ICU Management & Practice, Volume 21 - Issue 1, 2021
Introduction
During the pandemic caused by the SARS-CoV-2 virus, which produces coronavirus disease 2019 (COVID-19), prone positioning (PP) has been proposed for awake, non-intubated patients hospitalised for pneumonia and respiratory failure.
This therapy is not new and has been described for two decades (Valter 2003), but has become popular around the world over the past year as a result of the large number of patients with acute respiratory failure, as part of an attempt to improve oxygenation and prevent the need for intubation and IMV given the lack of mechanical ventilators and free beds in intensive care units (ICUs) in many hospitals. Observational and some prospective clinical studies have been carried out with a limited number of patients and significant improvement has been observed, with an increase in arterial partial pressure of oxygen (PaO2), decrease in respiratory rate (RR) and decrease in respiratory failure; yet there remains some debate on the benefits of PP in awake patients in terms of achieving a significant decrease in intubation.
Pathophysiologic Considerations for ARDS and Prone Position
Acute respiratory distress syndrome (ARDS) is characterised by progressive inflammation of the alveolar-capillary unit with the infiltration of inflammatory cells and formation of hyaline membranes, significantly affecting gas exchange. It can be triggered by direct lung injury, such as by viral pneumonia (e.g., the SARS-CoV-2 or influenza viruses), or by serious systemic diseases (e.g., sepsis, burns, multiple trauma).
The local and/or systemic inflammatory response generates an endothelial lesion at the pulmonary capillaries, increased permeability of the alveolar-capillary membrane, interstitial oedema, alveolar oedema, diapedesis and activation of lymphocytes, neutrophils and macrophages in the lungs, which generate a greater amount of inflammatory cytokines including metabolites derived from arachidonic acid and interleukins, activating the complement system and reacting with proteases and free radicals, in turn damaging the endothelium and activating the tissue factor pathway, leading to a prothrombotic state.
Multiple mechanisms of hypoxaemia are involved in ARDS: decreased oxygen diffusion, hypoventilation, increased shunting, and ventilation/perfusion (V/Q) mismatch. Clinically, ARDS manifests as dyspnoea, tachypnoea, and increased load on respiratory muscles; arterial gas studies show a decrease in PaO2, a decrease in peripheral arterial oxygen saturation (SpO2), and an increase in partial pressure of carbon dioxide (PaCO2). In ventilatory mechanics there is a decrease in static lung compliance (Cst).
There are large areas of alveolar collapse, predominantly in the gravity-dependent lung regions (posteriorbasal segment) that are richest in capillaries, and therefore changes in body position result in changes in ventilatory mechanics and gas exchange. The supine position does not benefit ventilatory mechanics due to the weight of the heart, the anterior chest wall and the abdomen, which falls on the gravity-dependent pulmonary areas, decreasing Cst and functional residual capacity (FRC), predisposing to the formation of atelectasis and shunts and contributing to hypoxaemia and alveolar hypoventilation (Bower 2020).
