IMRIS Inc. has announced that at Yale-New Haven Hospital, New Haven, CT, neurosurgeons are confirming effective chemotherapy delivery in treating eye cancer using intraoperative imaging within the VISIUS® Surgical Theatre.
Selective intra-arterial chemotherapy is used to treat retinoblastomas. The technique allows for delivery of an increased concentration of the drug directly to the tumour and reduces the need to use systemically delivered chemotherapy which can cause significant side effects.
Using the VISIUS Surgical Theatre with iMRI during the treatment procedure is a novel approach to this strategy that permits Yale neurosurgeons to confirm successful delivery of chemotherapy at the tumour site. "Combining the intraoperative MRI with biplane angiography has allowed us to rapidly acquire an intraoperative MRI and indirectly confirm that the chemotherapy reached the site of interest," said Dr. Ketan R. Bulsara, Associate Professor of Neurosurgery and Director of Neuroendovascular and Skull-Base Surgery at Yale School of Medicine.
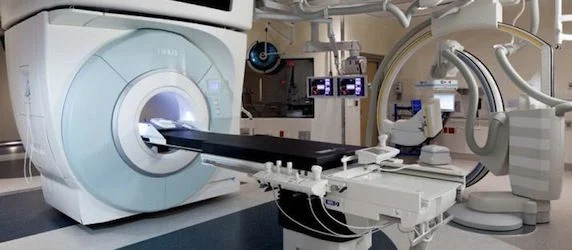
The VISIUS Surgical Theatre at Yale-New Haven Hospital features a high-field iMRI that moves between three rooms for diagnostic and surgical usage. Installed in 2010, the multi-disciplinary suite also has biplane angiography in the third room to add a true intraoperative imaging advantage to neurosurgical, endovascular and microsurgical operating capabilities. The VISIUS iMRI does not require the patient to be moved from the OR table to other rooms for scanning because the MR moves on ceiling rails.
For the retinoblastoma cases, the Yale-New Haven setup allows Dr. Bulsara to use angiography to guide the drug delivery catheter from the entry point at the femoral artery to the ophthalmic artery. The surgeon can then confirm that the chemotherapy reached the site of interest using iMRI.
During the procedures, iMRI scans were obtained within 15 minutes after drug delivery. "The iMRI provided enhanced visualisation of the tumor and the space around the eye using gadolinium as an indirect marker," said Dr. Bulsara.
In the first case, after each of three treatments - spaced four to six weeks apart - imaging showed significant tumor reduction in the child's eye until it was all gone with no major systemic side effects observed. "So far there hasn't been a need to adjust the delivery method because we haven't seen evidence of the therapy going elsewhere," Bulsara said.
Dr. Bulsara, one of only a select few neurosurgeons in the country that is dual fellowship trained in skull based cerebrovascular microsurgery and endovascular neurosurgery, believes that physicians are only beginning to see the potential advantages of having all these capabilities in a single room.
Latest Articles
MRI, Surgery
IMRIS Inc. has announced that at Yale-New Haven Hospital, New Haven, CT, neurosurgeons are confirming effective chemotherapy delivery in treating eye cance...