Openness and honesty when things go wrong in healthcare are the ideal to aim for. However, the implications for breast screening programmes when interval cancers are diagnosed are not straightforward, said Eleanor Cornford, consultant radiologist, Nottingham Brast Institute, UK, speaking at the Radiological Society of North America (RSNA) annual scientific meeting in Chicago last week. When is the best time to tell a patient that their cancer was missed in screening? What if they do not wish to know the results of the audit?
In the UK, a regulation on duty of candour (meaning the quality of being open and honest) came into force in 2015, under the Health and Social Care Act 2008. Regulation 20 - duty of candour states:
“The intention of this regulation is to ensure that providers are open and transparent with people who use services and other 'relevant persons' (people acting lawfully on their behalf) in general in relation to care and treatment. It also sets out some specific requirements that providers must follow when things go wrong with care and treatment, including informing people about the incident, providing reasonable support, providing truthful information and an apology when things go wrong.”
The regulation also states that “As soon as reasonably practicable after becoming aware that a notifiable safety incident has occurred a registered person must notify the relevant person that the incident has occurred …and provide reasonable support to the relevant person in relation to the incident, including when giving such notification."
See Also: Fewer ‘Call Backs’, Improved Breast Cancer Detection With DBT
A notifiable incident means an unintended or unexpected incident that occurred in respect of a service user that could result in or appears to have resulted in death, severe harm, moderate harm or prolonged psychological harm to the service user.
Due to the implications of the regulation for informing women diagnosed with interval cancers and for other national screening programmes, a group was set up in the UK to provide guidance. Interval cancers are those cancers that are diagnosed within the 3-year period after a normal (negative) screening result. These include false negatives, complication of screening tests or false positive diagnoses.
The Disclosure of Audit guidance from 2006 forms the basis of the current best practice guidelines on duty of candour for screening programmes, published in September 2016. These include disclosure of results of audits undertaken following a diagnosis for a screened condition (positive) subsequent to a screening episode.
In the UK there are no current standards for “acceptable” rates of false negatives and national data are not available, said Cornford. However, standards for interval cancers exist. There are three categories used in the screening programme that determine what are notifiable incidents. If most radiologists would have recalled a patient for further screening after a mammogram, that is notifiable. ‘Clear misses’ are notifiable, but have to be defined consistently between screening centres, and work on categorisation of interval cancers is continuing, added Cornford.
Patient Information
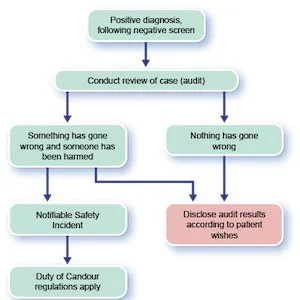
The leaflet provided to women coming for breast screening informs the patient that screening is not 100 percent accurate, that not all cancers will be detected, that interval cancers are not unexpected, and that at time of diagnosis the patient should be provided with information about the review process of previous mammograms. A flowchart and pictogram are planned to assist with discussions with patients. If the patient doesn’t want to know the results of the review, the key worker has to record that decision, and the patient can change her mind at any point.Cornford emphasised that patient choice is important, as the patient may not wish to know the results of the review of previous screening mammograms. That is her right, and the duty of candour regulation and advice on implementation respects that. The timing of disclosure is very important, and “as soon as reasonably practicable” may not be in the patient’s best interest.
The duty of candour concept is to be commended, concluded Cornford. However when it is applied it must be handled very carefully to avoid unnecessary additional harm to patients, by telling them information at the wrong point.
Claire Pillar
Editorial director, HealthManagement
Image credit: PHE Screening
Latest Articles
Candour, interval cancers, safety, patients
Openness and honesty when things go wrong in healthcare are the ideal to aim for. However, the implications for breast screening programmes when interval cancers are diagnosed are not straightforward, said Eleanor Cornford, consultant radiologists, Notti