On the other hand, in the prone position (PP), the weight of the heart, anterior wall of the rib cage and abdomen falls on the bed, releasing the pressure exerted on the dependent alveoli and causing a rapid improvement in ventilation. In most cases, due to the increase in FRC and tidal volume, a decrease in shunting and atelectatic areas is also observed (Figure 1).
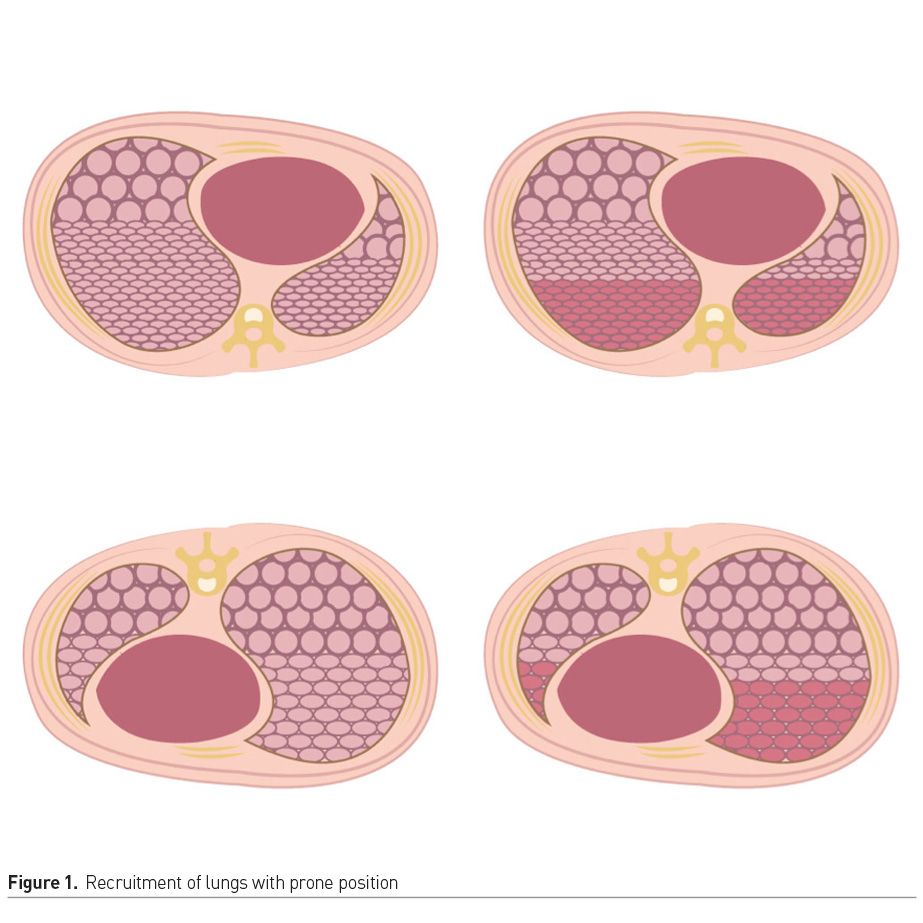
The improvement in ventilatory mechanics is not the only advantage observed in non-intubated patients in the PP. In ARDS there is a capillary derecruitment due to microthrombosis and collapse of the pulmonary vasculature due to hypoxaemia-mediated redistribution, which decreases perfusion. This occurs predominantly in areas with poor ventilation, heavily impacting gas exchange. PP favours more homogeneous ventilation, which improves oxygenation and favours capillary recruitment, benefitting V/Q significantly.
Evidence on Prone Position in Non-Intubated Patients with ARDS
PP has been shown to decrease mortality in patients with ARDS receiving IMV (Guerin 2017); however, there is still no solid evidence that this occurs in non-intubated patients. Some studies conducted in the last two decades have shown improvement in oxygenation in patients with hypoxaemic respiratory failure placed in PP, but research on this topic grew exponentially last year during the COVID-19 pandemic.
The prone position (PP) in awake, non-intubated patients with acute hypoxaemic respiratory failure results in better oxygenation, demonstrated by an increase in PaO2 and SpO2 and the PaO2/FiO2 ratio, while pH increases due to a decrease in the level of PaCO2, and a decrease in RR and work of breathing is also observed (Figure 2). PP is not associated with haemodynamic deterioration (Scaravilli 2015). In addition, PP combined with non-invasive ventilation (NIV) or a high-flow nasal cannula (HFNC) in patients with moderate to severe acute respiratory distress syndrome (ARDS) has been shown to be safe and effective and may prevent intubation (Ding 2020; Perez-Nieto 2020). One further advantage of PP without intubation is that it allows the patient to interact with family during hospitalisation, favouring humanisation in healthcare (Slessarev 2020).
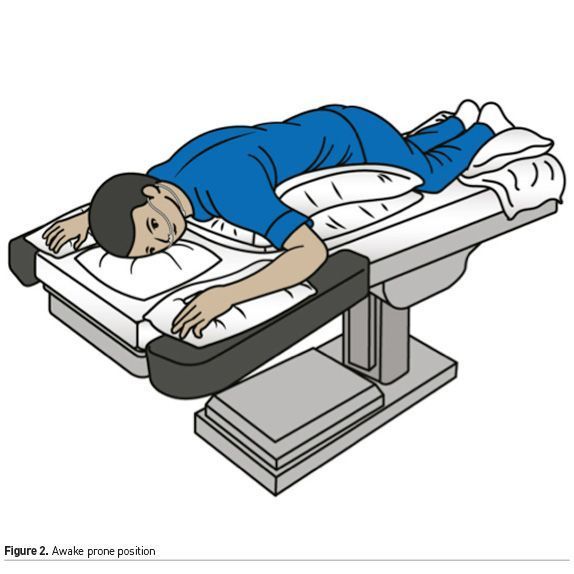
Due to the COVID-19 pandemic and the high global demand for respiratory support, the PP in awake non-intubated patients has become popular in China, and clinical interest has increased rapidly in the Americas and Europe. An early strategy combining the PP together with non-invasive ventilation (NIV) or a high-flow nasal cannula (HFNC) has been reported to be associated with reduced intubation and mortality (Sun 2020) and improved oxygenation compared to patients who were not administered this therapy (Caputo 2020; Thompson 2020; Jagan 2020), and therefore may be beneficial; however, one prospective observational cohort study found no benefit in terms of reducing the intubation rate (Ferrando 2020).
Practical Considerations for Prone Position in Non-Intubated Patients with Respiratory Failure
Due to the great demand for medical attention due to COVID-19, it is appropriate to encourage all patients with respiratory failure, with SpO2<92-94% and RR> 22-28 breaths per minute, to practise the prone position because it is a free, low-risk manoeuvre that requires minimal assistance to perform. The safety and efficacy of PP has been demonstrated in non-intubated patients and so can be performed safely in all areas of care, including the emergency room, ICUs, and other hospital care units (Table 1).
