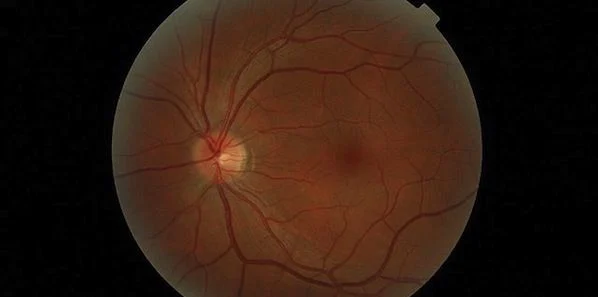
A noninvasive retinal imaging device, created at Cedars-Sinai, has potential for early detection of changes that later occur in the brain and are associated with Alzheimer's disease, according to preliminary results of a clinical trial performed in Australia.
The new optical imaging tool has been shown to detect changes that occur 15-20 years before clinical diagnosis. "It's a practical exam that could allow testing of new therapies at an earlier stage, increasing our chances of altering the course of Alzheimerís disease," explained Shaun Frost, a biomedical scientist and the study manager at the Commonwealth Scientific and Industrial Research Organisation (CSIRO).
Frost explained that, based on preliminary results in 40 patients, the optical exam could differentiate between Alzheimer's disease and non-Alzheimer's disease with 100 percent sensitivity (everyone with the disease tested positive) and 80.6 percent specificity (most people without the disease tested negative.
The researchers presented their findings July 15 at the Alzheimer's Association International Conference (AAIC) 2014 in Denmark.
Frost, first author of the AAIC 2014 abstract, was to make the oral presentation on behalf of his team. He noted that 120 participants of a full study of 200 had completed testing.
Beta-Amyloid Plaque
The accumulation of beta-amyloid plaque in the brain is a strong indicator of Alzheimer's, but available tests detect changes only when the disease is already in advanced stages, said Keith Black, MD, professor and chair of Cedars-Sinai's Department of Neurosurgery and concurrently director of the Maxine Dunitz Neurosurgical Institute and the Ruth and Lawrence Harvey Chair in Neuroscience.
Positron emission tomography (PET) is currently the diagnostic modality of choice. Prof. Black explaind that as PET scans need the use of radioactive tracers, and cerebrospinal fluid analysis means that patients undergo invasive and often painful lumbar punctures, neither approach is quite feasible, especially for patients in the earlier stages of disease.
The retina, as part of the central nervous system, shares many characteristics of the brain. Dr. Black said the plaques associated with Alzheimer's disease occur in the brain and also in the retina. He explained that by 'staining' the plaque with curcumin, which is found in the spice turmeric, the plaque could be detected in the retina before it began to accumulate in the brain. The device developed at Cedars-Sinai enables researchers to look through the eye and see these changes.
This clinical trial allowed researchers to correlate retinal plaque detected by optical imaging with brain plaque detected by PET scans. Participants in this study included patients diagnosed with Alzheimer's, patients with mild cognitive impairment, and a group with no evidence of brain abnormality.
Rodents Used In Previous Studies
Previous research on retinal beta-amyloid plaque and optical imaging technology by Cedars-Sinai included studies with live rodents and the post-mortem examination of human retinas of people who had died with Alzheimer's. Authors of the original results included Maya Koronyo-Hamaoui, PhD, assistant professor of neurosurgery in the Department of Neurosurgery and the Department of Biomedical Sciences and Yosef Koronyo, a research scientist. Their findings were presented at the AAIC in 2010 and published.
The CSIRO-led study is one of several in progress to determine if similar results can be confirmed in humans affected by the disease.
"This large double-blind clinical trial appears to validate our novel human retinal amyloid imaging approach using curcumin labeling. It further demonstrates significant correlation with brain amyloid burden, thereby predicting accumulation of plaques in the brain through the retina," said Koronyo-Hamaoui, a faculty principal investigator and head of the Neuroimmunology and Retinal Imaging Laboratory at Cedars-Sinai.
NeuroVision Imaging LLC, under license by Cedars-Sinai, is working towards enhancement of the retinal imaging technology.
Source: ScienceDaily
Image source: Wikimedia Commons
Latest Articles
Imaging, Alzheimer's, retina
A noninvasive retinal imaging device, created at Cedars-Sinai, has potential for early detection of changes that later occur in the brain and are associate...