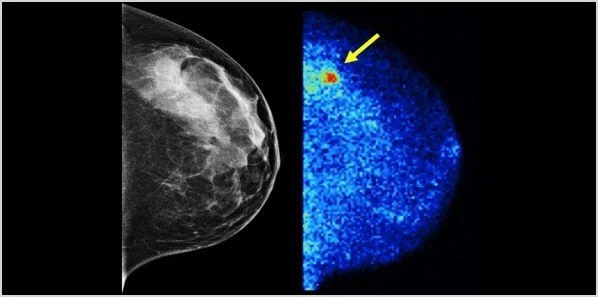
Molecular Breast Imaging (MBI), a new breast imaging technique pioneered at Mayo Clinic, nearly quadruples detection rates of invasive breast cancers in women with dense breast tissue. Results of a major study show that MBI increased the detection rate of invasive breast cancers by more than 360 percent when used in addition to regular screening mammography.
MBI is a supplemental imaging tool designed to find tumours that would otherwise be obscured by surrounding dense breast tissue on a mammogram. It uses small, semiconductor-based gamma cameras to image the breast following injection of a radiotracer that tumours absorb avidly. This imaging technique exploits the different behaviour of tumours relative to background tissue, producing a functional image of the breast that can detect tumours not seen on mammography.
Tumours and dense breast tissue can both appear white on a mammogram, making tumours indistinguishable from background tissue in women with dense breasts. About half of all screening-aged women have dense breast tissue, according to Deborah Rhodes, MD, a Mayo Clinic Breast Clinic physician and the senior author of this study. The results are published in the American Journal of Roentgenology.
In the study, conducted at Mayo Clinic, 1,585 women with heterogeneously or extremely dense breasts underwent an MBI exam at the time of their screening mammogram. Key findings of the study include:
“The finding that MBI substantially increases detection rates of invasive cancers in dense breasts without an unacceptably high increase in false positive findings has important implications for breast cancer screening decisions, particularly as 20 states now require mammography facilities to notify women about breast density and encourage discussion of supplemental screening options,” Dr. Rhodes pointed out.
The results indicate that MBI has a more favourable balance of additional invasive cancers detected versus additional biopsies incurred relative to other supplemental screening options, she said. “Recent studies have reported supplemental cancer detection rates of 1.9 per 1,000 women screened with automated whole breast ultrasound and 1.2 to 2.8 per 1,000 women screened with digital breast tomosynthesis, so our finding of an additional 8.8 cancers per 1,000 women makes MBI a very compelling option for women who elect supplemental screening.”
This latest study is a major milestone for both safety and efficacy of MBI largely because of the high detection rates achieved through low radiation exposure, according to Michael O’Connor, PhD, a Mayo Clinic scientist and inventor of the new imaging device.
“We are very excited about what MBI can offer women with dense breasts,” said Amy Conners, MD, chair of Mayo Clinic’s Breast Imaging Division and a co-author of the study. “While we endorse annual mammography for all women age 40 and over, and the addition of annual MRI for women at high risk, MBI fills an important gap for supplemental screening in women with dense breasts who are not otherwise at high risk.”
Source: Mayo Clinic
Image Credit: Mayo Clinic
MBI is a supplemental imaging tool designed to find tumours that would otherwise be obscured by surrounding dense breast tissue on a mammogram. It uses small, semiconductor-based gamma cameras to image the breast following injection of a radiotracer that tumours absorb avidly. This imaging technique exploits the different behaviour of tumours relative to background tissue, producing a functional image of the breast that can detect tumours not seen on mammography.
Tumours and dense breast tissue can both appear white on a mammogram, making tumours indistinguishable from background tissue in women with dense breasts. About half of all screening-aged women have dense breast tissue, according to Deborah Rhodes, MD, a Mayo Clinic Breast Clinic physician and the senior author of this study. The results are published in the American Journal of Roentgenology.
In the study, conducted at Mayo Clinic, 1,585 women with heterogeneously or extremely dense breasts underwent an MBI exam at the time of their screening mammogram. Key findings of the study include:
- Of the 1,585 women, 21 were diagnosed with cancer — five through mammography alone (24 percent or 3.2 cancers per 1,000 women) and 19 with mammography plus MBI (91 percent or 12 cancers per 1,000 women).
- Particularly notable was the fourfold increase in detection of invasive cancers (1.9 invasive cancers per 1,000 women with mammography and 8.8 per 1,000 women with mammography plus MBI). Detection rates for noninvasive cancers were not significantly different.
- The risk of incurring an unnecessary biopsy due to a false positive exam rose in this study, from 1 in 100 women with mammography to 4 in 100 women with mammography plus MBI. (In contrast, recent studies have shown that alternative supplemental screening techniques, such as ultrasound and MRI, generate about eight additional unnecessary biopsies per 100 women.)
“The finding that MBI substantially increases detection rates of invasive cancers in dense breasts without an unacceptably high increase in false positive findings has important implications for breast cancer screening decisions, particularly as 20 states now require mammography facilities to notify women about breast density and encourage discussion of supplemental screening options,” Dr. Rhodes pointed out.
The results indicate that MBI has a more favourable balance of additional invasive cancers detected versus additional biopsies incurred relative to other supplemental screening options, she said. “Recent studies have reported supplemental cancer detection rates of 1.9 per 1,000 women screened with automated whole breast ultrasound and 1.2 to 2.8 per 1,000 women screened with digital breast tomosynthesis, so our finding of an additional 8.8 cancers per 1,000 women makes MBI a very compelling option for women who elect supplemental screening.”
This latest study is a major milestone for both safety and efficacy of MBI largely because of the high detection rates achieved through low radiation exposure, according to Michael O’Connor, PhD, a Mayo Clinic scientist and inventor of the new imaging device.
“We are very excited about what MBI can offer women with dense breasts,” said Amy Conners, MD, chair of Mayo Clinic’s Breast Imaging Division and a co-author of the study. “While we endorse annual mammography for all women age 40 and over, and the addition of annual MRI for women at high risk, MBI fills an important gap for supplemental screening in women with dense breasts who are not otherwise at high risk.”
Source: Mayo Clinic
Image Credit: Mayo Clinic
Latest Articles
Tomosynthesis, Mammography, Tumours, MBI, dense breasts, molecular breast imaging
Molecular Breast Imaging (MBI), a new breast imaging technique pioneered at Mayo Clinic, nearly quadruples detection rates of invasive breast cancers in wo...