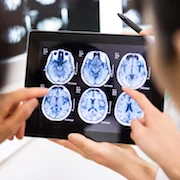
A new study that will be presented next week during the annual meeting of the Radiological Society of North America (RSNA) shows MRI brain scans are better at predicting the development of Alzheimer’s disease in patients compared to clinical tests commonly used today.
Until now, the standardized questionnaires and tests to measure cognition and those administered to locate a gene variant associated with higher risk of Alzheimer’s disease commonly used as prediction models have fallen short with 70 -71 percent accuracy rates, leaving out a large number of the population who will go on to develop the disease.
In the study, researchers have now achieved 89 percent accuracy in predicting which patients would later develop Alzheimer’s disease using MRI measures of white matter integrity which could speed interventions that slow the course of Alzheimer’s disease or delay its onset.
You may also like: PET imaging tool measures synaptic loss in Alzheimer's disease
"As we develop new drug therapies and study them in trials, we need to identify individuals who will benefit from these drugs earlier in the course of the disease," said lead author of the study Cyrus A. Raji, assistant professor of radiology at the Mallinckrodt Institute of Radiology at Washington University School of Medicine in St. Louis, who also highlighted that "Alzheimer's disease is the most common cause of dementia in the world and is expected to increase globally, and especially in the U.S., as the population gets older."
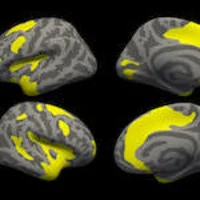
Using diffusion tensor imaging (DTI) in MRI exams that help assess the condition of the brain’s white matter provides a promising option for analyzing dementia risk. DTI provides different metrics of white mater integrity including fractional anisotropy (FA) that measures how well water molecules move along white matter tracts. Higher FA value shows water is moving normally along the tracts and lower value shows the tracts may be damaged.
Dr. Raji says that with DTI you look at the movement of water molecules along white matter tracts, the telephone cables of the brain and adds, “when these tracts are not well connected, cognitive problems can result.”
They performed DTI brain exams on 61 patients from the Alzheimer’s Disease Neuroimaging Initiative, multisite major study researching the progression of the disease, in order to quantify the differences in those who decline from normal cognition or mild cognitive impairment to Alzheimer’s dementia compared to controls who do not develop dementia.
"DTI performed very well compared to other clinical measures," Dr. Raji said. "Using FA values and other associated global metrics of white matter integrity, we were able to achieve 89 percent accuracy in predicting who would go onto develop Alzheimer's disease. The Mini-mental State Examination and APOE4 gene testing have accuracy rates of about 70 - 71 percent."
In more detailed analysis of the white matter tracts performed on about 40 of the study participants, the technique reached 95% accuracy, according to Dr. Raji. He also stated that as many people already receive MRI as part of their care, DTI could add significant value to the exam without substantially increasing the costs.
These MRI measures of white matter integrity may help slow the course of the disease or delay its onset if it could help faster intervention.
"Research shows that Alzheimer's disease risk can be reduced by addressing modifiable risk factors like obesity and diabetes," Dr. Raji said. "With early detection, we can enact lifestyle interventions and enlist volunteers into drug trials earlier."
The results may point to a future role in DTI for diagnosing those at risk for Alzheimer’s disease but more work is needed before this is ready for routine clinical use.
Image Credit: iStock
References:
Latest Articles
Dementia, MRI, RSNA, DTI, brain scans, alzheimers, Mallinckrodt Institute of Radiology, Washington University School of Medicine, fractional anisotropy, Alzheimer’s Disease Neuroimaging Initiative, #RSNA18
A new study that will be presented next week during the annual meeting of the Radiological Society of North America (RSNA) shows MRI brain scans are better at predicting the development of Alzheimer’s disease in patients compared to clinical tests commonl