Photograph of the King’s College Hospital, Oxford University and OrganOx team following successful connection of the first human liver for transplant onto the OrganOx Metra device (Credit: Image courtesy of University of Oxford)
In a world first, a donated human liver has been 'kept alive' outside
a human being and then successfully transplanted into a patient in need
of a new liver.
So far the procedure has been performed on two
patients on the liver transplant waiting list and both are making
excellent recoveries.
Currently transplantation depends on
preserving donor organs by putting them ‘on ice’ – cooling them to slow
their metabolism. But this often leads to organs becoming damaged.
The
technology, developed at Oxford University and now being trialled at
the liver transplant centre at King’s College Hospital as part of a
controlled clinical investigation, could preserve a functioning liver
outside the body for 24 hours. A donated human liver connected to the
device is raised to body temperature and oxygenated red blood cells are
circulated through its capillaries. Once on the machine, a liver
functions normally just as it would inside a human body, regaining its
colour and producing bile.
The results from the first two
transplants, carried out at King’s College Hospital in February 2013,
suggest that the device could be useful for all patients needing liver
transplants. Based on pre-clinical data, the new device could also
enable the preservation of livers which would otherwise be discarded as
unfit for transplantation – potentially as much as doubling the number
of organs available for transplant and prolonging the maximum period of
organ preservation to 24 hours.
