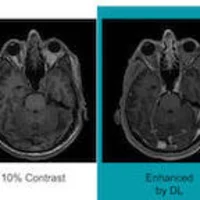
A 3D functional infrared imaging tool trialled in Israel was affordable and acceptable to patients, and can be used as a selection tool for high-risk women to be screened with MRI. Miriam Sklair-Levy, Israel, Sheba Medical Center, presented an evaluation study at the Radiological Society of North America annual scientific meeting in Chicago last week.
The total examination time is 21 minutes and the tool does not use compression. The woman sits in a cool room (temperature 20-21 degrees) while the machine scans. The imaging acquisition time is 6 minutes, and the results are immediately available to the physician, The system uses multiparametric machine learning to generate a risk score, based on multiparametric evaluation of metabolic imaging biomarkers that include vascular asymmetry as a prognostic biomarker. Every score above 0 is considered high risk.
The prospective trial was conducted between 2013 and 2015, including 230 women at high risk of developing breast cancer, and evaluated the diagnostic accuracy of the 3DIRI risk assessment score. There were 3 screening rounds during 24 months. Screening included the 3DIRI system, MRI, US and digital mammography. All the exams were read by a breast radiologist. Women with a negative screening mammography or ultrasound, but positive 3DIRI’s risk assessment score (e.g. likelihood for cancer), were referred to MRI.
If the 3DIRI score was above 0 but screening was negative, an additional MRI was performed. 18% of the women had positive 3DIRI results. There was 1 false negative on 3DIRI but 7 were positive for cancer, yielding a sensitivity, specificity, PPV and NPV of 87.5%, 82.9%, 9.33% and 99.7% respectively. In two women, cancer was missed by mammography and ultrasound, however, correctly classified as suspicious by 3DIRI and was detected by a subsequent MRI. The recall rate increased from 18% to 27%. Sklair-Levy observed that most of the women had dense breasts. She concluded that this tool can provide risk assessment for the likelihood of cancer with high accuracy in a population of women that are at high risk for breast cancer, and could be used as a selection tool for MRI, in an affordable procedure.
Added Value of Mammography
Suzan Vreemann, Njimegen, the Netherlands, presented a retrospective single centre study on the added value of mammography in a population of women with intermediate and high risk of developing breast cancer who are screened annually with MRI. This population includes women with a BRCA gene mutation, a family history without known BRCA gene mutation, personal history of breast cancer, and other groups, such as those who had previously received radiation to the chest. Breast MRI has a sensitivity of up to 90% and high risk women are already screened with MRI. Their study analysed data from 2003 to 2014 and looked at cancer yield, tumour and patient characteristics. Patients included were aged 30-60 years, who received an MRI and mammography yearly.Results
55 detected with both modalities67 detected by MRI alone
13 detected with mammography alone
2028 women at increased risk, 6556 screening rounds (median: 2 screening rounds)
The researchers concluded that mammography has added value in older women, and that cancers detected with mammography alone are mostly small or non-invasive.
Claire Pillar
Editorial director, HealthManagement
Latest Articles
screening, breast cancer, high risk
Two studies on screening women at intermediate or high risk of developing breast cancer were presented at the Radiological Society of North America meeting 2016.