ICU Management & Practice, Volume 16 - Issue 4, 2016
As awareness has grown of the great distress intensive care
patients may suffer, units have begun recruiting psychologists to their teams. Intensive
care unit psychologists aim to assess and reduce distress for patients,
families and staff, to improve outcomes. This paper summarises research on the
psychological impact of critical illness, highlights the growth of critical
care health psychology as a speciality, and discusses potential roles of
psychologists and the evidence base for psychological interventions in critical
care departments.
It is now widely recognised that the experience of critical illness, with admission to an intensive care unit (ICU), has a powerful psychological impact on people. A body of evidence about the prevalence of acute stress and frightening psychological experiences in the ICU and adverse psychological outcomes post-ICU has grown. Consequently, the necessity of psychological assessment and support of patients has gained acceptance. Since families of critically ill patients and ICU staff can also become stressed or traumatised, they may also require psychological input. With the gradual dissemination of these research findings among clinicians, critical care departments have started to employ psychologists as key colleagues in the multidisciplinary team.
Psychological Impact of Critical Care
The psychological impact of a critical care admission can be severe. It is known that patients may experience extreme stress (Samuelson 2007; Wade et al. 2012) and altered states of consciousness (Ely et al. 2001). Subsequently there is a high prevalence of psychological morbidity, including post-traumatic stress disorder (PTSD), depression and anxiety among survivors (Wade et al. 2013). Studies have found that more than half of critical care patients suffered symptoms of a psychological disorder after their admission. Cognitive deficits in memory, attention and executive function, affecting activities of daily living, are also common (Pandharipande et al. 2013).
Patients are exposed to multiple stressors in the ICU, including illness, pain, sleep deprivation, thirst, hunger, dyspnoea, unnatural noise and light, nakedness and lack of dignity, inability to communicate, isolation, fear of dying and witnessing other people suffering and dying. They may also have strong emotional or behavioural reactions in response, including anxiety, panic, low mood, anger or agitation. Interventions, such as mechanical ventilation (MV) or invasive monitoring for cardiovascular support, may be difficult for patients to tolerate. Furthermore, the onset of delirium, including frightening symptoms such as hallucinations and paranoid delusions, is common in intensive care. Flashbacks, nightmares and traumatic memories of hallucinations and delusions may form part of post-ICU PTSD, while delirium is associated with later cognitive impairment.
There is also evidence that the critical care experience is traumatic for families, with relatives frequently suffering from PTSD (33% in one study) once their family member has left the ICU (Davidson et al. 2012). Critical care staff have been shown to suffer from high rates of stress, burnout and PTSD in a number of large studies (Moss et al. 2016).
Need for Psychological Assessment and Support
A landmark document on the organisation of critical care services in the UK (Department of Health 2000) recognised that the ICU environment was “extremely distressing” for relatives and patients, who needed support from staff. However, psychological support was “difficult and time-consuming”, and senior staff and appropriate materials were needed to deliver it. A National Institute for Health and Care Excellence (NICE) guideline (Tan et al. 2009) stated that patients should be assessed during their critical care stay for acute symptoms such as anxiety, depression, panic episodes, nightmares, delusions, hallucinations, intrusive memories, flashback episodes and underlying psychological disorders, to determine their risk of future psychological morbidity. Furthermore, psychological support should be provided to aid rehabilitation and recovery in critical care units, on general wards, and in the community. However, it is not known to what extent psychological assessment and support are really carried out in ICUs.
Research suggests that acute stress in the ICU may be one of the strongest patient risk factors for poor psychological and cognitive outcomes after intensive care (Wade et al. 2012; Davydow et al. 2013). Therefore it is important to detect and minimise acute tress where possible. It is known that healthcare staff who have not been trained in mental health may find it difficult to recognise that a patient is suffering from acute stress, hallucinations or delusions. However, tools to detect distress in the ICU are now available. The Confusion Assessment Method for the ICU (CAM-ICU) can be used by staff to detect delirium in critical care patients (icudelirium. org/delirium/monitoring.html). An intensive care psychological assessment tool (IPAT) has recently been validated and may be used by trained critical care staff to detect acute stress and indicate the risk of future psychological morbidity (uclh.nhs.uk/OurServices/Consultants/Documents/Dorothy%20Wade%20profile%20documents/IPATTool.pdf).
Families of critical care patients also frequently need support to deal with anxiety and fatigue, to comfort them when they learn that a loved one is dying, or after a death. Conflict may arise between family members who have different views on a patient’s care, or between families and staff, particularly around withdrawal of support or non-resuscitation orders.
Staff in critical care have much higher than average rates of stress and burnout than other hospital staff (Moss et al. 2016). This may be related to the responsibility of maintaining lives through sophisticated technological interventions; difficult emotions created by caring for patients who are dying or who die, and a culture in which staff may be perfectionist, driving themselves to provide high standards of care, without utilising appropriate self-care strategies. Conflict between patients’ families who are upset, angry or grieving, and staff who are not trained to deal with these emotions, can also escalate. Excessive stress can lead to staff going on long-term sick leave or eventually leaving the service. The United States critical care societies’ collaborative has recently issued a call to action on burnout syndrome (Moss et al. 2016).
Growth of
Critical Care Psychology
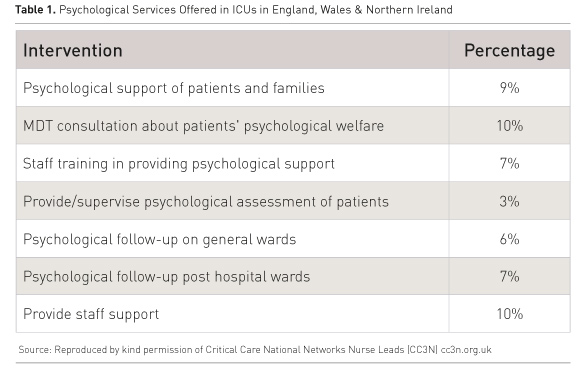
Acute stress, the effects of delirium, adverse cognitive and psychological outcomes, and family and staff stress are complex matters to manage within a highly complex medical environment. There is evidence that critical care departments are now starting to employ fully-trained, usually senior, psychologists to help manage these issues. A workforce survey of allied health professionals in critical care in England, Wales and Northern Ireland (Critical Care Network National Nurse Leads 2016) found that 23 of 135 responding units (17%) offered a psychological support service to families and patients. However, the true proportion of ICUs in England, Wales and Northern Ireland offering psychology could be smaller, given that 270 units were sent a survey and 217 were returned. Many units did not complete the psychology spreadsheet, presumably because they have no psychology provision. In 15 units the service was provided by practitioner psychologists (health, counselling or clinical). Of 27 identified psychologists, 15 were senior psychologists in the band 8 range* (NHS Agenda for Change payscales range from 1-9, see healthcareers.nhs.uk/about/careers-nhs/nhs-pay-and-benefits/agenda-change-pay-rates), while 12 were more recently qualified band 7s. The most frequent provision was one psychologist one day a week (range 5-37.5 hours per week). In some units the psychological service was provided by psychotherapists, counsellors, follow-up nurse specialists, bereavement nurses or psychology support workers (band 6s). Table 1 highlights psychological support services offered in a given percentage of the 135 units.
A survey of health psychology in the USA received 175 responses (Stucky et al. 2016). It found that psychologists are involved in critical care settings in various roles. It was not known how frequently psychologists were consulted or what specific services were most effective, valued, or desired.
Role of Psychologists
Now that psychologists are taking their place in the critical care team, what should their role be? The role has been recognised and described in a section of the UK Guidelines for the Provision of Intensive Care Services (Howell and Wade 2015). Psychologists can play a vital role in the acute critical care setting, and as part of patients’ follow-up care, both in- and post-hospital. They are also able to help maintain a healthy working environment and manage workplace stress.
In the acute setting, psychologists should supervise the psychological and cognitive assessment of all patients, both in the critical care unit, and after transfer to other wards, as well as providing or supervising psychological support to patients and relatives who are highly stressed or traumatised. They can also help staff manage communications with distressed families. Psychologists can provide training to increase staff knowledge and understanding of psychological reactions, delirium, stressors in the critical care environment, and psychological and cognitive outcomes of critical illness. They may also deliver training to increase staff competency in providing psychological support to patients who are distressed, agitated, or delirious. Similar types of training have proved successful in cancer services (for example the SAGE & THYME® model (UHSM Academy 2012)).
