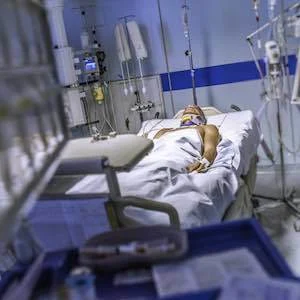
A group of researchers from France and six other countries assessed the influence of neutropaenia on outcome of critically ill cancer patients by meta-analysis of individual data. Among 7,512 critically ill cancer patients included in this systematic review, neutropaenia was independently associated with poor outcome despite a meaningful survival.
You might also like: Caring for critically ill immunocompromised patients
Neutropaenia remains a common side effect of most treatments administered to haematological patients. Neutropaenia is associated with complications that include severe sepsis, acute respiratory failure and specific conditions such as neutropaenic enterocolitis. Although neutropaenia remains associated with a poor outcome in general ICU populations, several recent studies failed to demonstrate an impact of neutropaenia on the outcome of critically ill cancer patients.
This systematic review was a preplanned follow-up study of an initial meta-analysis on aggregated data. (Bouteloup M et al. 2017) Neutropaenia was defined as a neutrophil count (or if missing as a white blood cell count) lower than 1 G/L (stage 3 or more according to Common Terminology Criteria for Adverse Events version 4.03). Data sources were PubMed and the Cochrane database. Study selection included articles focusing on critically ill cancer patients published in English and studies in humans from May 2005 to May 2015. Individual data from selected studies were obtained from corresponding authors.
Overall, 114 studies were identified and authors of 30 studies (26.3% of selected studies) agreed to participate in this study. Of the 7,515 included patients, three were excluded due to a missing major variable (neutropaenia or mortality) leading to analysis of 7,512 patients, including 1,702 neutropaenic patients (22.6%).
After adjustment for confounders, and taking study effect into account, neutropaenia was independently associated with mortality (OR 1.41; 95% CI 1.23–1.62; P = 0.03). When analysed separately, neither admission period, underlying malignancy nor need for mechanical ventilation modified the prognostic influence of neutropaenia on outcome. However, among patients for whom data on G-CSF administration were available (n = 1949; 25.9%), neutropaenia was no longer associated with outcome in patients receiving G-CSF (OR 1.03; 95% CI 0.70–1.51; P = 0.90).
The results strongly suggest that neutropaenia, conversely to the recently published recommendations, should be considered a prognostic factor. However, additional studies are needed to confirm these data and to identify room for improvements in the management of this specific population, according to the review team.
This study, published in Critical Care, is the first to date to suggest indirectly that G-CSF may limit the prognostic impact of neutropaenia in critically ill patients. Although this finding is insufficient to modify existing recommendations, additional interventional studies in this setting may be warranted.
Image credit: iStock
Furthermore, the results showed the prognostic impact of neutropaenia was unchanged when stratifying for malignancy, period of ICU admission or use of mechanical ventilation. Interestingly, neutropaenia was no longer significantly associated with outcome in patients treated with granulocyte colony stimulating factor (G-CSF), suggesting a beneficial effect of G-CSF in neutropaenic critically ill cancer patients.
You might also like: Caring for critically ill immunocompromised patients
Neutropaenia remains a common side effect of most treatments administered to haematological patients. Neutropaenia is associated with complications that include severe sepsis, acute respiratory failure and specific conditions such as neutropaenic enterocolitis. Although neutropaenia remains associated with a poor outcome in general ICU populations, several recent studies failed to demonstrate an impact of neutropaenia on the outcome of critically ill cancer patients.
This systematic review was a preplanned follow-up study of an initial meta-analysis on aggregated data. (Bouteloup M et al. 2017) Neutropaenia was defined as a neutrophil count (or if missing as a white blood cell count) lower than 1 G/L (stage 3 or more according to Common Terminology Criteria for Adverse Events version 4.03). Data sources were PubMed and the Cochrane database. Study selection included articles focusing on critically ill cancer patients published in English and studies in humans from May 2005 to May 2015. Individual data from selected studies were obtained from corresponding authors.
Overall, 114 studies were identified and authors of 30 studies (26.3% of selected studies) agreed to participate in this study. Of the 7,515 included patients, three were excluded due to a missing major variable (neutropaenia or mortality) leading to analysis of 7,512 patients, including 1,702 neutropaenic patients (22.6%).
After adjustment for confounders, and taking study effect into account, neutropaenia was independently associated with mortality (OR 1.41; 95% CI 1.23–1.62; P = 0.03). When analysed separately, neither admission period, underlying malignancy nor need for mechanical ventilation modified the prognostic influence of neutropaenia on outcome. However, among patients for whom data on G-CSF administration were available (n = 1949; 25.9%), neutropaenia was no longer associated with outcome in patients receiving G-CSF (OR 1.03; 95% CI 0.70–1.51; P = 0.90).
The results strongly suggest that neutropaenia, conversely to the recently published recommendations, should be considered a prognostic factor. However, additional studies are needed to confirm these data and to identify room for improvements in the management of this specific population, according to the review team.
This study, published in Critical Care, is the first to date to suggest indirectly that G-CSF may limit the prognostic impact of neutropaenia in critically ill patients. Although this finding is insufficient to modify existing recommendations, additional interventional studies in this setting may be warranted.
Image credit: iStock
References:
Georges Q, Azoulay E, Mokart D, Darmon M et al. (2018) Influence of neutropenia on mortality of critically ill cancer patients: results of a meta-analysis on individual data. Critical Care 22:326. https://doi.org/10.1186/s13054-018-2076-z
Bouteloup M, Perinel S, Bourmaud A et al. (2017) Outcomes in adult critically ill cancer patients with and without neutropenia: a systematic review and meta-analysis of the Groupe de Recherche en Réanimation Respiratoire du patient d’Onco-Hématologie (GRRR-OH). Oncotarget, 8:1860–70.
Latest Articles
Cancer, mortality, in-hospital mortality, Critically ill, neutropaenia
A group of researchers from France and six other countries assessed the influence of neutropaenia on outcome of critically ill cancer patients by meta-anal...