The use of the mechanical chest compression device LUCAS-2 represents poor value for money when compared to standard manual chest compression in out-of-hospital cardiac arrest, according to a new study published in the journal Resuscitation.
A critical step of the resuscitation process is early cardiopulmonary resuscitation (CPR) – i.e., the combination of chest compressions and ventilations. CPR can be started by bystanders and is typically taken over by emergency services. Current resuscitation guidelines highlight the importance of high-quality CPR for ensuring optimal outcomes from cardiac arrest. In this context, several mechanical devices have been proposed that are able to provide compressions of a standard depth and frequency for long periods without interruption or fatigue.
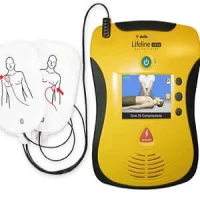
The LUCAS-2 (Lund University Cardiopulmonary Assistance System) is a mechanical device that provides automatic chest compressions, manufactured in Sweden by PhysioControl. It delivers sternal compression at a constant rate to a fixed depth and has been on the market since 2002 in Europe. In this study, researchers assessed the cost-effectiveness of the LUCAS-2 device versus manual CPR in adults with non-traumatic, out-of-hospital cardiac arrest.
The researchers analysed patient-level data from a large, pragmatic, multicentre trial – the PARAMEDIC trial – linked to administrative secondary care data from the Hospital Episode Statistics (HES) to measure healthcare resource use, costs and outcomes in both arms. A within-trial analysis using quality adjusted life years derived from the EQ-5D-3L was conducted at 12-month follow-up and results were extrapolated to the lifetime horizon using a decision-analytic model.
Among the 4,771 patients enrolled in the trial, 1,652 were assigned to the intervention group (LUCAS-2) and 2,819 were assigned to the control group (manual CPR). At 12 months, 89 (5%) patients survived in the LUCAS-2 group and 175 (6%) survived in the manual CPR group. In the vast majority of analyses conducted, both within-trial and by extrapolation of the results over a lifetime horizon, manual CPR dominates LUCAS-2. In other words, patients in the LUCAS-2 group had poorer health outcomes (i.e., lower QALYs) and incurred higher health and social care costs.
"The cost-effectiveness results are driven by worse neurological outcomes and lower survival in the LUCAS-2 group as compared to manual CPR. Results resonate with previously published short-term clinical outcomes observed in the PARAMEDIC trial and are in line with several other randomised trials that have investigated the effectiveness of mechanical chest compression and that found no consistent evidence of survival benefits and highly heterogeneous effects in terms of neurological outcomes," the authors write.
Possible explanations for worse outcomes in the LUCAS-2 group include interruptions in CPR during device deployment that could cause reduced cardiac and cerebral perfusion and possible delay in the time to first shock due to the deployment of LUCAS-2. More intensive initial training, regular re-training adopting a “pit-stop” approach with on-going CPR quality monitoring may reduce potentially deleterious interruptions to CPR associated with device deployment, according to the researchers.
While several other studies have assessed the effectiveness of mechanical chest compression devices in out-of-hospital cardiac arrest, the researchers say their study is the first comprehensive economic evaluation in this area. The analysis also provides useful costs and health-related quality-of-life (HRQoL) estimates that will be of use in future economic models.
Source: Resuscitation
Image Credit: sasastro
References:
Marti, Joachim et al. (2017) The cost-effectiveness of a mechanical compression device in out-of-hospital cardiac arrest. Resuscitation. doi.org/10.1016/j.resuscitation.2017.04.036
Latest Articles
CPR, out-of-hospital cardiac arrest, LUCAS-2, mechanical chest compression
The use of the mechanical chest compression device LUCAS-2 represents poor value for money when compared to standard manual chest compression in out-of-hospital cardiac arrest, according to a new study published in the journal Resuscitation.