Psychologists should play a key role in the multidisciplinary team (MDT), attending ward rounds, and being available for consultation on matters such as communication, sleep, effects of sedation, anxiety, stress, mood, delirium, and family issues. They should be involved in developing holistic care plans for long-stay patient.
The psychologist should also play a full role in follow-up care, including assessment and support of patients who suffer traumatic stress reactions such as flashbacks of frightening delusions, or who become depressed in the hospital after discharge from ICU. Their role should also include the psychological (emotional and cognitive) assessment of patients attending critical care follow-up clinics. In a well-resourced follow-up service, a psychologist could ideally offer sessions of CBT (including trauma-focused CBT) and other evidence-based treatments. These sessions would be specifically tailored for critical care patients. If not possible, the critical care psychologist should liaise with GPs and/or community mental health teams regarding appropriate psychological treatment or cognitive rehabilitation in the community.
Finally, psychologists should play a role in addressing stress and burnout among critical care staff. This could include advising senior management at an organisational level on systemic issues influencing patient and staff wellbeing, as well as organising a wellbeing programme for staff (individual and group sessions as well as teaching and proactive work) and coaching or reflective sessions with senior management. (M Smithies & J Highfield, University Hospital Wales, Cardiff, personal communication).
This is a highly complex role in a sensitive, complex, medical environment. To provide a coordinated service across the critical care department, ideally a consultant-level health, clinical or counselling psychologist should be employed to ensure the necessary seniority, experience and expertise. Additional junior psychology staff could be employed to support the senior psychologist, according to numbers of beds, specialities or units within the department. With such a multi-faceted role, and high-level need, burnout is a risk for the senior psychologist, similarly to other critical care staff, if the psychology service is not properly structured and staffed.
Evidence Base for Psychological Interventions in Critical Care
There has been little evaluation of psychological interventions for critical care patients to date, but a recent systematic review suggests that a range of non-pharmacological measures, including psychological interventions, could help to reduce both short- and medium-term stress (Wade et al. 2015). For example, an intervention to introduce psychology input to an Italian critical care unit reduced the incidence of post-traumatic stress disorder (PTSD) a year later with a large effect size (using a historical, not randomised control design) (Peris et al. 2011). Small studies point to the value of cognitive rehabilitation, potentially beginning as early as the critical care admission (Jackson et al. 2012).
Editorials have emphasised an increased need for psychological interventions in the critical care setting to be evaluated (Hatch et al. 2011), and such studies are now underway. A cluster randomised controlled trial in 24 hospitals in the UK, aims to evaluate the clinical and cost-effectiveness of a complex, nurse-led, preventative psychological intervention in critical care (icnarc.org/Our-Research/Studies/Poppi/About). A Danish trial to evaluate a nurse-led psychological recovery programme beginning 1-10 months post-ICU, found no benefit across a range of outcomes (Jensen et al. 2016). Other post-ICU interventions undergoing evaluation are cognitive rehabilitation (Jackson et al. 2012), coping skills training (Cox et al. 2012) and mindfulness (Cox et al. 2014). The key question is whether psychological interventions can improve patients’ clinical outcomes.
Senior psychologists working in intensive care should ideally have the research expertise to contribute to, as well as keep abreast of, the evolving evidence base for this relatively new but rapidly expanding role.
Conclusion
As recognition of intensive care-related psychological distress grows, senior practitioner psychologists are being recruited to the multidisciplinary team, to assess and manage acute and long-term stress in patients, families and staff. Further evaluation of the effect of specific psychological interventions on critical care outcomes will help to refine the ICU psychologist’s role.
Abbreviations
ICU intensive care unit
IPAT intensive care psychological assessment tool
MV mechanical ventilation
References:
Cox CE, Porter LS, Hough CL et al. (2012) Development and preliminary evaluation of a telephone-based coping skills training intervention for survivors of acute lung injury and their informal caregivers. Intensive Care Med, 38(8): 1289-97.
PubMed ↗
Cox CE, Porter LS, Buck PJ et al. (2014) Development and preliminary evaluation of a telephone-based mindfulness training intervention for survivors of critical illness. Ann Am Thorac Soc, 11(2): 173-81.
