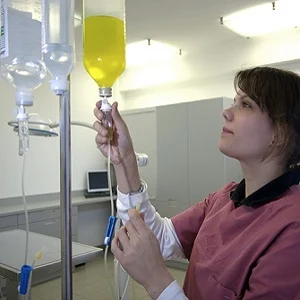
Many patients in the ICU receive multiple IV infusions. This can lead to significant confusion because infusions look quite similar, and a patient with multiple infusions tends to be surrounded by associated components such as bags, tubing, pumps, etc. There is often a lack of information along the infusion pathway, which can lead to confusion. For example, if an infusion change is required, the healthcare provider must reconcile the bag that is associated with the tubing, pump, and access port. It is at this point that there could be an error. Delays could occur, and in serious cases, patients can be harmed.
Kane-Gill et al. have shown that the higher the number of drugs being infused IV, the greater is the likelihood of having an adverse drug event. Also, a review by the Pennsylvania Patient Safety Authority reports that infusion mix-up errors were the most common error and 92% of these errors were related to high-alert drugs such as heparin and insulin. The ECRI Institute has also rated infusion mix-ups as one of the top 10 health technology hazards, and the FDA has issued an urgent call to action to improve the management of multiple infusions.
There are very limited strategies in place to reduce infusion mix-up, and infusion setups vary between different hospitals, clinicians, and units. Several interventions have been proposed but have not been empirically evaluated.
In this review, the authors evaluate the impact of three interventions on the accuracy and speed of infusion identification and disconnection:
Use of Line Label/Organisers
This strategy has been recommended to improve the transfer of information along the infusion pathway and to reduce the physical complexity of the different components. This particular intervention has three components: the use of pre-printed wrap-around labels on each infusion; tubing organisers/guides; and a rake pole-top to align the bags to the corresponding pump.
Smart Pump
The use of a pump with dose error reduction software that would check programmed variables using infusion identifiers (such as drug name, dose) which will be displayed on each pump's channel.
Light-Linking System
This involves illuminating the infusion pathway to automate line racing. By pushing a button on the bag, a wireless signal is sent to the receivers on the corresponding pump and distal end of the tubing which would result in a green light to flash for 7 seconds.
The study findings suggest that labels/organisers can decrease infusion identification time and errors. Clearly, there is a need to use labels/organisers in patients receiving multiple infusions, which is currently not a standard practice.
Source: Critical Care Medicine
Image Credit: iStock
References:
Sonia JP et al. (2019) Untangling Infusion Confusion. A Comparative Evaluation of Interventions in a Simulated Intensive Care Setting. Critical Care Medicine, 47(7):e597-e601.
Latest Articles
ICU, infusion pumps, infusion, tubing, infusion mix-up
In this review, the authors evaluate the impact of three interventions on the accuracy and speed of infusion identification and disconnection: