Among adults with suspected infection admitted to an ICU, an increase in Sequential [Sepsis-related] Organ Failure Assessment (SOFA) score of 2 or more had greater prognostic accuracy for in-hospital mortality than the quick SOFA (qSOFA) score or the systemic inflammatory response syndrome (SIRS) criteria. The findings, published in JAMA, suggest that SIRS criteria and qSOFA may have limited use for predicting mortality in an ICU setting.
See Also: Sepsis-3 - Towards Earlier Recognition and Management
Sepsis remains difficult to define but represents a significant burden of disease. Survival following sepsis is associated with long-term physical, cognitive, and psychosocial morbidity, and an increased mortality rate up to two years after an event.
Accurate diagnostic criteria and consensus definitions have an important role in adult intensive care medicine, providing tools for research, benchmarking, performance monitoring, and accreditation. The Sepsis-3 Criteria emphasised the value of a change of 2 or more points in the SOFA score, introduced qSOFA, and removed the SIRS criteria from the sepsis definition.
Researchers performed a retrospective cohort analysis of 184,875 patients with an infection-related primary admission diagnosis in 182 Australian and New Zealand intensive care units (ICUs) from 2000 through 2015. The aim was to assess the discriminatory capacities of an increase in SOFA score by 2 or more points, 2 or more SIRS criteria, or a qSOFA score of 2 or more points for outcomes among patients who are critically ill with suspected infection. For this study, the primary outcome was in-hospital mortality. In-hospital mortality or ICU length of stay (LOS) of three days or more was a composite secondary outcome.
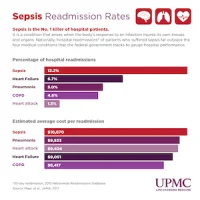
Mean age of patients was 62.9 years, with women comprising 44.6 percent of the study population. The most common diagnosis was bacterial pneumonia: 32,634 patients (17.7 percent). The investigators reported these key findings:
According to the researchers, SOFA demonstrated significantly greater discrimination for in-hospital mortality than SIRS criteria or qSOFA. SOFA also outperformed the other scores for the secondary end point. The findings were consistent for both outcomes in multiple sensitivity analyses, the researchers noted.
"Using a large binational database independent of the sepsis consensus development cohorts, this study confirmed that an increase in SOFA score of 2 or more points within the first 24 hours of ICU admission had superior prognostic accuracy for mortality or ICU length of stay of three days or more compared with SIRS criteria or qSOFA," the authors write. "It established that the use of an increase in SOFA score of 2 or more points to define sepsis was an appropriate data-based starting point, and would likely have broad external validity in ICU patients from developed countries."
In an email to ICU Management & Practice, Andrew Udy, Eamon Raith and David Pilcher, from the research group, commented: “Perhaps most surprising was how consistent and similar our findings were to those of the Sepsis-3 taskforce who promoted the new Sepsis definitions in JAMA in early 2016, even though they had only originally examined a much smaller number of Intensive Care admissions. Our findings were encouraging in that they provided external validity to support the new Sepsis-3 definitions, at least in modern ICUs in higher-income countries.”
Udy added: “For the clinician at the bedside, it emphasises the significance of organ dysfunction with infection in predicting a higher mortality risk for an individual patient…the concept underpinning the new definition of sepsis. This will potentially allow for better planning of treatment strategies and more informed discussions with patients and families. For the researcher and epidemiologist, we now have a consistent and well-validated method to diagnose sepsis which appears generalisable across different health care systems and which may assist development of clinical trials and interpretation of variation in outcomes.”
See Also: Sepsis-3 - Towards Earlier Recognition and Management
Sepsis remains difficult to define but represents a significant burden of disease. Survival following sepsis is associated with long-term physical, cognitive, and psychosocial morbidity, and an increased mortality rate up to two years after an event.
Accurate diagnostic criteria and consensus definitions have an important role in adult intensive care medicine, providing tools for research, benchmarking, performance monitoring, and accreditation. The Sepsis-3 Criteria emphasised the value of a change of 2 or more points in the SOFA score, introduced qSOFA, and removed the SIRS criteria from the sepsis definition.
Researchers performed a retrospective cohort analysis of 184,875 patients with an infection-related primary admission diagnosis in 182 Australian and New Zealand intensive care units (ICUs) from 2000 through 2015. The aim was to assess the discriminatory capacities of an increase in SOFA score by 2 or more points, 2 or more SIRS criteria, or a qSOFA score of 2 or more points for outcomes among patients who are critically ill with suspected infection. For this study, the primary outcome was in-hospital mortality. In-hospital mortality or ICU length of stay (LOS) of three days or more was a composite secondary outcome.
Mean age of patients was 62.9 years, with women comprising 44.6 percent of the study population. The most common diagnosis was bacterial pneumonia: 32,634 patients (17.7 percent). The investigators reported these key findings:
- Of the 184,875 patients, a total of 34,578 patients (18.7 percent) died in the hospital, and 102,976 patients (55.7 percent) died or experienced an ICU LOS of three days or more.
- SOFA score increased by 2 or more points in 90.1 percent; 86.7 percent manifested 2 or more SIRS criteria, and 54.4 percent had a qSOFA score of 2 or more points.
According to the researchers, SOFA demonstrated significantly greater discrimination for in-hospital mortality than SIRS criteria or qSOFA. SOFA also outperformed the other scores for the secondary end point. The findings were consistent for both outcomes in multiple sensitivity analyses, the researchers noted.
"Using a large binational database independent of the sepsis consensus development cohorts, this study confirmed that an increase in SOFA score of 2 or more points within the first 24 hours of ICU admission had superior prognostic accuracy for mortality or ICU length of stay of three days or more compared with SIRS criteria or qSOFA," the authors write. "It established that the use of an increase in SOFA score of 2 or more points to define sepsis was an appropriate data-based starting point, and would likely have broad external validity in ICU patients from developed countries."
In an email to ICU Management & Practice, Andrew Udy, Eamon Raith and David Pilcher, from the research group, commented: “Perhaps most surprising was how consistent and similar our findings were to those of the Sepsis-3 taskforce who promoted the new Sepsis definitions in JAMA in early 2016, even though they had only originally examined a much smaller number of Intensive Care admissions. Our findings were encouraging in that they provided external validity to support the new Sepsis-3 definitions, at least in modern ICUs in higher-income countries.”
Udy added: “For the clinician at the bedside, it emphasises the significance of organ dysfunction with infection in predicting a higher mortality risk for an individual patient…the concept underpinning the new definition of sepsis. This will potentially allow for better planning of treatment strategies and more informed discussions with patients and families. For the researcher and epidemiologist, we now have a consistent and well-validated method to diagnose sepsis which appears generalisable across different health care systems and which may assist development of clinical trials and interpretation of variation in outcomes.”
References:
Raith E, Udy AA, Bailey M, McGloughlin S, MacIsaac C, Bellomo R, Pilcher
DV for the Australian and New Zealand Intensive Care Society (ANZICS)
Centre for Outcomes and Resource Evaluation (CORE) (2017) Prognostic accuracy of the SOFA score, SIRS criteria, and qSOFA score for in-hospital mortality among adults with suspected infection admitted to the intensive care unit. JAMA, 317(3): 290-300.
doi:10.1001/jama.2016.20328
Latest Articles
SOFA, mortality, sepsis
Study: SOFA Score Helps Predict ICU Mortality