Readmissions due to sepsis are higher and costlier than for the four conditions already reported in the U.S. to measure quality of care and guide pay for performance, according to researchers from the University of Pittsburgh School of Medicine and VA Pittsburgh Healthcare System. Their research is published in JAMA to coincide with the presentation of the findings at the Society of Critical Care Medicine’s 46th Critical Care Congress, meeting in Hawaii. In their congress abstract, the authors report that one of seven patients with an index hospitalisation for sepsis is readmitted within 30 days, resulting in excess costs of almost 1.5 billion dollars annually.
This really puts in perspective how important sepsis is," commented lead author Florian B. Mayr, MD, MPH, faculty member in Pitt's Department of Critical Care Medicine and the Center for Health Equity Research and Promotion at the VA Pittsburgh, in a media release. "If we, as a nation, place such high emphasis on reducing readmissions for the other four conditions, then we really need to look for opportunities to improve outcomes for sepsis, which has a higher rate of readmission than heart failure. People who survive an initial episode of sepsis often don't do well. They return to the hospital frequently, accrue new health conditions and have significantly elevated death rates."
The Centers for Medicare & Medicaid Services (CMS) tracks readmissions within 30 days for acute myocardical infarction (AMI), heart failure, chronic obstructive pulmonary disease (COPD) and pneumonia. Mayr, with senior author Sachin Yende, MD, MS, associate professor in the Pitt School of Medicine's departments of Critical Care Medicine and Clinical and Translational Sciences and vice president of Critical Care at the VA Pittsburgh Healthcare System, and colleagues examined readmissions after index admissions for sepsis by analysing data from the 2013 Nationwide Readmissions Database, which includes data from 21 states, representing inpatient use for 49 percent of the U.S. population.
The authors suggest that adding sepsis to the CMS’ Hospital Readmission Reduction Program may prompt development of new interventions to improve sepsis outcomes and reduce unplanned readmissions and associated costs. In an email to ICU Management & Practice, Drs Yende and Mayr noted that CMS has developed a core sepsis measure (SEP-1), and policy makers are aware of the importance of sepsis as an issue for the healthcare system.
Sources: JAMA; University of Pittsburgh Schools of the Health Sciences
Image credit: Nicole Davison/UPMC
This really puts in perspective how important sepsis is," commented lead author Florian B. Mayr, MD, MPH, faculty member in Pitt's Department of Critical Care Medicine and the Center for Health Equity Research and Promotion at the VA Pittsburgh, in a media release. "If we, as a nation, place such high emphasis on reducing readmissions for the other four conditions, then we really need to look for opportunities to improve outcomes for sepsis, which has a higher rate of readmission than heart failure. People who survive an initial episode of sepsis often don't do well. They return to the hospital frequently, accrue new health conditions and have significantly elevated death rates."
The Centers for Medicare & Medicaid Services (CMS) tracks readmissions within 30 days for acute myocardical infarction (AMI), heart failure, chronic obstructive pulmonary disease (COPD) and pneumonia. Mayr, with senior author Sachin Yende, MD, MS, associate professor in the Pitt School of Medicine's departments of Critical Care Medicine and Clinical and Translational Sciences and vice president of Critical Care at the VA Pittsburgh Healthcare System, and colleagues examined readmissions after index admissions for sepsis by analysing data from the 2013 Nationwide Readmissions Database, which includes data from 21 states, representing inpatient use for 49 percent of the U.S. population.
Results
1,187,697 unplanned 30-day
readmissions, 2013:
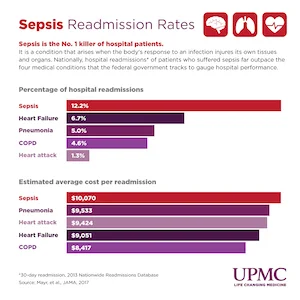
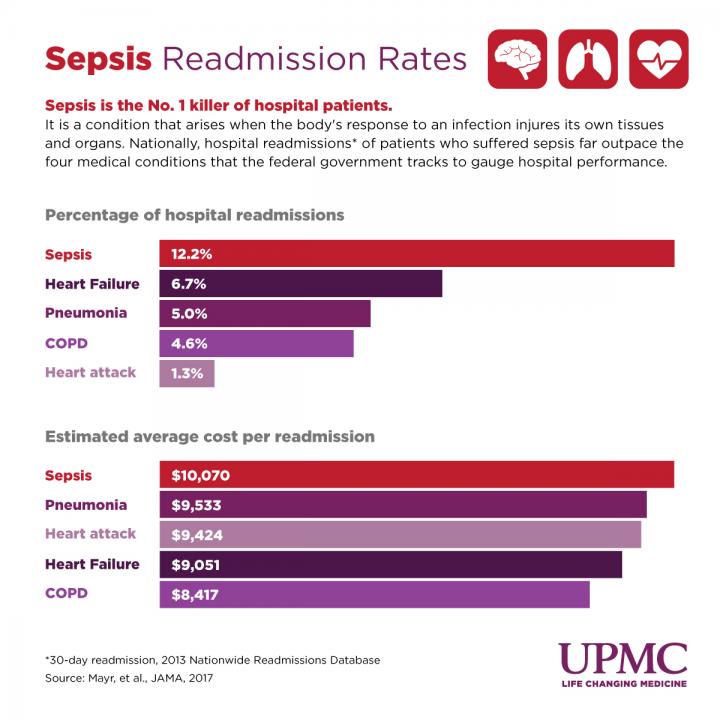
| % | Av. cost per readmission | |
| Sepsis | 12.2 | $10,070 |
| Heart failure | 6.7 | $9,051 |
| Pneumonia | 5 | $9,533 |
| COPD | 4.6 | $8,417 |
| AMI | 1.3 | $9,424 |
The authors suggest that adding sepsis to the CMS’ Hospital Readmission Reduction Program may prompt development of new interventions to improve sepsis outcomes and reduce unplanned readmissions and associated costs. In an email to ICU Management & Practice, Drs Yende and Mayr noted that CMS has developed a core sepsis measure (SEP-1), and policy makers are aware of the importance of sepsis as an issue for the healthcare system.
Sources: JAMA; University of Pittsburgh Schools of the Health Sciences
Image credit: Nicole Davison/UPMC

References:
Mayr F, Talisa VB, Balakumar V, Chang CCH, Fine M, Yende S (2017) Proportion and cost of unplanned 30-day readmissions after sepsis compared with other medical conditions. JAMA, E1-E2. Published online Jan 22.
Mayr F, Balakumar V, Talisa V, Fine M, Yende S (2017) 1336: Understanding the burden of unplanned sepsis readmissions, Society of Critical Care Medicine, 46th Critical Care Congress, 20-24 January 2017, Honolulu, Hawaii, USA.
Mayr F, Balakumar V, Talisa V, Fine M, Yende S (2017) 1336: Understanding the burden of unplanned sepsis readmissions, Society of Critical Care Medicine, 46th Critical Care Congress, 20-24 January 2017, Honolulu, Hawaii, USA.
Latest Articles
Sepsis, COPD, Pneumonia, heart failure, acute myocardial infarction, hospital readmissions
Readmissions due to sepsis are higher and costlier than for the four conditions already reported in the U.S. to measure quality of care and guide pay for p...