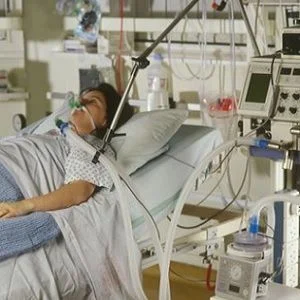
A new analytical tool developed at Thomas Jefferson University Hospital can help identify surgical patients at risk for respiratory complications. Using data from the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP®), the Jefferson researchers devised a scoring system to identify risk factors for ventilator dependence after major operations.
Estimates put mechanical ventilation expenditure at $1,522 per day per patient in the intensive care unit. Although the need for ventilation is not widespread — about one to three percent of patients who have non-emergency surgical procedures require ventilation afterward — the consequences are nonetheless significant, according to researchers.
"The need for artificial mechanical ventilation after operations is infrequent, but when it happens it does carry high costs," says study co-author Adam P. Johnson, MD, MPH. "Ventilator dependence is highly associated with mortality, and in and of itself is a morbidity."
The Jefferson team examined ACS NSQIP data on 7,473 patients who had elective general or vascular operations at the institution between 2006 and 2013. The scoring system assigned points for different factors, such as current smoker (1 point), age older than 60 years (2 points), and oesophagus procedures (3 points). Total risk scores ranged from 0 to 7 for study subjects. The median risk score for patients who did not need the ventilator after operations was 2, while that for patients who did need the ventilator was 3. Those with a score above 3 comprised the 20 percent of patients who experienced 70 percent of adverse events, the researchers explained.
Other risk factors associated with postoperative ventilator dependence were a diagnosis of severe chronic obstructive pulmonary disease; signs of active infection or inflammatory response; and low albumin counts, a sign of malnutrition. "Our goal was to quantify how each factor affects the risk of ventilator dependence," said Dr. Johnson. After identifying this smaller set of high risk patients, "the goal then is to optimise them before and during their hospital stay," he added.
The team says other hospitals may be able to use the scoring system to identify ventilator dependence risks in their own patient populations. "Our institution's risk score may not be generalisable, but the methodology of how we developed and then implemented the risk score may be used at other hospitals when looking at their own patients," Dr. Johnson said.
The findings were presented at the 2015 American College of Surgeons National Surgical Quality Improvement Program Conference.
Source: American College of Surgeons
Image credit: Google images
new method to avoid costly postoperative ventilation
Estimates put mechanical ventilation expenditure at $1,522 per day per patient in the intensive care unit. Although the need for ventilation is not widespread — about one to three percent of patients who have non-emergency surgical procedures require ventilation afterward — the consequences are nonetheless significant, according to researchers.
"The need for artificial mechanical ventilation after operations is infrequent, but when it happens it does carry high costs," says study co-author Adam P. Johnson, MD, MPH. "Ventilator dependence is highly associated with mortality, and in and of itself is a morbidity."
The Jefferson team examined ACS NSQIP data on 7,473 patients who had elective general or vascular operations at the institution between 2006 and 2013. The scoring system assigned points for different factors, such as current smoker (1 point), age older than 60 years (2 points), and oesophagus procedures (3 points). Total risk scores ranged from 0 to 7 for study subjects. The median risk score for patients who did not need the ventilator after operations was 2, while that for patients who did need the ventilator was 3. Those with a score above 3 comprised the 20 percent of patients who experienced 70 percent of adverse events, the researchers explained.
Other risk factors associated with postoperative ventilator dependence were a diagnosis of severe chronic obstructive pulmonary disease; signs of active infection or inflammatory response; and low albumin counts, a sign of malnutrition. "Our goal was to quantify how each factor affects the risk of ventilator dependence," said Dr. Johnson. After identifying this smaller set of high risk patients, "the goal then is to optimise them before and during their hospital stay," he added.
The team says other hospitals may be able to use the scoring system to identify ventilator dependence risks in their own patient populations. "Our institution's risk score may not be generalisable, but the methodology of how we developed and then implemented the risk score may be used at other hospitals when looking at their own patients," Dr. Johnson said.
The findings were presented at the 2015 American College of Surgeons National Surgical Quality Improvement Program Conference.
Source: American College of Surgeons
Image credit: Google images
new method to avoid costly postoperative ventilation
Latest Articles
healthmanagement, mechanical ventilation, risk factors, scoring system, surgery, respiratory
Using data from the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP®), researchers devised a scoring system to identify risk factors for ventilator dependence after major operations.