissions, the investigators found that 141 patients were readmitted to the SICU within 72 hours of discharge. The patients had been admitted for trauma, general surgical, vascular and transplant procedures, but cardiac patients were not included, as the hospital has a separate cardiac ICU. From 179 possible demographic, clinical and laboratory measures that could contribute to risk of readmission, the researchers used statistical methods to reduce these to just seven:
- patient age
- respiratory rate
- history of atrial fibrillation
- history of renal insufficiency
- level in the blood of urea nitrogen
- blood glucose level
- level of serum chloride
A total of 40 points (the minimum that an ill SICU patient would likely have, Dr. Martin explained) to 79 points represented a 1 to 5 percent chance, or low risk, for SICU readmission, according to the study abstract. A 6 to 20 percent chance--medium risk--of readmission was 80 to 114 points, and a 21 to 50 percent chance--or high risk--was 115 to 150 points total. The nomogram was validated using data from 577 additional SICU patients.
"The risk prediction model has a moderately good ability to predict readmission to the surgical ICU and takes only about a minute to calculate for each patient," Martin said. "This nomogram allows for a quick and easy assessment of the surgical ICU patient's readiness to leave the SICU."
Martin said that the researchers are studying the accuracy of the nomogram by specific category of surgical procedure, starting with vascular surgical procedures. They are also currently in the process of implementing a protocol to use this tool in all of their ICU patients, and they will study the impact it has on our readmission rate. They plan to validate the tool at other institutions in the future.
Dr. Martin's co-investigators from the University of Utah are Ragheed Al-Dulaimi, MD, MPH; Mary C. Mone, RN; Joseph E. Tonna, MD; Richard G. Barton, MD, FACS; and Benjamin S. Brooke, MD, PhD, FACS, senior investigator.
Souce: American College of Surgeons
Image credit: Wikimedia Commons
Latest Articles
surgery, ICU, readmissions, prediction
A simple and easy to use nomogram can predict the likelihood of readmission to surgical intensive care using just 7 common variables already collected for critical care patients, according to research presented at the 2016 2016 Clinical Congress of the Am