ICU Management & Practice, ICU Volume 11 - Issue 3 - Autumn 2011
Patients recovering from serious illness have been shown to be at risk for developing Post Traumatic Stress Disorder (PTSD). Studies show that around 1 in 10 patients with an ICU stay of 48 hours or more develop PTSD (Jones et al. 2007).
Since
the 1980s, it has been known that patients don’t tend to remember much from
their time in ICU and as doctors and nurses we thought that was good. If
patients asked questions about their stay they might be told “Don’t worry about
that, look forward now and you will be better as time goes on.” It was also
believed that relatives could answer the patients’ questions.
You might also like:Do ICU Patient Diaries Promote Recovery?
We now know that most of our patients really want to know what happened during their stay and that relatives need assistance in explaining the course of their ICUstay, because this a very chaotic time for them too and their memory might be influenced by anxiety, depression and sleep problems. As a result, these patients can spend a lot of time thinking about what really happened, and become confused by the mingling of reality and dreams, often relating disturbing “memories” of people being killed or injured.
The Diary Projects
The diary projects at Norrköping (Sweden) and Whiston (UK) hospitals started in 1995 and 2002, respectively. The aim of both projects was to recreate the time in ICU for patients and their relatives. This was done by writing and taking photographs of the patients during their ICU stay and then, after one or two months, inviting the patient together with their family to return for a follow-up meeting. At Norrköping, we originally got the idea of writing diaries from a group of nurse assistants, led by Annelie Unosson from Danderyds Hospital, Stockholm. It was only later that we discovered that diaries had been used in Norway (Schou in Sygeplejjen,1984).
We wanted to make the diaries a part of a larger concept; not only writing about the patients’ ICU stay but also taking photographs of significant events and including them in the pages. To achieve this, we had to understand how patients and families felt about these very realistic pictures. In addition, we also needed their evaluation of this whole intervention.
Impact
In our follow-up study which included both centres, patients and relatives reported feeling that the diary was a good idea and that the photographs helped to complete the story (Bäckman and Walther 2001). Here are some of the comments made:
From Patients:
- The diary helps me to understand what I have gone through and I think the idea of having photos and text together is a very good idea.
- By having the diary to show to friends and acquaintances, I find they gain a better understanding. The photos and text provide a complete picture that is difficult to communicate in any other way.
- It has helped us to understand what went on during the time we spent in Intensive Care – something that is difficult when you are in the midst of it all. A valuable document which we will have use for the rest of our lives.
From the Relatives:
- During the time following my friends’ ICU stay, I used to carry the diary with me everywhere. Whenever a question came to me, I had something concrete to refer to. He was very proud of his diary and use to talk a lot about it.
- It is obvious to me that a diary like this should be a routine part of Intensive Care.
- It felt good to be able to express in words the feelings of loss and sadness, thoughts that passed my mind, things I wanted to tell Dad. It was also important for us close relatives to read about Dad’s daily life in Intensive Care and to read how you, the staff, helped him when we were not there.
In a separate study on the impact of ICU diaries on the incidence of PTSD, patients were also asked to give personal comments about diaries (Jones et al. 2010). The study showed that the incidence of PTSD was reduced from 13% down to 5% in those receiving the diary.
Feedback about the diaries was very positive with most of the intervention patients receiving the diary at the one month follow-up and reading it a median of three times (0-20 range), only one patient had not read the diary.
148 (84%) of the intervention patients said that others had read the diary, most commonly family (100%), friends (36%), colleagues (5%) and healthcare staff (4%). When asked what the intervention patients felt helped most only two (1.4%) patients mentioned the meeting with the nurse, while 66 (49%) felt reading the text in the diary was most helpful, 49 (36%) the combination of photographs and text and 21 (15%) the photographs.
Implementing the Diary Concept
The
concept includes four important steps:
1.Starting a Diary
2.Consent
Where possible it should be explained to patient and their relatives that staff are going to create a tool (the diary) during theICU-stay that is meant to be used during recovery both for patients and relatives. At Norrköping, we often start the diary before we get their consent (often from the relatives when the patient is too sick) to write and take photos, make sure that the relatives know that they are also allowed to write. At Whiston, the diaries are explained to the family and the patient (where possible) as a standard therapy and assent/consent is not sought. The patient gives written, retrospective consent once they are well enough to receive the diary.
Documentation
Start the diary by making a summary of what happened to bring the patient into ICU and why it was needed. Write in everyday language in a realistic way and where possible the staff and relatives should write something everyday, if the stay is very prolonged you don’t have to write so often. At Norrköping the diary, without photos, follows the patient to the ward so that staff and relatives and sometimes the patient themselves can write about life on the general ward.
