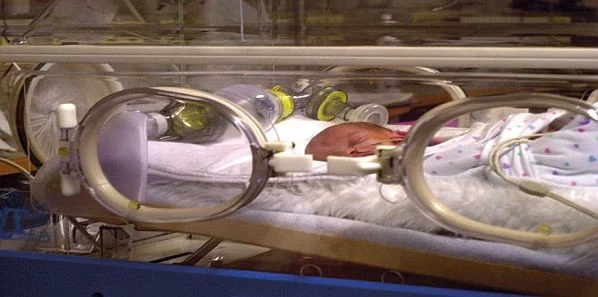
Worldwide, an estimated three to six percent of newborn infants need assisted positive pressure ventilation (PPV) at birth. Adequate PPV is the cornerstone for effective neonatal resuscitation. However, achieving effective manual ventilation can be difficult because most clinicians are not aware when a mask leaks or airway obstruction occurs and excessive peak inflation pressures (PIP) are delivered (above 35 cm H2O).
Studies have shown that proper training significantly improves mask ventilation given by experienced and inexperienced caregivers. In previous studies, a T-piece resuscitator (TPR) – the most commonly used device in developed countries and one often recommended by experts – was used. However, in guidelines a self-inflating bag (SIB) and mask are also recommended for neonatal resuscitation. The SIB is widely used in low- and middle-income countries given the limited access to continuous gas flow. The SIB is positioned horizontally and attached to the mask in a 90° angle and this could make it more difficult to create an adequate mask seal. Also, with a SIB more variable pressures are given, which can lead to either inadequate or excessive volumes delivered to the lung which may cause lung injury.
Giving mask training that is short and simple, with the emphasis on key points, is in line with the current concept of using simplified versions of neonatal resuscitation in developing countries. This study therefore aimed to test the effectiveness of a two-minute training drill consisting of a few key points in ventilation using the SIB.
Materials and Participants
The neonatal intensive care unit (NICU) of the Leiden University Medical Centre is a tertiary level perinatal centre with 400 intensive care admissions on average per year. Experienced and inexperienced caregivers were asked to mask ventilate a leak-free mannequin (fitted with a 50 ml test lung) using the SIB before and after the training.
PPV was applied using a Laerdal size 0/1 round mask in combination with a Laerdal Silicone Resuscitator Pediatric Basic SIB. The SIB has a pressure release valve (35 cm H2O), but has no positive end expiratory pressure (PEEP) valve and no manometer attached. Mask leak and pressure were measured using a Respiratory Function Monitor (RFM). It uses a hot-wire anemometer with a dead space of 1 ml to measure gas flow in and out of the face mask. The sensor was placed between the SIB and the facemask. The flow signal was automatically integrated to provide inspired- and expired tidal volumes (Vti and Vte). The Florian was permanently switched on during the procedure to minimise drift and the flow sensor was calibrated before each measurement. The participants were blinded to the output of the RFM.
The experienced group consisted of 27 neonatologists, fellows and senior registrars who received neonatal resuscitation education, including mask ventilation technique with RFM feedback, at least once during their training and applied mask ventilation in newborns on a regular basis. Experienced caregivers were included to determine if a short training exercise was also effective for them. The inexperienced group included 25 junior registrars, neonatal and obstetric nurses who received education on neonatal resuscitation during their general training, but did not train in face mask ventilation technique with RFM feedback, and rarely used mask ventilation in a clinical setting.
Before training, participants were asked to mask ventilate a leak-free mannequin at a rate of 40–60 inflations per minute using the technique they had been taught during their training. Participants received no further instructions but were asked to use chest excursion for evaluation of the mask ventilation given.
The Short 'Key Points' Training
Verbal instruction and the demonstration were standardised before commencing the study. Duration of the training has been clocked a few times during the study, which was approximately two minutes. All participants received a verbal instruction and demonstration by one instructor.
The following key-points were explained in two minutes: 1) positioning of the head in neutral position; 2) placing of the mask on the baby's chin, rolling over the mask onto the face without encroaching the eyes; 3) two point top hold using index finger and thumb and evenly applying pressure on the mask; 4) holding the ipsi- or contralateral mandible in order to squeeze the mask at the face without applying pressure on the occiput of the skull; and 5) a gentle squeeze in the bag with one finger and thumb is enough to deliver appropriate tidal volumes.
Immediately after the instruction, the second round of recordings were made, participants were not allowed to practise first and the instruction was only performed once for each participant.
Analysis and Results
Mask leak, PIP given and dispersion of pressures (expressed in SD) before and after training were analysed and compared. Pressures above 35 cm H2O were considered excessive. All signals were digitised and recorded at 200 Hz using a laptop with a data acquisition program (Spectra, Grove Medical, Hampton, England). Breaths were analysed on a breath-to-breath basis. Parameters were compared using a Wilcoxon non-parametric test.
Before and after the short training, experienced caregivers had minimal median (IQR) mask leak [14 (3-75) vs. 3 (0-53) percent; p<0.01]. Inexperienced users had large leak which decreased from 51 (7-91) percent before training to 11 (2-71) percent after training (p<0.01). Pressures above 35 cm H2O hardly occurred in experienced caregivers [0 (0-5) vs. 0 (0-0) percent; non-significant difference]. In inexperienced caregivers this frequently occurred but decreased considerably after training [94 (46-100) vs. 2 (0-70) percent; p<0.01].
