ICU Management & Practice, Volume 18 - Issue 1, 2018
There are a number of complications related to the use of decompressive surgery. The most important thing to bear in mind is these complications can impair recovery.
What is a decompressive craniectomy?
Decompressive craniectomy is a surgical procedure where a large section of the skull is removed and the underlying dura mater exposed. Primary decompressive craniectomy refers to leaving a large bone flap out after extraction of an intracranial haematoma in the early phase post-TBI. Cranial reconstruction is undertaken between a few weeks and months later with autologous bone (the removed bone flap is stored in the patient’s abdominal wall or a deep freezer) or an implant (titanium or other synthetic material). A secondary decompressive craniectomy is used as part of tiered therapeutic protocols that are frequently used in intensive care units (ICUs) in order to control raised intracranial pressure and ensure adequate cerebral perfusion pressure.
What complications are attributable to a decompressive craniectomy?
- Herniation of the cortex through bone defect
- Subdural/subgaleal effusion
- Syndrome of the trephined (headache, dizziness, irritability, mood swings and behavioural disturbance)
- Seizures
- Hydrocephalus (defined as dilatation of the ventricular system with accompanying clinical features that required shunt placement).
- Infection
- Paradoxical herniation
What complications are attributable to a subsequent cranioplasty?
- Infection
- Bone flap resorption
Can the skull defect cause neurological dysfunction?
Certain patients are particularly susceptible to neurological signs and symptoms relating to the presence of a large skull defect. Clinical presentation can range from symptoms such as headaches, seizures, mood swings, and behavioural disturbances (syndrome of trephined) to neurological deficits due to cortical dysfunction (syndrome of the sinking scalp flap).
The pathophysiology responsible for the neurological manifestations has yet to be established. A number of different theories have been put forward, i.e. direct effects of atmospheric pressure on the brain, alterations in cerebrospinal fluid hydrodynamics, and changes in cerebral blood flow and metabolism.
Given the wide variety of clinical manifestations, the mechanism may be multifactorial.
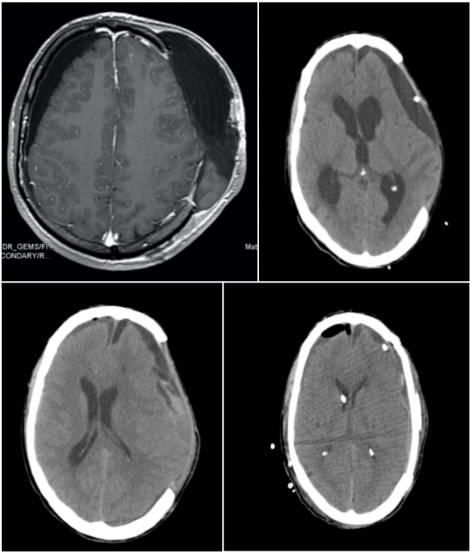
The images correspond to the same patient who presented all the possible complications of a primary decompressive craniectomy after traumatic brain injury: subdural effusions or hygromas, hydrocephalus, paradoxical herniation, seizures, syndrome of trephined, and infection. The final image demonstrates the result after cranioplasty and ventriculoperitoneal shunt and decompressive catheter inside the subdural hygroma.
The most important thing to bear in mind is that we usually see these complications in the ICU. Moreover, we must be very clear about the approach to follow. It is essential to know the probability of neurological deterioration after lumbar puncture or lumbar cerebrospinal fluid (CSF) drainage in the setting of large cranial defects, since this has been observed following decompressive craniectomy and is due to symptomatic herniation.
In the early stage of recovery from traumatic brain injury following decompressive craniectomy, symptoms of paradoxical herniation may be masked and even mistaken for neurological damage from the trauma.
How to avoid complications
Neurosurgeons, intensive care specialists and the other professionals involved in the treatment of these patients need to carefully decide who will benefit from immediate decompressive craniectomy and who are best treated by initial monitoring and medical treatment of intracranial hypertension. Correct selection for decompressive surgery is required in order to avoid an intervention that increases survival at the expense of a persistent vegetative outcome.
In addition to using the appropriate surgical technique, the patient’s neurological condition should be followed closely, looking out for signs and symptoms of syndrome of the trephined.
Tapping and shunt treatment of CSF subdural hygromas should be avoided, where possible. There is also a risk of paradoxical herniation in those patients with a skull defect, who undergo lumbar puncture and ventriculoperitoneal shunt.
A cranioplasty procedure is necessary when the patient is clinically improved. Nevertheless, it is best performed as early as possible, since atmospheric pressure may cause local vascular dysfunction.
Conclusions
Despite the successes and worldwide application of decompressive craniectomy, the procedure remains controversial and there continue to be uncertainties regarding its appropriate application. These areas of controversy can be grouped into four categories: patient selection, timing, technical considerations, outcome results and complications. In this article I have only described the complications.To what degree patients are affected by the symptoms of syndrome of the trephined is difficult to determine, since many patients are in the severe head injury recovery phase.
Several studies have demonstrated that hydrodynamic abnormalities present prior to cranioplasty were reversed after the bone flap was replaced. In some cases, this was accompanied by a clinical improvement. However, this was not always so.
Technically speaking, whilst the procedure is straightforward, the complications can impair recovery. Not least it represents an aggressive intervention associated with significant morbidity, not only from the initial decompression but also from the subsequent reconstructive cranioplasty.
The aim of this brief review is to emphasise that although decompressive surgery is indicated in some neurocritical patients for cerebral oedema management, the technique is not without significant complications. Furthermore, said complications are not always reversible, and may contribute to a worsening of the neurological outcome of these patients.
References:
Honeybul S (2010) Complications of decompressive craniectomy for head injury. J Clin Neurosci, 17: 430-45.
Honeybul S (2014) Neurological susceptibility to a skull defect. Surg Neurol Int, 5: 83.
Honeybul S et al. (2018) Long-term outcome following decompressive craniectomy: an inconvenient truth? Curr Opin Crit Care, 23 Jan. doi: 10.1097/MCC.0000000000000481. [Epub ahead of print]
Hutchinson PJ et al. (2016) Trial of decompressive craniectomy for traumatic intracranial hypertension. N Engl J Med 375: 1119-30.
Nasi D et al. (2016) Paradoxical brain herniation after decompressive craniectomy provoked by drainage of subdural hygroma. World Neurosurg, 91: 673: e1-4.







