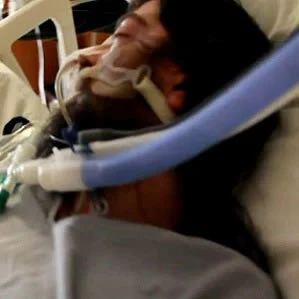
Ventilator-associated pneumonia (VAP) is the most frequent life-threatening nosocomial infection in intensive care units. Although bundles of prevention measures are effective in decreasing the VAP rate, the insufficient compliance observed in clinical practice needs to be addressed in order to define easier-to-apply procedures, according to a review paper published by F1000 Research.
VAP develops in ICU patients mechanically ventilated for at least 48 hours. Most studies showed that VAP is usually due to aerobic Enterobacteriaceae (25%), Staphylococcus aureus (20%), Pseudomonas aeruginosa (20%), Haemophilus influenza (10%), and streptococci. Multidrug-resistant (MDR) pathogens are more common among late-onset cases.
Two groups of risk factors for VAP have been identified — namely ventilation-related factors (instrumentation of the airway with an endotracheal tube and subsequent microaspirations) and, less frequently, patient-related factors (for example, pre-existing pulmonary disease) —and only the former is accessible to prevention. As a result, VAP, unlike many other nosocomial infections, is difficult to prevent.
"First of all, reducing the exposure to risk factors for VAP is the most efficient way to prevent VAP onset. Therefore, intubation should be avoided whenever possible, and strategies such as non-invasive positive-pressure ventilation, sedation, and weaning protocols should be used to replace or shorten mechanical ventilation. In contrast, recent data suggest that the timing of the tracheotomy does not significantly change VAP incidence," the article explains.
While studies demonstrated great success in reducing VAP rates using bundle of care in recent years, meta-analyses showed that most of the preventive measures failed to demonstrate a sustained effect. This conclusion is in line with the absence of substantial improvement of VAP rates in the past decade.
"Beyond the theoretical frame, a great deal of attention must be given to the factors that might facilitate a bundle implementation and allow a sustained compliance. An educational session alone, without an associated behavioural strategy, is unlikely to induce profound behavioural changes," notes the article. "It should be kept in mind that, to engage an individual in a particular behaviour and improve compliance, we need to act on predisposing factors (knowledge, perceptions, and beliefs) to favour the access to new processes or technologies and to continually reinforce the behaviour by feedback."
In case of VAP suspicion, respiratory secretions must be collected for bacteriological secretions before any new antimicrobials. Recent U.S. guidelines recommend noninvasive sampling with semi-quantitative culture, whereas the European guidelines suggest obtaining distal samples with quantitative cultures to improve the accuracy of results. Despite this discrepancy, the two guidelines agreed that a bacteriological sample should be performed before any antibiotic treatment in order to reduce antibiotic exposure.
The article says quantitative distal bacteriological exams may be preferable for a more reliable diagnosis and therefore a more appropriate use of antimicrobials. "To improve the prognosis, the treatment should be adequate as soon as possible but should avoid unnecessary broad-spectrum antimicrobials to limit antibiotic selection pressure," the authors point out. For empiric treatments, the selection of antimicrobials should consider the local prevalence of micro-organisms along with their associated susceptibility profiles.
Beta-lactams remain a cornerstone antibiotic for the treatment of VAP. Critically ill patients require high dosages of antimicrobials and more specifically continuous or prolonged infusions for beta-lactams. "For β-lactams, the best results seem to be associated with β-lactam plasma levels up to four times the minimal inhibitory concentration (MIC) of the involved pathogen and during 100% of the interval between each dose. For these agents, a loading dose followed by a continuous infusion may be a relevant method of administration to increase the antibiotic concentration in the blood and the lung lining fluid with a lower risk of neurological or renal toxicity," the authors explain. After patient stabilisation, antimicrobials should be maintained for 7–8 days.
The article also notes that the evaluation of VAP treatment based on 28-day mortality is being challenged by regulatory agencies, which are working on alternative surrogate endpoints and on trial design optimisation.
Source: F1000 Research
Image Credit: Aaron Cohen
References:
Timsit, Jean-Francois et al. (2017) Update on ventilator-associated pneumonia. F1000Research.
Latest Articles
nosocomial infection, intensive care units, ventilator-associated pneumonia
Ventilator-associated pneumonia (VAP) is the most frequent life-threatening nosocomial infection in intensive care units. Although bundles of prevention measures are effective in decreasing the VAP rate, the insufficient compliance observed in clinical pr