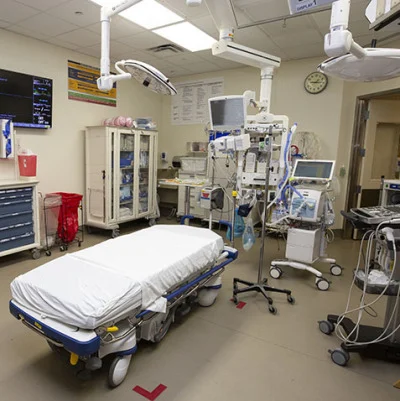
A study of the Massey Family Foundation Emergency Critical Care Center – EC3 found that the implementation of emergency department ICUs led to improved survival rates and better patient care.
Opened in February 2015, EC3 is a highly advanced critical care centre, next to the emergency department at Michigan Medical. The unit is equipped with five resuscitation trauma bays, nine patient rooms and critical care nurses and physicians to accommodate patient’s needs as they are admitted through the emergency department.
The study of EC3 was conducted by collecting electronic health records from the Michigan Medical emergency department from 1st September 2012 to 31st July 2017. These health records were then split and compared based on admissions before and after EC3 was opened and the mortality outcomes over 30 days and the admissions into the ICU were noted.
Lead author of the study published in JAMA Network Open, Kyle Gunnerson, M.D., explained how the pressure on emergency departments has meant that patients are waiting longer for critical care. It is these long waiting times for the ICU which are reducing patient survival. The implementation of EC3 saw a decrease in the mortality rate from 2.13% before EC3 to 1.83% after the EC3 was opened, and up to 30 days after patients were admitted to the emergency department evidence of survival benefit could be seen. Additionally, there was a decrease in hospital ICU admissions which went from 3.2% to 2.7%, as the EC3 meant that critical care could be initiated immediately.
Early intervention for the most critically ill patients led to improved patient outcomes. Robert Neumar, MD, PhD, senior author of the study, discussed how the results showed most patients did not need to be admitted into the ICU after they were treated in EC3 as these patients could be stabilised for non-ICU admission or discharged entirely. Also, the study demonstrated a 30% reduction in the odds for short ICU admissions, optimising bed allocations for patients in other wards and allowing an increase of ICU transfers from different hospitals.
Benjamin Bassin, MD, co-author of the study stressed how these results show the impact of critical care. As statistically, the implementation of the EC3 had saved the lives of one in 333 patients that had entered the hospital through the emergency department, totalling an additional life being saved every 36 hours.
Researchers hope that the findings of the study influence the objectives of critical care departments. As Nathan Haas, MD, co-author of the study explains, if health centres are not able to build units similar to EC3 certain strategies could be implemented and tailored to individual health centre’s needs and possibilities.
From design to implementation, researchers also stressed that this initiative would not be possible without teamwork. It is only through interdisciplinary work that this care delivery model could be created.
Source: Michigan Medicine - M Health LAB
Image Credit: Michigan Medicine - M Health LAB
References:
Gunnerson KJ, Bassin BS, Havey RA, et al. (2019) Association of an Emergency Department–Based Intensive Care Unit With Survival and Inpatient Intensive Care Unit Admissions. JAMA Netw Open. Published online July 24, 20192(7):e197584. doi:10.1001/jamanetworkopen.2019.7584
Latest Articles
ICU, Critical Care, emergency department, University of Michigan Health System, EC3, Emergency Department-Based Intensive Care Improves Patient Survival, Michigan Medicine, Massey Family Foundation Emergency Critical Care Center – EC3, Massey Family Foundation Emergency Critical Care Center, Emergency Department-Based Intensive Care
A study of the Massey Family Foundation Emergency Critical Care Center – EC3 found that the implementation of emergency department ICUs led to improved survival rates and better patient care.