Targeted temperature management is the key intervention for improving neurological outcomes after cardiac
arrest. We discuss new data on the optimal timing and modalities of targeted temperature management. It took nearly half a century, from 1957 to
2002, for therapeutic hypothermia to acquire
its current status as a key intervention for
improving neurological outcomes in survivors
of cardiac arrest. Despite growing interest from
healthcare workers and researchers, many questions
remain unanswered regarding this treatment
tool. Recent large multicentre trials raised
as many questions as they provided answers. In this
review, we will try to reconcile new and old data,
explain discordant results, and discuss future trials
of therapeutic hypothermia and other aspects of the
management of cardiac arrest survivors.
Indications of Therapeutic Hypothermia
Cardiac Arrest in Shockable Rhythm
For the past 12 years, treatment decisions for
cardiac arrest survivors have relied largely on
two trials reported in 2002 (Hypothermia after
Cardiac Arrest Study Group 2002; Bernard et al.
2002). Both trials showed improved neurological outcomes with hypothermia between 32° and 34°
compared to normothermia after cardiac arrest
in shockable rhythm. The vast majority of observational,
retrospective, and propensity-adjusted
cohort studies support this finding. The landmark
Targeted Temperature Management (TTM)
trial reported in 2013 (Nielsen et al. 2013) failed
to demonstrate any difference in neurological
outcomes or survival between hypothermia at
33° and hypothermia at 36°C. The results of the
TTM trial complicate the interpretation of another
preliminary study showing better outcomes with
hypothermia at 32°C compared to 34°C (Lopezde-Sa
et al. 2012).
These data have generated active controversy. The
International Liaison Committee on Resuscitation
(ILCOR) issued the following statement:
Pending formal consensus on the optimal temperature, we suggest
that clinicians provide post-resuscitation care based on the current
treatment recommendations. We accept that some clinicians may
make a local decision to use a target temperature of 36°C pending
this further guidance (ILCOR 2013).
The European Resuscitation Council (ERC) new
guidelines issued in October 2015 specify: “maintain
a constant, target temperature between 32°C
and 36°C for those patients in whom temperature
control is used” (Nolan et al. 2015).
Several considerations may help to reconcile
new data from trials of TTM and older results.
First, TTM at 36° is not normothermia [37°]. The
difference in neurological outcomes between
two groups depends on the temperature difference:
for instance, a 3° difference [e.g., 33° vs.
36°] may produce a 33% smaller benefit than a 4°
difference [e.g., 33° vs. 37°]. Second, the control
groups were not comparable between the trials
reported in 2002 (Hypothermia after Cardiac
Arrest Study Group 2002; Bernard et al. 2002)
and 2013 (Nielsen et al. 2013). Interest in the
management of cardiac arrest increased massively
during this interval, leading to marked improvements
in outcomes, due not only to TTM, but also
to changes in the management of heart disease,
notably the use of coronary angiography (Dumas
et al. 2012), haemodynamics and gas exchange.
The benefits from these other interventions may
decrease the relative effects of TTM to levels detectable only in large sample sizes. Third, 10% to 20%
of patients survived without marked neurological
damage (Cerebral Performance Category 1
or 2) in subgroups with favourable prognostic
factors (bystander cardiopulmonary resuscitation
and short low-flow time) in the 2002 trials
and in patients with poor prognostic factors (no
bystander, longer low-flow time and, above all,
non-shockable rhythm) in recent trials. Conceivably,
patients with more severe brain damage may
benefit from lower temperatures, e.g., 33°C instead
of 36°C. In several retrospective studies, benefits
from TTM at 33°C were more marked in patients
with longer no-flow or low-flow times (Testori
et al. 2012; Kagawa et al. 2010; Drennan et al.
2014), but this result was not replicated in a post
hoc analysis of data from the TTM trial (Kjaergaard
et al. 2015).
Cardiac Arrest in Non-Shockable Rhythm
Patients with cardiac arrest in non-shockable
rhythms now account for the majority of patients
admitted to the ICU after the return of spontaneous
circulation (ROSC) (Wong et al. 2014).
Their prognosis is considerably poorer compared
to that of patients with cardiac arrest in shockable
rhythms. Nevertheless, very few data are available
on this specific population, which is more heterogeneous
than the population with cardiac arrest in
shockable rhythm, as causes include heart disease,
pulmonary embolism, asphyxia, hanging and
many other conditions. Except for a subgroup analysis
in the TTM trial (Frydland et al. 2015), no data
from randomised trials are available. Guidelines
still recommend TTM after non-shockable cardiac
arrest. An ongoing trial will provide information
on this growing population of cardiac arrest survivors
(Lascarrou et al. 2015).
1. Modalities of Targeted Temperature
management (Nau et al. 1992)
Induction of TTM
Recent data on conducting TTM, particularly the
induction phase, are available. Earlier induction
seemed associated with better outcomes in animal
experiments and small observational studies.
However, no adequately powered trial in humans has confirmed this possibility. Pre-hospital induction
of mild hypothermia by infusing 4°C normal
saline immediately after ROSC not only failed to
improve neurological outcomes, but was also
associated with higher rates of re-arrest and acute
pulmonary oedema (Kim et al. 2014). However,
this trial has several methodological weaknesses:
only 77% of patients managed with pre-hospital
hypothermia subsequently received hospital
maintenance of hypothermia, and oxygenation
level was unusually high in the patients diagnosed
with acute pulmonary oedema. A major source
of bias in studies of TTM is the faster speed of
cooling in the sickest patients, due to absence of
the hypothalamic response to cooling (Lin et al.
2014). There is probably a need for studies of
fluids other than normal saline for inducing hypothermia.