Conclusion
The two-minute training on bag and mask ventilation was effective. This short and simple 'key points' training significantly decreased mask leak to acceptable levels in both experienced and inexperienced caregivers. The training had no influence in the inconsistency of the given pressures. However, the amount of high pressures given by inexperienced users, for which the pop-off valve apparently does not protect, considerably decreased after training. To improve immediate ventilation skills, this two-minute bag and mask training could easily be incorporated into training programmes.
Image Credit: Laerdal.com
Studies have shown that proper training significantly improves mask ventilation given by experienced and inexperienced caregivers. In previous studies, a T-piece resuscitator (TPR) – the most commonly used device in developed countries and one often recommended by experts – was used. However, in guidelines a self-inflating bag (SIB) and mask are also recommended for neonatal resuscitation. The SIB is widely used in low- and middle-income countries given the limited access to continuous gas flow. The SIB is positioned horizontally and attached to the mask in a 90° angle and this could make it more difficult to create an adequate mask seal. Also, with a SIB more variable pressures are given, which can lead to either inadequate or excessive volumes delivered to the lung which may cause lung injury.
Giving mask training that is short and simple, with the emphasis on key points, is in line with the current concept of using simplified versions of neonatal resuscitation in developing countries. This study therefore aimed to test the effectiveness of a two-minute training drill consisting of a few key points in ventilation using the SIB.
Materials and Participants
The neonatal intensive care unit (NICU) of the Leiden University Medical Centre is a tertiary level perinatal centre with 400 intensive care admissions on average per year. Experienced and inexperienced caregivers were asked to mask ventilate a leak-free mannequin (fitted with a 50 ml test lung) using the SIB before and after the training.
PPV was applied using a Laerdal size 0/1 round mask in combination with a Laerdal Silicone Resuscitator Pediatric Basic SIB. The SIB has a pressure release valve (35 cm H2O), but has no positive end expiratory pressure (PEEP) valve and no manometer attached. Mask leak and pressure were measured using a Respiratory Function Monitor (RFM). It uses a hot-wire anemometer with a dead space of 1 ml to measure gas flow in and out of the face mask. The sensor was placed between the SIB and the facemask. The flow signal was automatically integrated to provide inspired- and expired tidal volumes (Vti and Vte). The Florian was permanently switched on during the procedure to minimise drift and the flow sensor was calibrated before each measurement. The participants were blinded to the output of the RFM.
The experienced group consisted of 27 neonatologists, fellows and senior registrars who received neonatal resuscitation education, including mask ventilation technique with RFM feedback, at least once during their training and applied mask ventilation in newborns on a regular basis. Experienced caregivers were included to determine if a short training exercise was also effective for them. The inexperienced group included 25 junior registrars, neonatal and obstetric nurses who received education on neonatal resuscitation during their general training, but did not train in face mask ventilation technique with RFM feedback, and rarely used mask ventilation in a clinical setting.
Before training, participants were asked to mask ventilate a leak-free mannequin at a rate of 40–60 inflations per minute using the technique they had been taught during their training. Participants received no further instructions but were asked to use chest excursion for evaluation of the mask ventilation given.
The Short 'Key Points' Training
Verbal instruction and the demonstration were standardised before commencing the study. Duration of the training has been clocked a few times during the study, which was approximately two minutes. All participants received a verbal instruction and demonstration by one instructor.
The following key-points were explained in two minutes: 1) positioning of the head in neutral position; 2) placing of the mask on the baby's chin, rolling over the mask onto the face without encroaching the eyes; 3) two point top hold using index finger and thumb and evenly applying pressure on the mask; 4) holding the ipsi- or contralateral mandible in order to squeeze the mask at the face without applying pressure on the occiput of the skull; and 5) a gentle squeeze in the bag with one finger and thumb is enough to deliver appropriate tidal volumes.
Immediately after the instruction, the second round of recordings were made, participants were not allowed to practise first and the instruction was only performed once for each participant.
Analysis and Results
Mask leak, PIP given and dispersion of pressures (expressed in SD) before and after training were analysed and compared. Pressures above 35 cm H2O were considered excessive. All signals were digitised and recorded at 200 Hz using a laptop with a data acquisition program (Spectra, Grove Medical, Hampton, England). Breaths were analysed on a breath-to-breath basis. Parameters were compared using a Wilcoxon non-parametric test.
Before and after the short training, experienced caregivers had minimal median (IQR) mask leak [14 (3-75) vs. 3 (0-53) percent; p<0.01]. Inexperienced users had large leak which decreased from 51 (7-91) percent before training to 11 (2-71) percent after training (p<0.01). Pressures above 35 cm H2O hardly occurred in experienced caregivers [0 (0-5) vs. 0 (0-0) percent; non-significant difference]. In inexperienced caregivers this frequently occurred but decreased considerably after training [94 (46-100) vs. 2 (0-70) percent; p<0.01].
Conclusion
The two-minute training on bag and mask ventilation was effective. This short and simple 'key points' training significantly decreased mask leak to acceptable levels in both experienced and inexperienced caregivers. The training had no influence in the inconsistency of the given pressures. However, the amount of high pressures given by inexperienced users, for which the pop-off valve apparently does not protect, considerably decreased after training. To improve immediate ventilation skills, this two-minute bag and mask training could easily be incorporated into training programmes.
Image Credit: Laerdal.com
References:
van Vonderen J J, Witlox R S, Kraaij S, te Pas A B (2014) Two-Minute
Training for Improving Neonatal Bag and Mask Ventilation. PLoS One.
2014; 9(10): e109049. PMCID: PMC4184825
Latest Articles
ventilation, ICU, resuscitation, PPV, neonatologists
Worldwide, an estimated three to six percent of newborn infants need assisted positive pressure ventilation (PPV) at birth. Adequate PPV is the cornerstone...