Medical decision-making about antibiotic use in critically ill patients is challenging and complex. The need for antibiotic stewardship requires judicious prescription and choice of antimicrobials, as the need for effective therapy has to be put in balance with the need to limit undue selection pressure, and all this must be done in a context of diagnostic and prognostic uncertainty. This decision-making is not a single or static decision, but should rather be seen as an evolving series of successive decisions and choices that have to be made when the clinical case gradually unfurls its course while more diagnostic results progressively become available. As a means to clarify this decision process and stimulate the application of antibiotic stewardship in its different stages, it may be helpful to use a metaphor.
You might also like: Antimicrobial stewardship in the ICU
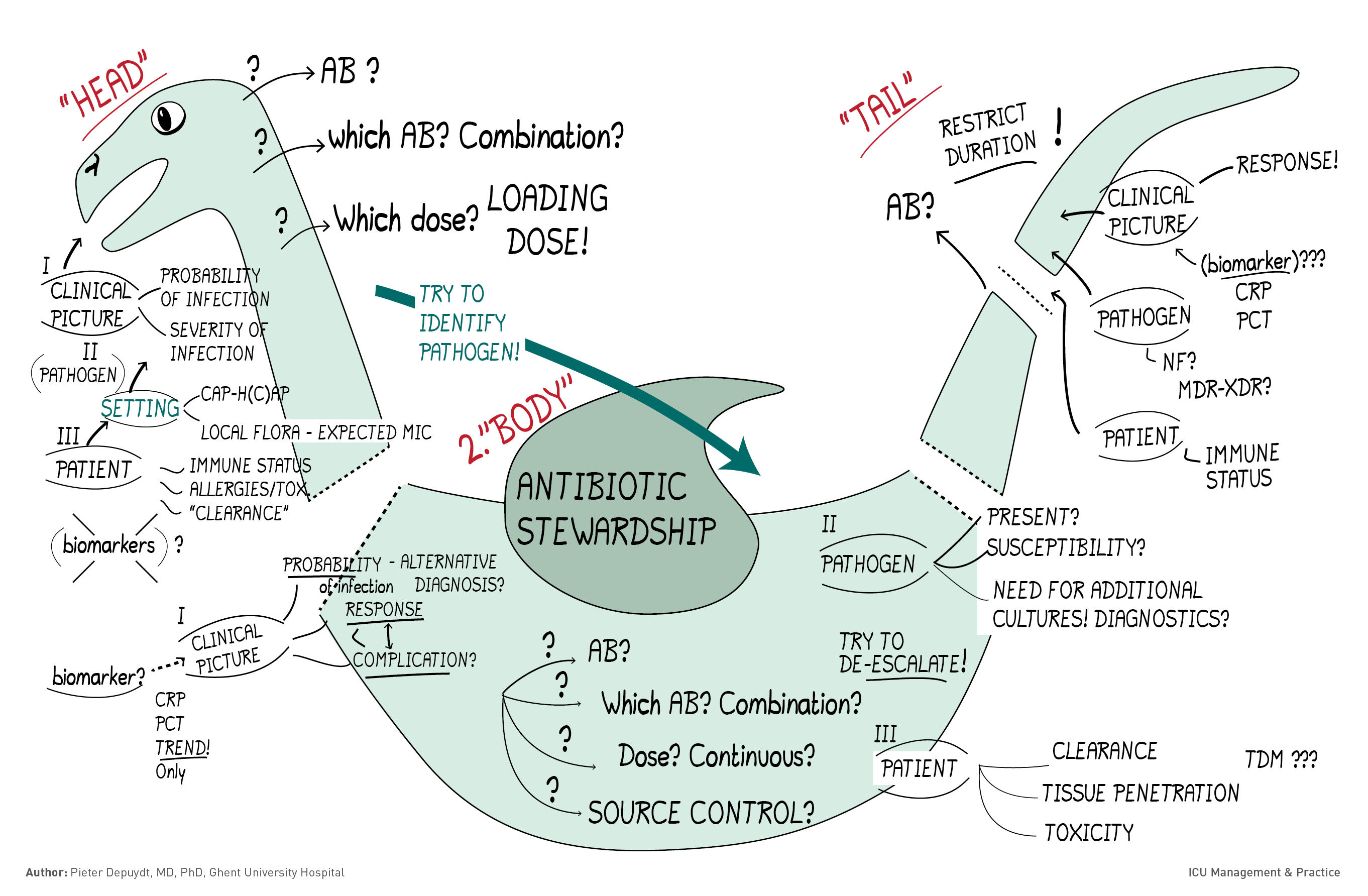
‘Head’: clinical suspicion of infection
Let us consider the clinical problem of suspected infection in your ICU patient as a ‘monster’ (a dragon, griffion or alvarezsaurid dinosaur if you like) that comes to you with a ‘head’, a ‘body’ and a ‘tail’. The ‘head’ stares at you when the first clinical suspicion of infection is raised, when you must decide whether or not to initiate antibiotics and which empirical choices to make. You should weigh clinical, radiological and biochemical elements to judge the likelihood and severity of infection. Whether broad-spectrum (and maybe a combination of) antibiotics are required is determined by severity of infection, risk factors for antibiotic drug resistance and local epidemiology. When you decide to start antibiotics, ascertain that these are given as soon as possible and in a sufficient dose. Obtaining appropriate samples for microbiology first (while not unduly delaying antibiotic therapy) will bring you much needed information in later stages of decision-making.
‘Body’ of the clinical problem
After this initial empirical phase, you enter the ‘body’ of the clinical problem, when more diagnostic results come in (including microbiology results) and when you already may observe a clinical response (or lack thereof) to the initiated antibiotics. Now you must reconsider the need for and choice of antibiotics in the light of this new information. At this point, you may decide to stop empirical antibiotics when infection is at second sight unlikely, or you can change them to therapy which more selectively targets the pathogen that has been identified as the likely cause of infection. This is the time when you should try de-escalation. Closely observing clinical response will help you to timely detect toxicity or failure of your antibiotics. You can consider changing or escalating antibiotics, but importantly, think if you would not want some more diagnostics (new cultures, imaging), or whether a more aggressive source control should be attempted.
‘Tail’ - clinical problem resolves
When the clinical problem resolves, you come to its ‘tail’, where you have another opportunity to limit or stop the selection pressure caused by the antibiotics. Biomarkers may be helpful to support your decision to stop antibiotics, but your careful clinical examination and appreciation of pathogen and host characteristics may be just as trustworthy. At this stage, your decision to stop antibiotics may be backed up by numerous papers that show that
shorter courses of antibiotics are generally safe.