PubMed ↗
Critical Care Network – National Nurse Leads (2016) National critical care non-medical workforce survey: overview report. [Accessed: 20 October 2016] Available from noeccn.org.uk/resources/Documents/JCF/National%20Critical%20Care%20NMWS%20Report%202016%20V2.pdf
Davidson JE, Jones C, Bienvenu OJ (2012). Family response to critical illness: postintensive care syndrome-family. Crit Care Med, 40(2): 618-24.
PubMed ↗
Davydow DS, Zatzick D, Hough CL et al. (2013) In-hospital acute stress symptoms are associated with impairment in cognition 1 year after intensive care unit admission. Ann Am Thorac Soc, 10(5): 450–457.
PubMed ↗
Department of Health (2000) Comprehensive critical care: a review of adult critical care services. London: Department of Health. [Accessed: 30 September 2016] Available from webarchive.nationalarchives.gov.uk/20130107105354/http:/www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4082872.pdf
Ely EW, Siegel MD, Inouye SK (2001) Delirium in the intensive care unit: an under-recognized syndrome of organ dysfunction. Semin Respir Crit Care Med, 22(2): 115–26.
PubMed ↗
Hatch R, McKechnie S, Griffiths J (2011). Psychological intervention to prevent ICU-related PTSD: who, when and for how long? Crit Care, 15(2): 141.
PubMed ↗
Howell D, Wade D (2015). Practitioner psychologists. In: Guidelines for Provision of Intensive Care Services, Chapter 2.2.10, pp. 48-50. London: Faculty of Intensive Care Medicine and Intensive Care Society. [Accessed: 1 October 2016] Available from ficm.ac.uk/sites/default/files/Core%20Standards%20for%20ICUs%20Ed.1%20(2013).pdf
Jackson JC, Ely EW, Morey MC et al. (2012) Cognitive and physical rehabilitation of intensive care unit survivors: results of the RETURN randomized controlled pilot investigation. Crit Care Med, 40(4): 1088-97.
PubMed ↗
Moss M, Good VS, Gozal D et al. (2016) An Official Critical Care Societies Collaborative Statement: burnout syndrome in critical care healthcare professionals: a call for action. Crit Care Med, 44(7): 1414-21.
PubMed ↗
Pandharipande PP, Girard TD, Jackson JC et al. (2013) Long-term cognitive impairment after critical illness. N Engl J Med, 369(14): 1306-16.
PubMed ↗
Peris A, Bonizzoli M, Iozzelli D et al. (2011) Early intra-intensive care unit psychological intervention promotes recovery from post traumatic stress disorders, anxiety and depression symptoms in critically ill patients. Crit Care, 15(1): R41.
PubMed ↗
Samuelson KA (2007) Stressful memories and psychological distress in adult mechanically ventilated intensive care patients - a 2-month follow-up study. Acta Anaesth Scand, 51(6): 671-8.
PubMed ↗
Stucky K, Jutte JE, Warren AM et al. (2016) A survey of psychology practice in critical-care settings. Rehabil Psychol, 61(2): 201-9.
PubMed ↗
Tan T, Brett SJ, Stokes T, Guideline Development Group (2009) Rehabilitation after critical illness: summary of NICE guidance. BMJ, 338:b822.
PubMed ↗
Wade DM, Howell DC, Weinman JA et al. (2012).
Investigating risk factors for psychological morbidity three months after intensive care: a prospective cohort study. Crit Care, 16(5): R192.
PubMed ↗
Wade D, Hardy R, Howell D et al. (2013). Identifying clinical and acute psychological risk factors for PTSD after critical care: a systematic review. Minerva Anestesiol, 79(8): 944–63.
PubMed ↗
Wade DM, Hankins M, Smyth DA et al. (2014). Detecting acute distress and risk of future psychological morbidity in critically ill patients: validation of the Intensive care psychological assessment tool. Crit Care, 18(5): 519.
PubMed ↗
Wade DM, Moon Z, Windgassen SS et al. (2016) Non-pharmacological interventions to reduce ICU-related psychological distress: a systematic review. Minerv Anestesiol, 82(4): 465-478.
PubMed ↗








