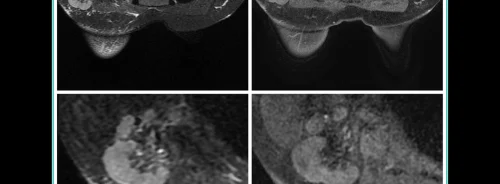
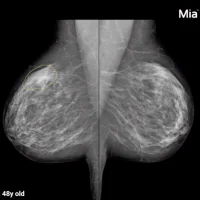
While the tattoo trend continues, many newly inked Generation X and Millennials have started undergoing regular breast screenings. Radiologists have been spotting pigment in lymph nodes much more frequently, and more disturbingly, tattoo pigment can mimic malignant breast cancer.
With 38% of Millennials having at least 1 tattoo, 32% of Generation X and 15% of Baby Boomers, the prevalence of tattoos has been increasing in recent decades - with women especially. 15% of women reported having at least 1 tattoo in 2003 compared to 31% in 2016. The same poll showed that half of women aged 30-39 had a tattoo in 2016. As these women reach the age of 40 and start obtaining screening mammograms, the percentage of patients with tattoos routinely seen by breast imagers will continue to increase.
You might also like: While COVID-19 has resulted in decreases in absolute imaging volumes, imaging utilisation on a per-patient basis has not been reported. A surprising new study published in Clinical Imaging shows that clinicians are more likely to request imaging for non-respiratory patients during the COVID-19 pandemic.
Tattoos are created by repeated piercing the skin with a small needle and injecting a small amount of ink into the dermis. Tattoo ink comprises of two main components: a dye which is commonly a heavy metal containing compound such as iron oxide, carbon or mercury and a water based or alcohol solvent. It has been well established that tattoo pigments can migrate to the regional lymph nodes through the lymphatic vessels after being phagocytosed by the dermal macrophages. Such pigment can manifest clinically for several years after its application.
Distinguishing tattoo pigment from metastases secondary to occult breast malignancies masquerading as intranodal calcification on imaging may be extremely difficult for clinicians.
Distinguishing tattoo pigment from metastases secondary to occult breast malignancies masquerading as intranodal calcification on imaging may be extremely difficult for clinicians. Even cutting-edge imaging modalities can be associated with pitfalls. Tattoo pigment may generate false positive findings on positron emission tomography scan. Iron oxide containing inks have been reported to result in burning or tingling sensation in the skin during magnetic resonance imaging.
Aside from tattoo pigment, other benign pathologies that resemble similar radiological findings include fat necrosis, gold deposits after chrysotherapy for treatment of rheumatoid arthritis, fat necrosis and granulomatous diseases such as tuberculosis and sarcoidosis These metal oxides are radiopaque and can appear similar to calcifications on imaging. The body responds to this injected material by removing the smaller pigment molecules through passive transport along lymphatic vessels and active transport via phagocytosis within days of exposure. Tattoo pigment travels systemically via the bloodstream to deposit in the liver and regionally to lymph nodes where it remains even if the original tattoo is removed by laser surgery or dermabrasion.
Migration of tattoo pigment particles from the dermis to lymph nodes can mimic other disease processes at surgery and on imaging. Gross black appearance of a sentinel lymph node is highly suggestive of metastatic disease when lymph node dissection is performed for melanoma treatment. Therefore, tattoo pigment mimicking melanoma metastases can result in unnecessary complete nodal dissection rather than termination of the dissection. During breast surgery, a superficially located pigmented axillary lymph node may mimic a sentinel node with blue dye on visual inspection and be incorrectly removed while the true sentinel is left behind, potentially understaging the patient, thus immuno-histological studies should be performed on lymph nodes for melanoma treatment and dual tracer technique for breast cancer lymph node mapping may be necessary to correctly evaluate lymph nodes in patients with tattoos.
So does the tattoo trend in fact affect mammograms?
Short answer? Yes. There are several case studies that discuss clinical management of these patients. Clinical history of prior tattoos and physical exam of the patient is necessary to guide management. If biopsy is warranted to confirm the specific diagnosis, suspicion of tattoo pigment laden lymph nodes should be shared with the pathologist.
Photo: National Cancer Institute on Unsplash