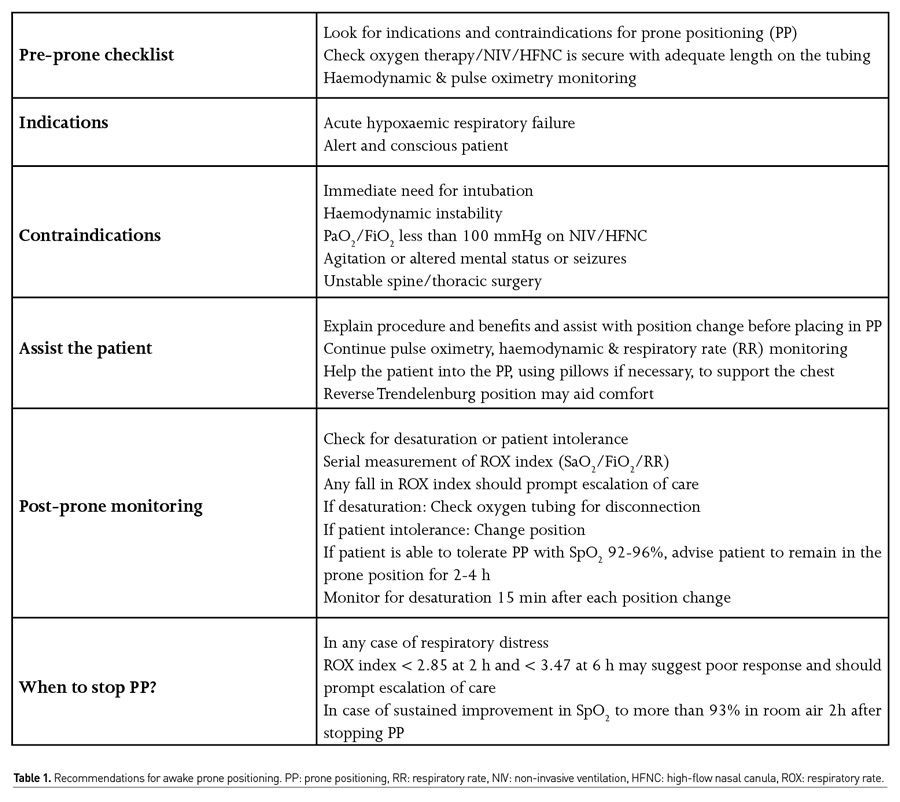
Patients receiving supplemental oxygen through nasal cannulas (HFNCs or LFNCs), oxygen masks, and NIV can safely self-pronate depending on their tolerance and comfort. It should be considered that some more vulnerable groups of patients (the elderly, obese, etc.) may require help to properly position themselves in the PP. Patients must be aware of the procedure, awake, cooperative, and able to communicate on their own and mobilise with minimal assistance.
The recommended duration of PP in non-intubated patients is not clear, but based on the patient’s tolerance, can be set at a minimum of 2 hours every 12 hours or up to 16 hours a day, and alternative lateral and semi-prone positions can be tried if the patient cannot bend fully (Sodhi 2020).
Proposed contraindications to initiating PP in non-intubated patients include patients requiring immediate intubation, airway compromise, respiratory fatigue, patient non-cooperation, neurological deterioration, haemodynamic instability, arrhythmias, spinal instability, pelvic instability, chest trauma, recent abdominal surgery and pregnancy in the 2nd and 3rd trimesters. Some of these contraindications could be relative, but the risk of complications must be taken into account.
All non-intubated patients in the PP should be continuously monitored for treatment failure and the need for greater respiratory support, including IMV or admission to the ICU. Close monitoring of SpO2, vital signs (mainly RR), and dyspnoea is recommended, as well as the use of the ROX index to determine the need to intubate patients (Sryma 2020). An RR> 26 breaths per minute sustained for more than 30 minutes and a work of breathing (WOB) scale score> 5 points are associated with the need for intubation (Apigo 2020).
There is no consensus on when to stop PP therapy, but we can recommend that when the patient is in the supine position and presents a SaO2> 92 to 94%, with RR <22 to 28 breaths per minute and relief of dyspnoea, PP may be discontinued.
In conclusion, PP in awake, non-intubated patients with respiratory failure is a physiology-based ventilatory strategy that improves oxygenation and may decrease the need for intubation. As a minimal risk intervention requiring minimal assistance, it is now a globally accepted therapy to improve oxygenation in patients with respiratory failure, including from COVID-19 (Sodhi 2020). Randomised controlled studies are required to confirm the current theoretical benefits of this therapy.
Conflict of Interest
No authors declare any conflict of interest.