2. Taking Photographs
Take a photograph on the day the diary is started and then at points of change in the patients’ condition. The pictures should not be intrusive but realistic, don’t be afraid of getting close to the patient, they need to be able to recognise themselves. It is important to include staff and relatives in the photographs where possible, as the patient may not remember anything but hallucinations or nightmares.
3. The Follow-up Meeting/Going Through the Diary
At Norrköping, we call the follow-up meeting “The golden meeting” when we can have a two-way conversation, giving the patient a chance to ask about things that they may not be sure really happened. We can ask the patient and relatives how they felt they were taken care of and how the relatives experienced the ICU stay. This is a situation where we as staff can learn a lot about how closely we are meeting their needs. Nowadays we have this meeting at our follow-up clinic, which is run by two ICU nurses together with two nurse assistants, all of them working in the ICU.
At Whiston the patient often receives the diary before they go home from hospital at a point they feel comfortable with going through it. Their family are encouraged to be there at the meeting. Opportunity is given for questions and information given about recovery from critical illness both verbally and in a written form using the ICU Recovery manual (Jones et al. 2003). Patients will then be called back to the follow-up clinic at 2-3 months post ICU discharge to make sure there are no issues remaining that need to be addressed.
4. Evaluation of the ICU-Diary Concept
The evaluation includes the diary, the photos and the follow-up meeting. At Norrköping the patient is sent a questionnaire allowing them to anonymously evaluate the whole intervention. At Whiston the patient and their family are asked directly at the follow-up clinic if they feel the diary and photographs are helpful and if there is anything they would like done differently. The evaluation gives the staff the opportunity to improve the concept.
How to Implement a Diary Programme in Your ICU
What You Need:
- Diary Group- Assemble a diary- group which contains of staff who are very interested in this area of ICU. At Norrköping we have had a mixed group of six people, including nurses, nurse-assistants and the occasional doctor. At Whiston, it is made up of nurses of different grades.
- Books - Acquire some books that can be used as a diary. In Norrköping, we use a A5 lined notebook while at Whiston, we use a spiral bound A5 lined notebooks with a clear plastic cover which can be wiped clean as they are kept at the patients bedside in ICU.
- Camera– Find a digital camera with (simple) instructions how to use it. In Norrköping the staff from the follow-up clinic once a month moves the photos from the camera to a memory stick which is kept in a locked drawer at the follow-up clinic. The photos are collected in “personal boxes”, one for each patient. Before the one/two month follow-up meeting, these photos are printed out on plain paper so they easily can be pasted in the diary. Patients are also able to retreive their photos from the “personal box” on a memory stick. At Whiston, the legal department has directed that the photograph must be printedout straight away and the originaldeleted from the memory card sothat there are no copies. The photographsare kept in a lockeddrawer in the ICU offices untilthey are placed in the diary afterthe patient has given retrospectiveconsent. We also only use plain paperrather than photographic paperto print out onto as it is easyto paste into the diary at the appropriateplace when the patientreceives the diary.
- Guidelines- Guidelines for writing the diaries should be designed by the diary group and made readily accessible. These should cover the reasons for doing the diary, the kind of things that should be written and how the diary should be looked after. For an example of diary guidelines see Jones et al. 2010).
- Information Sheet– In Norrköping we inform the relatives that we have started or shall start a diary and take pictures. We explain that we have done this for more than 15 years and different studies have proven that it is helpful for both patients and relatives. At Whiston, we have an information sheet for relatives which explains about the diary, encourages them to write in it themselves and contains some suggestions about what they could write about.
- Consent Form - At Whiston, we have a retrospective consent form that the patient signs to say they are happy to keep the diary and photographs. A copy of this is filed in the hospital notes.
- Follow-Up Materials– It may be useful to provide an information book about recovery from critical illness. At Norrköping this is given to the patient before they leave the hospital along with verbal and written information about being invited back after one or two months with relatives/friends. When it’s time for follow-up, one of the staff from the follow-up clinic contacts the former ICU-patient (who often is back home) and a meeting is scheduled, and then confirmed by post. Together with the written invitation we also send a questionnaire (SF-36) to be filled in when coming to the meeting. The SF-36 (Ware and Sherbourne 1992) is a questionnaire that deals with HealthRelated Quality of Life and that we ask our patients to fill it in at two, six and 12 months to investigate how their Quality of Life changes as time goes by. At Whiston, the ICU Recovery Manual is provided after the patient has moved to the general wards. An invitation for an outpatient appointment (with their family) within two to three months post-ICU discharge is forwarded by post.