‘These first clinical cases
confirm that we can support human livers outside the body, keep them
alive and functioning on our machine and then, hours later, successfully
transplant them into a patient,’ said Professor Constantin Coussios of
Oxford University's Department of Engineering Science, one of the
machine's inventors and Technical Director of OrganOx, the University
spin-out created to bring the device from bench to bedside.
‘The
device is the very first completely automated liver perfusion device of
its kind: the organ is perfused with oxygenated red blood cells at
normal body temperature, just as it would be inside the body, and can
for example be observed making bile, which makes it an extraordinary
feat of engineering.
‘It was astounding to see an initially cold grey liver flushing with colour once hooked up to our machine and performing as it would within the body. What was even more amazing was to see the same liver transplanted into a patient who is now walking around.’
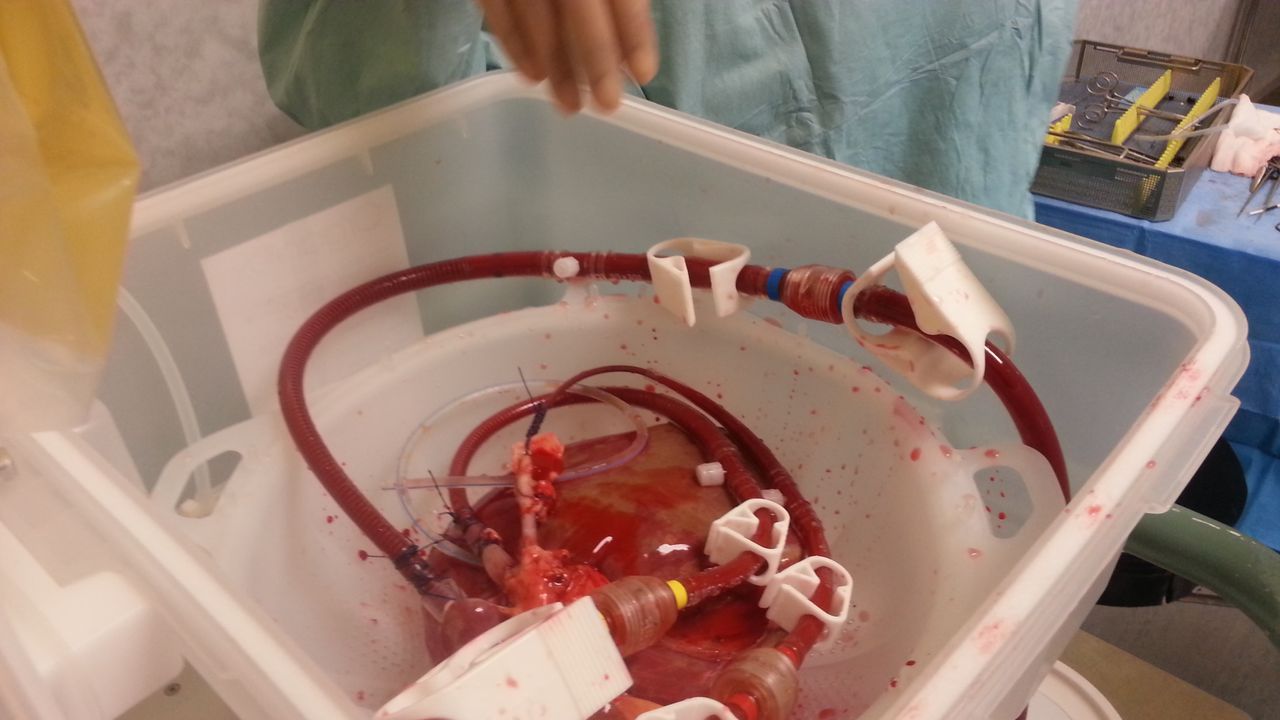
Liver 30 seconds after connection to the OrganOx Metra device (parts of the organ are still cold, whilst others are warm and perfused with the red cell solution) (Credit: Image courtesy of University of Oxford)
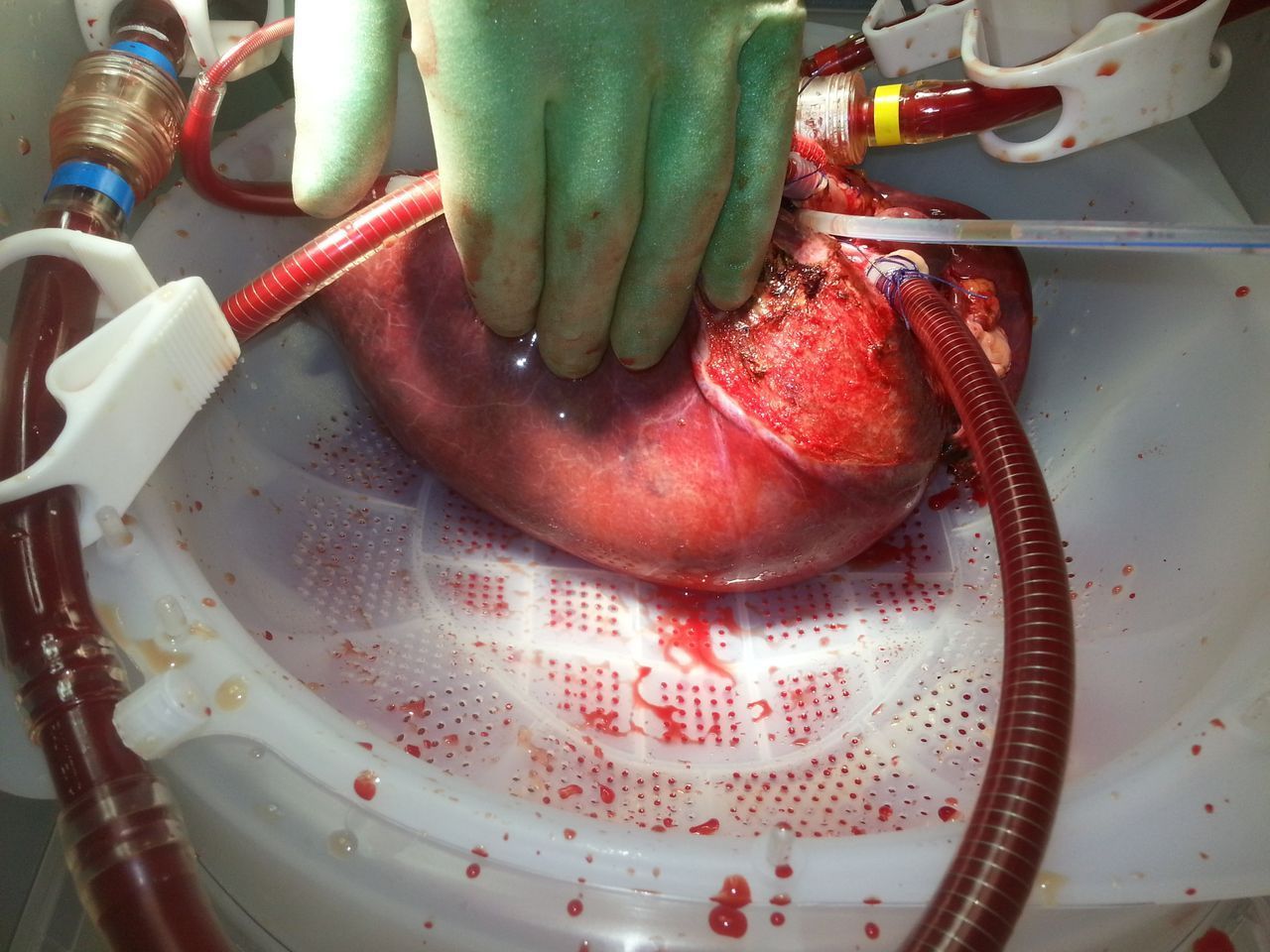
Organ some 5 minutes after connection to the OrganOx Metra, now fully perfused and at physiological temperature (Credit: Image courtesy of University of Oxford)
‘Whilst for these two transplants we only needed to keep
the livers alive for up to 10 hours, in other experiments we have shown
we can preserve a functioning liver and monitor its function outside the
body for periods up to 24 hours.’
