While the radiology workload is increasing, radiologists are expected to just do more, said Prof. Erika Denton (pictured), National Clinical Director for Diagnostics, National Health Service (NHS) England, speaking at the Management in Radiology (MIR) Annual Scientific Meeting in Bologna, 2-3 October 2014. Change is needed, and data about services is essential to effect change and monitor results.
 Prof. Denton is responsible for the national strategy for radiology in England, and ensuring that radiological services across England are delivered fairly and equally. Showing recent data on the increase in radiology examinations, Denton observed that strategic thinking is needed to managing the overwhelming sense that radiologists are being overworked. It is important to count what radiologists do, and count the impact of what radiologists do, beyond the “technological silo” that radiology can tend to focus on.
Prof. Denton is responsible for the national strategy for radiology in England, and ensuring that radiological services across England are delivered fairly and equally. Showing recent data on the increase in radiology examinations, Denton observed that strategic thinking is needed to managing the overwhelming sense that radiologists are being overworked. It is important to count what radiologists do, and count the impact of what radiologists do, beyond the “technological silo” that radiology can tend to focus on.
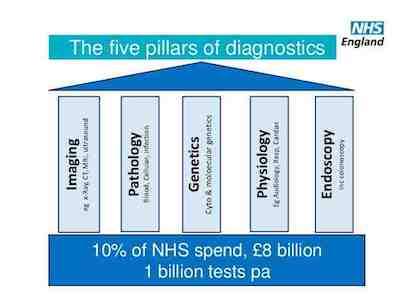
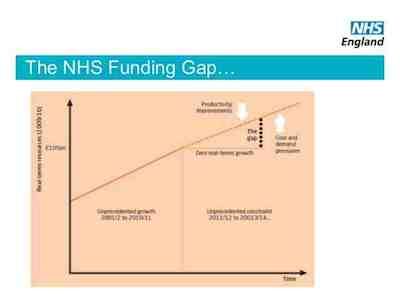
Radiology represents around 7% of the NHS budget. However, the NHS faces a funding gap, which is a 5% year on year reduction in reality. As with other European countries, in England the vast majority of the increase in population over the next 6 years is predicted to be in the 60+ age bracket. 80 percent of deaths in the over 60s are due to just three underlying causes: cancer, circulatory diseases and respiratory diseases. The issue is thus how to deliver appropriate imaging to these populations. Demographics plus patient/ public expectation and assuring quality while delivering value for money make for a complicated equation.
The solution? A transformational change to the current way of delivering health care. Previously radiology has effected transactional change, pedalling systems harder and faster. However, said Denton, quoting Einstein, “You can’t solve a problem by using same thinking that created it.”
Denton explained that collecting data can help to deliver change.The NHS England Diagnostic Imaging Dataset collects data monthly directly from Radiological Information Systems (RIS), and includes for every imaging event, who requested it, demographics, code of the test, report turnaround and waiting times. NHS England performs nearly 1 million imaging exams per month, which is almost double the activity of 10 years ago. However, the workforce hasn’t increased to the same degree. The NHS is exploring linking this data to outcome via the Hospital Episode Statistics and Cancer registries. The aim is to establish “optimum” intervention rates.
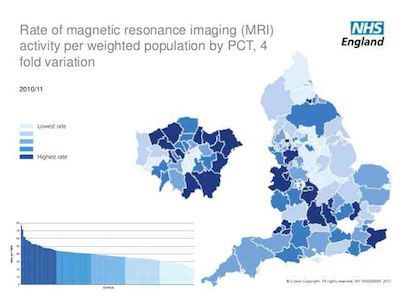
The NHS Atlas of Variation looks at the rate of healthcare interventions undertaken per population. For MRI examinations, there is a four-fold difference between geographic areas. There is a 20-fold variability in ultrasound usage. Now what is needed is the evidence of why there is such variation.
Funding for imaging relies on accurate coding. Unlike other European countries, in England there are not separate tariffs for inpatient imaging. There are tariffs for directly accessed and outpatient imaging. These are ‘bundled’ in patient tariffs. There are also block contracts for some plain film and ultrasound. Some best practice tariffs are used to encourage change. For example, to encourage a shift from performing hysterectomy towards embolisation, there is more money for new procedures than for traditional open procedures. Procedures with best practice tariffs include endovascular arterial repair for aortic aneurysm, thoracic endovascular aneurysm repair (EVAR), uterine artery embolisation for fibroids, angioplasty and stenting for vasular disease with a tariff uplift for diabetics, transjugular intrahepatic portosystemic shunts and vacuum-assisted breast lump excision. There are proposals for CT colongraphy.
Service improvement uses benchmarking, and an inhouse NHS benchmarking service has over 320 member organisations. The data collected includes radiology, and benchmarking data is available on radiology rooms, scanners/ machines by modality, activity, workforce and more. For example, an average of 62% of exams are reported with voice recognition, which is an important tool for improving efficiency.
These data are and mapped against in- and outpatient attendances.
Cost reduction in radiological services is enabled by PACS, speech recognition dictation and skill mix, so that radiologists only do what only they can do. Other tools will look at efficiency, for example lean 6-sigma etc. Seven day and 24/7 working, teleradiology and demand management will also play a role.
The reasons for change are compelling, said Denton. The health service needs to lower costs and make best use of resources, deal with increasing demand vs capacity, lower the length of patient pathways and waiting times, and not least, change because patients want it. Worse outcomes for patients admitted and discharged at weekends are not acceptable. Whole system change is essential, said Denton, and needs to involve primary and secondary care, social services, transport for patients and staff, childcare.
