Research presented at the Society of Nuclear Medicine and Molecular Imaging's 2019 Annual Meeting draws a strong link between severe obstructive sleep apnea (OSA) and impaired coronary flow reserve, which is an early sign of the heart disease atherosclerosis. Using 13N-ammonia positron emission tomography/computed tomography (PET/CT), researchers were able to noninvasively evaluate coronary microvascular function in OSA patients and use their findings to predict cardiovascular disease risk.
Obstructive sleep apnea occurs when a person's airway is blocked while sleeping, which causes intermittent pauses in breathing. According to the American Sleep Apnea Association, an estimated 22 million Americans suffer from sleep apnea, which is increasingly recognized as a cardiovascular disease risk factor. Left untreated, OSA can lead to high blood pressure, stroke, chronic heart failure and other cardiovascular problems.
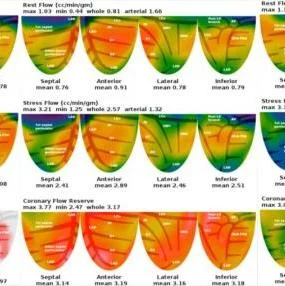
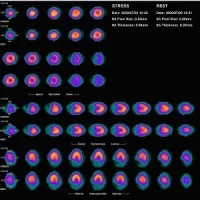
To evaluate the cardiovascular disease risk factors in OSA patients, researchers conducted 13N-ammonia PET/CT imaging on 38 patients, who were divided into three groups based on the severity of their sleep apnea. During the PET/CT imaging, myocardial blood flow and coronary flow reserve--key indicators of coronary dysfunction--were automatically calculated using quantitative PET/CT software.
The mean rest myocardial blood flow was similar among patients in the three groups of mild, moderate and severe OSA. The mean hyperemic myocardial blood flow was also similar, though researchers found that the blood flow decreased gradually as the severity of OSA increased. There were, however, significant differences in the mean coronary flow reserve among the three groups--those with severe OSA had a substantially lower coronary flow reserve.
"As we all know, impaired coronary flow reserve is an early sign of atherosclerosis," said Ruonan Wang, MD, The First Hospital of Shanxi Medical University in Taiyuan, China. "Our study suggests that patients with OSA, especially severe OSA, should receive PET myocardial perfusion imaging as early as possible to exclude coronary microcirculatory dysfunction."
Source: Society of
Nuclear Medicine and Molecular Imaging
Image Credit: Wang R, Wu P, Li L, et al.
Latest Articles
CT, PET, cardiovascular disease, sleep apnoea
Research presented at the Society of Nuclear Medicine and Molecular Imaging's 2019 Annual Meeting draws a strong link between severe obstructive sleep apnea (OSA) and impaired coronary flow reserve, which is an early sign of the heart disease atherosclero