Professor Nigel Heaton,
Consultant Liver Transplant Surgeon and Director of Transplant Surgery
at King’s College Hospital, said: ‘Despite all the advances in modern
medicine, the fundamentals of liver transplantation have not changed in
decades. This is why the device is so exciting. If we can introduce
technology like this into everyday practice, it could be a real, bona
fide game changer for transplantation as we know it. Buying the surgeon
extra time extends the options open to our patients, many of whom would
otherwise die waiting for an organ to become available.’
Mr Wayel
Jassem, Consultant Liver Transplant Surgeon at King’s College Hospital,
who performed both transplant operations, said: ‘There is always huge
pressure to get a donated liver to the right person within a very short
space of time. For the first time, we now have a device that is designed
specifically to give us extra time to test the liver, to help maximise
the chances of the recipient having a successful outcome. This
technology has the potential to be hugely significant, and could make
more livers available for transplant, and in turn save lives.’
Ian
Christie, 62, the first person to receive a transplanted liver kept
alive on the device, said: ‘In May 2012, I was told I had cirrhosis of
the liver and without a transplant I had an estimated 12-18 months to
live. I was placed on the waiting list but I was told there was about
12-18 months to wait for a liver of my type. I was very worried it was
cutting it a bit too fine and I wouldn’t get a transplant.
‘The
waiting is horrible. Sometimes I would forget about the transplant but
then I would catch sight of the bag in the corner of the room that I had
packed ready to go and then I would remember. You’re waiting for the
phone to ring, wondering “Are they ever going to call me? Are they ever
going to call me?”.
‘I took part in the trial because I just think
it’s the right thing to do. If the device can help more people in my
situation in the future, it’s my duty to help. I trusted that the
doctors wouldn’t go ahead with it unless they were absolutely sure so I
knew there wasn’t a risk to my transplant.
‘Three days after the
surgery, Mr Jassam from King’s and the professors from Oxford arrived in
my room with absolutely beaming smiles. They look like they are
normally quite serious gentlemen so I knew it was a good sign to see
them so pleased.
‘I feel better than I’ve felt for 10-15 years,
even allowing for the pain and wound that’s got to heal. I’m getting
better and better day by day. I just feel so alive!
‘It’s so easy
to get carried away and become euphoric, but things can still go wrong,
so I’m trying to keep my feet on the ground and take it day by day.’
Professor
Coussios and Professor Peter Friend, of Oxford University's Nuffield
Department of Surgical Sciences and Director of the Oxford Transplant
Centre, and colleagues have been researching the technology since 1994.
Professor
Peter Friend said: ‘Transplant surgery is a victim of its own success
with far more people needing transplants than there are donor organs
available. This device has the potential to change that situation
radically. By enabling us to transplant many organs that are unusable
with current techniques, this technology could bring benefit to a large
number of patients awaiting transplants, many of whom currently die
whilst still waiting.
‘At present, organ transplantation depends
upon cooling the organ to ice temperature to slow down its metabolism,
but this does not stop it deteriorating and, if the organ is already
damaged in some way, perhaps by being deprived of oxygen, then the
combined effect can be disastrous. Many potential donor organs are
declined as being unsuitable for this reason.
‘This new technique
allows us to assess how well an organ is working before having to decide
whether to commit a patient to the operation. So this technology
promises to quality-assure organs which would otherwise be discarded.
This would increase the number of transplants without increasing the
risks. It will make a real difference to what happens to patients on the
waiting list without requiring any change in current donation
practices.’
In 2008 the spin-out company OrganOx was formed,
through the University's technology transfer firm Isis Innovation, in
order to commercialise the Oxford research. OrganOx, headed by CEO Dr
Les Russell, developed the device for these first clinical trials.
‘In
Europe and the US, around 13,000 liver transplants are undertaken each
year,’ said OrganOx CEO Dr Les Russell. ‘However, there is a combined
waiting list of around 30,000 patients and up to 25 per cent of these
patients die whilst awaiting transplantation. Meanwhile, over 2000
livers are discarded annually because they are either damaged by oxygen
deprivation or do not survive cold preservation due to elevated
intracellular fat’.
King’s College Hospital is home to the largest
liver transplant centre in Europe, and carries out over 200 transplants
every year, on adults and children.
Source: University of Oxford