- Private Meeting Space– At Norrköping we have a special room for the follow-up meeting. At Whiston, this is done at the patients’ bedside on the ward or in the ward office if the patient requests privacy.
- Timefor the Follow-Up Meetings- At Norrköping, wenow have a follow-up clinic. Ourdiary group contains two nursesand two nurse assistants with acombined ICU experience of morethan 100 years. Each person in thegroup has 24 hours per monthavailable and they work in pairs(nurse + nurse assistant).The clinicis open on Thursdays (closedduring summer) and every patientthat has had an ICU stay of morethan four days is followed-up,even if they don’t have a diary.Patients also visit the ICU as partof the follow-up visit. At Whiston,the patient is followed up on thegeneral wards as part of the rehabilitation programme and told about
the diary. They then choose when they would like to go through the diary and a
meeting is organised, usually on the ward before they go home. A visit back to
the ICU is offered at the outpatient clinic.
- Other- Diaries where the patient dies. At Norrköping, if a patient dies, the relatives are given the diary and the photos during a follow-up meeting arranged by the staff from the follow-up clinic. At Whiston, the family are contacted three weeks after the patients’ death and offered the written part of the diary. The photographs can not be given to the family as the patients’ written consent has not been obtained (UK law).
Patient is critical, after perforated diverticulitis Patient’s circulation remains very unstable,
requiring a continuous team of staff
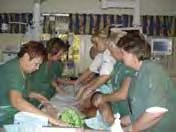
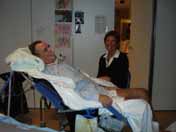
Patient is in recovery; wife visits him (note the Patient returns for
paintings done by grandchild on the walls). follow-up visit.

References:
Bäckman C. Patient diaries in ICU. In: Griffiths RD, Jones C, eds. Intensive care aftercare. Oxford: Butterworth-Heinemann, 2002: 125-29.
Bäckman CG, Orwelius L, Sjoberg F, Fredrikson M, Walther SM. Long-term effect of the ICU-diary concept on quality of life after critical illness. Acta Anaesthesiol Scand. 2010; 54: 736-43.
Backman CG, Walther SM. Use of a personal diary written on the ICU during critical illness. Intensive Care Med. 2001; 27: 426-9.
Bäckman CG, Walther SM. The photo-diary and follow-up appointment on ICU: Giving back time to patients and relatives. In: Ridley S, ed. Critical Care Focus 12: Psychological challenges of Intensive care. Oxford: Blackwell publishing 2005: 72-79.
Bergbom I, Svensson C, Berggren E, Kamsula M. Patients' and relatives' opinions and feelings about diaries kept by nurses in an intensive care unit: pilot study. Intensive Crit Care Nurs. 1999; 15: 185-91.
Combe D. The use of patient diaries in an intensive care unit. Nurs Crit Care. 2005; 10: 31-4.
Cox CE, Docherty SL, Brandon DH, Whaley C, Attix DK, Clay AS, Dore DV, Hough CL, White DB,Tulsky JA. Surviving critical illness: acute respiratory distress syndrome as experienced by patients and their caregivers. Crit Care Med. 2009; 37: 2702-8.
Griffiths RD, Jones C. Filling the intensive care memory gap? Intensive Care Med. 2001; 27: 344-6.
Griffiths RD, Jones C. Seven lessons from 20 years of follow-up of intensive care unit survivors. Curr Opin Crit Care. 2007; 13: 508-13.
Jones C, Backman C, Capuzzo M, Flaatten H, Rylander C, Griffiths RD. Precipitants of post-traumatic stress disorder following intensive care: a hypothesis generating study of diversity in care. Intens Care Med 2007;33(6):978-985.
Jones C, Bäckman C, Capuzzo M, Egerod I, Flaatten H, Granja C, Rylander C, Griffiths R D and RACHEL group. Intensive Care diaries reduce new onset PTSD following critical illness: a randomised, controlled trial. Critical Care 2010; 14: R168.
Jones C, Griffiths RD, Humphris G, Skirrow PM. Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Crit Care Med. 2001; 29: 573-80.
Jones C, Skirrow P, Griffiths RD, GH Humphris, Ingleby S, Eddleston J, Waldmann C, Gager M. Rehabilitation after critical illness: A randomised, controlled trial. Critical Care Medicine 2003;31(10):2456-2461.
Pearlin LI, Lieberman MA, Menaghan EG, Mullan JT. The stress process. J Health Soc Behav. 1981; 22: 337-56.
Ware JE, JR., Sherbourne CD.The MOS 36- item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care. 1992; 30:473-83.







