Failure to reliably diagnose ARDS, or acute respiratory distress syndrome, could lead to underrecognition and undertreatment in clinical practice. New research shows the reliability of the Berlin ARDS definition is "moderate," driven primarily by differences in chest imaging interpretation. The study is in press in the journal CHEST.
The 2012 revision to the ARDS definition sought to improve the validity and reliability of the previous American-European Consensus Conference definition. However, the Berlin definition’s success in improving the reliability of ARDS diagnosis in clinical practice is unknown. The new study examined the interobserver reliability of each aspect of the Berlin ARDS definition.
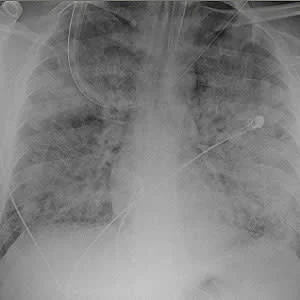
"Clinicians had only moderate interobserver agreement when diagnosing ARDS in patients with hypoxic respiratory failure under the Berlin criteria, and the major driver of this variability was differences in how chest images were interpreted," the study’s authors write.
In this study, 205 patients with hypoxic respiratory failure from four ICUs were reviewed independently by three clinicians, who evaluated whether patients had ARDS, the diagnostic confidence of the reviewers, whether patients met individual ARDS criteria, and the time when criteria were met.
Based on the results, interobserver reliability of an ARDS diagnosis was “moderate” (kappa = 0.50; 95% CI, 0.40-0.59). Sixty-seven percent of diagnostic disagreements between clinicians reviewing the same patient was explained by differences in how chest imaging studies were interpreted, with other ARDS criteria contributing less (identification of ARDS risk factor, 15%; cardiac oedema/volume overload exclusion, 7%).
The results also show that combining the independent reviews of three clinicians can increase reliability to “substantial” (kappa = 0.75; 95% CI, 0.68-0.80). When a clinician diagnosed ARDS with “high confidence,” all other clinicians agreed with the diagnosis in 72% of reviews. There was close agreement between clinicians about the time when a patient met all ARDS criteria if ARDS developed within the first 48 hours of hospitalisation (median difference, 5 hours).
"Strategies such as combining multiple independent reviews made by clinicians or using a clinician’s confidence in their review can increase the uniformity of the diagnosis of ARDS," the authors note. "When a simple majority of clinicians diagnosed a patient with ARDS, they agreed closely on the time when all ARDS criteria were present if onset was during the first 48 hours of hospitalisation."
The study's results highlight the need for better approaches to identifying patients with bilateral airspace disease. However, whether additional training improves reliability of chest radiograph interpretation is uncertain, say the authors, citing data from previous studies. They add: "Alternative approaches might include increasing the use of CT, lung ultrasonography, or automated processing of digital images, or greater engagement with radiologists as independent reviewers."
With the 2017 ARDS mechanical ventilation guidelines recommending prone positioning for severe ARDS, the need for precise ARDS diagnosis exists, the authors explain. The current study suggests that clinicians should seek out colleagues to evaluate patients independently when higher certainty is required. However, in scenarios in which other clinicians are unavailable, diagnostic confidence is also a meaningful measure. In the current study, when a clinician diagnosed ARDS with “high confidence,” other clinicians agreed with the diagnosis in most cases.
Source: CHEST
Image Credit: James Heilman, MD
References:
Sjoding MW, Hofer TP, Co I, Courey A, Cooke CR, Iwashyna TJ (2017) Interobserver Reliability of the Berlin ARDS Definition and Strategies to Improve the Reliability of ARDS Diagnosis. CHEST. dx.doi.org/10.1016/j.chest.2017.11.037
Latest Articles
acute respiratory distress syndrome, ARDS, hypoxic respiratory failure
Failure to reliably diagnose ARDS, or acute respiratory distress syndrome, could lead to underrecognition and undertreatment in clinical practice. New research shows the reliability of the Berlin ARDS definition is "moderate," driven primarily by differen