The NHS has issued Clinical Standards for 7 day services, including a standard for diagnostics, that inpatients must have scheduled 7 day access to diagnostic services such as x-ray, US, CT, MRI, echocardiography, endoscopy, bronchoscopy and pathology. Consultant-directed diagnostic tests and completed reporting will be available 7 days a week. Standard 6 states that interventional radiology is required as a 7 day service alongside critical care, interventional endoscopy and emergency general surgery. Working towards a new model for radiology, Denton said that tertiary services will remain a 5 day service, but for everything else 24/7 services will become standard. For that to happen, the NHS needs good teleradiology, telepathology and information sharing.
Claire Pillar
Managing Editor, HealthManagement
 Prof. Denton is responsible for the national strategy for radiology in England, and ensuring that radiological services across England are delivered fairly and equally. Showing recent data on the increase in radiology examinations, Denton observed that strategic thinking is needed to managing the overwhelming sense that radiologists are being overworked. It is important to count what radiologists do, and count the impact of what radiologists do, beyond the “technological silo” that radiology can tend to focus on.
Prof. Denton is responsible for the national strategy for radiology in England, and ensuring that radiological services across England are delivered fairly and equally. Showing recent data on the increase in radiology examinations, Denton observed that strategic thinking is needed to managing the overwhelming sense that radiologists are being overworked. It is important to count what radiologists do, and count the impact of what radiologists do, beyond the “technological silo” that radiology can tend to focus on. 

Radiology represents around 7% of the NHS budget. However, the NHS faces a funding gap, which is a 5% year on year reduction in reality. As with other European countries, in England the vast majority of the increase in population over the next 6 years is predicted to be in the 60+ age bracket. 80 percent of deaths in the over 60s are due to just three underlying causes: cancer, circulatory diseases and respiratory diseases. The issue is thus how to deliver appropriate imaging to these populations. Demographics plus patient/ public expectation and assuring quality while delivering value for money make for a complicated equation.
The solution? A transformational change to the current way of delivering health care. Previously radiology has effected transactional change, pedalling systems harder and faster. However, said Denton, quoting Einstein, “You can’t solve a problem by using same thinking that created it.”
Denton explained that collecting data can help to deliver change.The NHS England Diagnostic Imaging Dataset collects data monthly directly from Radiological Information Systems (RIS), and includes for every imaging event, who requested it, demographics, code of the test, report turnaround and waiting times. NHS England performs nearly 1 million imaging exams per month, which is almost double the activity of 10 years ago. However, the workforce hasn’t increased to the same degree. The NHS is exploring linking this data to outcome via the Hospital Episode Statistics and Cancer registries. The aim is to establish “optimum” intervention rates.
The NHS Atlas of Variation looks at the rate of healthcare interventions undertaken per population. For MRI examinations, there is a four-fold difference between geographic areas. There is a 20-fold variability in ultrasound usage. Now what is needed is the evidence of why there is such variation.

Funding for imaging relies on accurate coding. Unlike other European countries, in England there are not separate tariffs for inpatient imaging. There are tariffs for directly accessed and outpatient imaging. These are ‘bundled’ in patient tariffs. There are also block contracts for some plain film and ultrasound. Some best practice tariffs are used to encourage change. For example, to encourage a shift from performing hysterectomy towards embolisation, there is more money for new procedures than for traditional open procedures. Procedures with best practice tariffs include endovascular arterial repair for aortic aneurysm, thoracic endovascular aneurysm repair (EVAR), uterine artery embolisation for fibroids, angioplasty and stenting for vasular disease with a tariff uplift for diabetics, transjugular intrahepatic portosystemic shunts and vacuum-assisted breast lump excision. There are proposals for CT colongraphy.
Service improvement uses benchmarking, and an inhouse NHS benchmarking service has over 320 member organisations. The data collected includes radiology, and benchmarking data is available on radiology rooms, scanners/ machines by modality, activity, workforce and more. For example, an average of 62% of exams are reported with voice recognition, which is an important tool for improving efficiency.
These data are and mapped against in- and outpatient attendances.
Cost reduction in radiological services is enabled by PACS, speech recognition dictation and skill mix, so that radiologists only do what only they can do. Other tools will look at efficiency, for example lean 6-sigma etc. Seven day and 24/7 working, teleradiology and demand management will also play a role.
The reasons for change are compelling, said Denton. The health service needs to lower costs and make best use of resources, deal with increasing demand vs capacity, lower the length of patient pathways and waiting times, and not least, change because patients want it. Worse outcomes for patients admitted and discharged at weekends are not acceptable. Whole system change is essential, said Denton, and needs to involve primary and secondary care, social services, transport for patients and staff, childcare.
The NHS has issued Clinical Standards for 7 day services, including a standard for diagnostics, that inpatients must have scheduled 7 day access to diagnostic services such as x-ray, US, CT, MRI, echocardiography, endoscopy, bronchoscopy and pathology. Consultant-directed diagnostic tests and completed reporting will be available 7 days a week. Standard 6 states that interventional radiology is required as a 7 day service alongside critical care, interventional endoscopy and emergency general surgery. Working towards a new model for radiology, Denton said that tertiary services will remain a 5 day service, but for everything else 24/7 services will become standard. For that to happen, the NHS needs good teleradiology, telepathology and information sharing.
Claire Pillar
Managing Editor, HealthManagement
Latest Articles
Radiology, MIR 2014, England, Metrics
While the radiology workload is increasing, radiologists are expected to just do more, said Prof. Erika Denton (pictured), National Clinical Director for D...










