MRI shows brain damage in a high percentage of active duty U.S. military personnel who suffered blast-related mild traumatic brain injury (MTBI), or concussion, according to a study published in the journal Radiology. Researchers used MRI to study 834 military service members with MTBI related to blast injuries. MRI scans revealed the presence of white matter T2 hyperintensities, which can be thought of as brain scars, in 52 percent of the MTBI patients.
“We were really surprised to see so much damage to the brain in the MTBI patients,” said Gerard Riedy, MD, PhD, from the National Intrepid Center of Excellence (NICoE) at the Walter Reed National Military Medical Center in Bethesda, Md. “It’s expected that people with MTBI should have normal MRI results, yet more than 50 percent had these abnormalities.”
Slightly more than 84 percent of the MTBI patients reported one or more blast-related incidents, and 63 percent reported loss of consciousness at the time of injury.
MTBI is very common amongst U.S. service members returning from conflicts in Iraq and Afghanistan. Current assessment of MTBI relies heavily on behavioural observations and on patient recall of events, such as post-traumatic amnesia and loss of consciousness. The need for a more definitive marker motivated Dr. Riedy and his colleagues to look at advanced brain imaging with MRI as a tool for assessing MTBI.
See Also: Study Pinpoints PTSD and Trauma Injury Differences
The findings represent the first in a series of new studies from the NICoE on advanced brain imaging in MTBI patients, according to Dr. Riedy. “We have several more papers coming up that build on these findings and look at brain function, brain wiring, connectivity and perfusion, or brain blood flow.”
As the research team builds a database of advanced imaging data, they hope to begin to link the data with the more subjective symptoms associated with MTBI.
“A scar on a brain scan is an objective finding,” Dr. Riedy explained. “We start with the objective and build a foundation for the correct diagnosis of MTBI and then bring in the subjective measures later.”
He notes that an objective measure of traumatic brain injury can lead to proper therapies. One key area of focus is the diagnosis of post-traumatic stress disorder (PTSD), a mental health condition caused by a traumatic event or events. PTSD is challenging to diagnose. Symptoms of TBI and PTSD overlap, and treatments for one are unlikely to work for the other.
The ability to see the brain scans has already had an impact on military personnel and their families, Dr. Riedy said, allowing them to see for the first time what has previously been called the invisible wounds of war.
“Military traumatic brain injury is not a small problem for our country,” he said. “Through this research, we hope to learn more about what the future entails for our military personnel who’ve suffered these injuries.”
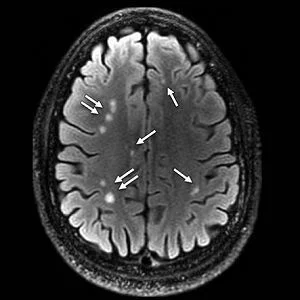
Top Image. Axial T2 FLAIR image shows multiple white matter T2-weighted hyperintense areas (arrows) in a 28-year-old man with blast-related mild TBI. This patient had a total of 76 lesions on all sections.
Source and image credit: Radiological Society of North America
“We were really surprised to see so much damage to the brain in the MTBI patients,” said Gerard Riedy, MD, PhD, from the National Intrepid Center of Excellence (NICoE) at the Walter Reed National Military Medical Center in Bethesda, Md. “It’s expected that people with MTBI should have normal MRI results, yet more than 50 percent had these abnormalities.”
Slightly more than 84 percent of the MTBI patients reported one or more blast-related incidents, and 63 percent reported loss of consciousness at the time of injury.
MTBI is very common amongst U.S. service members returning from conflicts in Iraq and Afghanistan. Current assessment of MTBI relies heavily on behavioural observations and on patient recall of events, such as post-traumatic amnesia and loss of consciousness. The need for a more definitive marker motivated Dr. Riedy and his colleagues to look at advanced brain imaging with MRI as a tool for assessing MTBI.
See Also: Study Pinpoints PTSD and Trauma Injury Differences
The findings represent the first in a series of new studies from the NICoE on advanced brain imaging in MTBI patients, according to Dr. Riedy. “We have several more papers coming up that build on these findings and look at brain function, brain wiring, connectivity and perfusion, or brain blood flow.”
As the research team builds a database of advanced imaging data, they hope to begin to link the data with the more subjective symptoms associated with MTBI.
“A scar on a brain scan is an objective finding,” Dr. Riedy explained. “We start with the objective and build a foundation for the correct diagnosis of MTBI and then bring in the subjective measures later.”
He notes that an objective measure of traumatic brain injury can lead to proper therapies. One key area of focus is the diagnosis of post-traumatic stress disorder (PTSD), a mental health condition caused by a traumatic event or events. PTSD is challenging to diagnose. Symptoms of TBI and PTSD overlap, and treatments for one are unlikely to work for the other.
The ability to see the brain scans has already had an impact on military personnel and their families, Dr. Riedy said, allowing them to see for the first time what has previously been called the invisible wounds of war.
“Military traumatic brain injury is not a small problem for our country,” he said. “Through this research, we hope to learn more about what the future entails for our military personnel who’ve suffered these injuries.”
Top Image. Axial T2 FLAIR image shows multiple white matter T2-weighted hyperintense areas (arrows) in a 28-year-old man with blast-related mild TBI. This patient had a total of 76 lesions on all sections.
Source and image credit: Radiological Society of North America
Latest Articles
healthmanagement, MRI, brain imaging, concussion, brain injury, MTBI, trauma
MRI shows brain damage in a high percentage of active duty U.S. military personnel who suffered blast-related mild traumatic brain injury (MTBI), or concussion, according to new a study published in the journal Radiology.