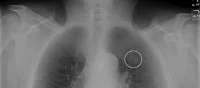
With screening for lung cancer likely to be funded in the United States in the near future for patients at high risk for lung cancer, radiologists need to consider how to communicate with those patients that need to get low dose CT scans every year, according to Prof. James Ravenel of the Medical University of South Carolina, speaking at the Radiological Society of North America’s annual meeting.
Radiologists are used to evaluating images and looking at the data related to lung cancer screening, but may not have thought about the impact on the individual patient. However, Ravenel suggested that the critical questions for the radiologist when thinking about what lung cancer screening means is for the individual what are their personal characteristics conditions and preferences, what do they expect will happen during the lung cancer screening process, what are their options and the benefits and harms of those options, and how can they participate in a way that improves my outcomes that are important to them. Radiologists also need to consider how they can aid clinicians in making the best decisions and help educate their patients.
The challenges in lung cancer screening are many, said Ravenel. Smokers have poor access to healthcare, are less likely to want to participate in any screening procedure, and in general have a lesser degree of understanding of the disease risks and the benefits of a screening test. In addition participating in screening may not encourage them to quite smoking. Smokers are more likely to be male, not Caucasian, with a lower level of education and poor health status, more likely to have had a previous cancer, less likely to have health insurance or unable to identify a usual source of healthcare. So the challenge is not just getting the screening test done but getting them in to healthcare in general. Even participants in the National Lung Cancer Screening Trial had no change in their attitudes on the perceived benefit of quitting and screening.
Smokers believe that screening is less likely to result in a good chance of survival, they are less likely to consider CT screening for lung cancer and only half of current smokers would opt for surgery if a screen-detected cancer was found. When thinking about lung cancer screening with patients, how do we reach them,? Advertising? Self-referral? Teaser rates? How do we engage with their primary care physicians and what is the best venue for care – the risk assessment clinic, smoking cessation clinic, should we mandate smoking cessation? Barriers to being screened include cost, concern about radiation dose, fatalism and fear.
Most lung nodules will be benign, but do patients and physicians understand the results they receive? How can radiologists frame the results to reduce patient anxiety and compliance with future screening and studies? In one qualitative analysis recommendations from patients included providing an estimate of cancer risk, verbal communication, and a recognition that nodules even if benign are of concern to patients. Prof. Ravenel quoted a pulmonologist colleague, Prof. Gerard Silvestri: “ It’s easy to forget that for the one hearing the news, it’s likely to be one of the scariest days of their life.”
Latest Articles
CT, Lung Cancer Screening
With screening for lung cancer likely to be funded in the United States in the near future for patients at high risk for lung cancer, radiologists need to...