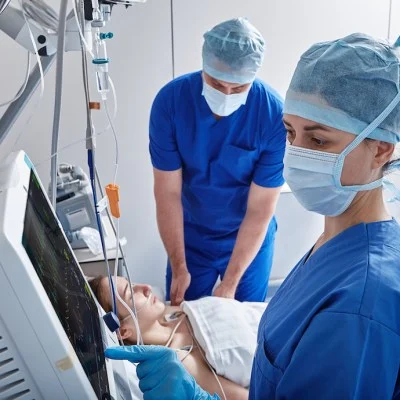
The treatment of critically ill and perioperative patients often involves targeting blood pressure as a cornerstone of haemodynamic management. Current guidelines suggest maintaining high blood pressure targets for these patients based on observational studies linking hypotensive events to adverse outcomes. However, these recommendations are not based on causal relationships but on associations.
While interventions to treat low blood pressure can be life-saving, the threshold at which interventions might become harmful is uncertain. Treatments like fluids, vasopressors, and inotropes used to raise blood pressure may also have negative consequences, such as fluid overload, increased myocardial oxygen consumption, and excessive vascular resistance.
Moreover, targeting higher blood pressure doesn't always improve microcirculatory blood flow. Therefore, the key question is whether hypotension directly causes adverse events and if managing to achieve higher blood pressure would benefit patients.
A study compared the effects of lower versus higher blood pressure targets on survival in randomised controlled trials involving critically ill and perioperative patients. The hypothesis was that a vasopressor-sparing strategy and other protective haemodynamic management techniques might benefit these patients.
The study included RCTs comparing higher and lower blood pressure targets in critically ill and perioperative populations. "Target" was defined as the minimum tolerated value from which treatment, such as vasoconstrictors, was initiated to increase blood pressure.
Of the 2940 studies identified, 28 were included, comprising 15,672 patients (12 in critically ill and 16 in perioperative settings). Patients in the low blood pressure target group exhibited lower mortality (13.3% vs. 14.4%). These results were primarily observed in ICU settings and with treatments lasting over 24 hours. Sensitivity analyses, including those restricted to low risk of bias studies, showed similar trends. Additionally, lower rates of atrial fibrillation and reduced need for transfusion were observed in the low-pressure target groups, while no differences were found in other secondary outcomes.
Evidence from this review suggests that targeting lower blood pressure levels compared to higher targets reduces mortality, atrial fibrillation, and transfusion requirements. While lower blood pressure targets show potential benefits, there remains ongoing uncertainty. Importantly, this meta-analysis diverges from previous findings and recommendations. These results could shape future guidelines and encourage further exploration of protective haemodynamics.
Source: Critical Care Medicine
Image Credit: iStock