In particular, balanced crystalloid solutions
(Hartman’s solution and others) are generating
considerable attention for managing sepsis,
and may deserve similar interest in the treatment
of cardiac arrest survivors. Finally, an intranasal
cooling system for inducing hypothermia in the
field, with no fluid infusion, is under investigation
(Nordberg et al. 2013).
Maintenance of TTM
Hypothermia can be maintained using a specific
internal or external device equipped with a
temperature control driver or using non-specific
means, such as a makeshift tent and conventional
ice packs. Studies of specific devices, including
a recent randomised trial (Deye et al. 2015),
showed no improvement in neurological outcomes
compared to nonspecific means, although nurse
workload was lower.
Duration of TTM and Rewarming Phase
No adequately designed trial is available for guiding
decisions about the duration of hypothermia or the
speed of rewarming. Based on the trials reported
in 2002, TTM is usually maintained for 12-24
hours. However, the longer duration used in the
TTM Trial may have beneficial effects, notably on
the inflammatory response (Bisschops et al. 2014).
Another trial addressing hypothermia duration is
under way [NCT02035839] (Zoll Circulation Inc
2015). Last, findings from observational studies
support a slow pace of rewarming, and further
information on this point will be provided by an
ongoing trial [NCT02555254] (Centre Hospitalier
Departemental Vendee 2015).
2. Patient Management During Therapeutic
Hypothermia
A specific protocol adapted to local conditions
must be developed and applied to optimise
neurological outcomes after TTM (Sunde et al.
2007). All healthcare workers must adhere to
guidelines (Orban et al. 2012; Camp-Rogers
et al. 2013). Sedation and analgesia are necessary
during TTM induction, maintenance and
rewarming, but interfere with the neurological
examination, thereby hindering outcome
prediction. The predicted neurological prognosis
is a major consideration when deciding
whether treatment limitation decisions are in
order. There is some evidence that drugs with
short half-lives, such as propofol and remifentanil,
may deserve preference over drugs
with longer half-lives, such as midazolam and
fentanyl (Bjelland et al. 2012). TTM is often
associated with shivering. The first-line treatment
of shivering is adjustment of the sedation
and analgesia. If shivering persists, surface
counterwarming, dexmedetomidine, or neuromuscular
blockade may be used depending on
the local protocol. Recent data suggest beneficial
effects of neuromuscular blockade on neurological
outcomes (Lascarrou et al. 2014; Salciccioli
et al. 2013), but the level of evidence is low and
further studies are needed.
3. Side Effects
Recent trials have improved our understanding of
the risk/benefit ratio of TTM. Most adverse effects
are well-known and have no effect on mortality or morbidity; examples include changes in the
electrocardiogram or in serum potassium levels.
A few are more serious and can lead to increased
morbidity. The pathophysiological effects of hypothermia
explain the increased risk of bacterial
pneumonia associated with TTM in all studies.
This risk is particularly high in cardiac arrest
patients, whose upper airways are unprotected
until endotracheal intubation is performed.
Nevertheless, no effect of pneumonia on neurological
outcomes was found in recent studies,
regardless of their design (observational, observational
with propensity-adjusted analysis) (Gagnon
et al. 2015; Perbet et al. 2011).
4. Prognostication: Early and Late
Large strides have been made in neurological
prognostication since the trials reported in 2002.
The two main advances are the clear definition of
situations warranting treatment limitation decisions
in the most recent trials and the availability
of validated and accurate prognostication criteria
that can be used at the bedside. These tools consist
of clinical tests (Glasgow motor score and brainstem
reflexes), serum assays of neuron-specific
enolase and S-100B, evoked potential recordings
and electroencephalography and magnetic resonance
imaging (MRI). Neurological prognostication
now relies on a combination of findings
obtained using these tools. It cannot be performed
accurately until 72 hours after the arrest, except when the prognosis is catastrophic, defined in
the TTM trial for instance as “the patient becomes
brain dead, has an early myoclonus status or, if
there are strong ethical reasons to withdraw intensive
care” (Nielsen et al. 2013). Recent European
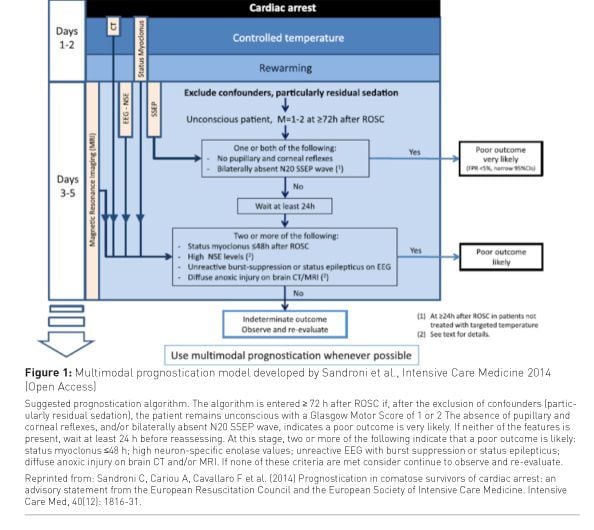
guidelines (see Figure 1) provide clinicians
with useful guidance (Sandroni et al. 2014).
However, according to a recent survey intensivists
vary widely regarding the tools they use for
neurological prognostication, and their decisions
may be based as much on beliefs as on science
(Friberg et al. 2015).
Predicting a poor neurological prognosis is
important to determine whether life-sustaining
interventions should be withheld or withdrawn.
There is growing evidence that factors predicting
a good prognosis can be assessed during TTM.
Thus shivering (Nair and Lundbye 2013) and
bradycardia (Staer-Jensen et al. 2014; Thomsen et
al. 2015) during TTM are associated with better
outcomes. Furthermore, although the use of
specific cooling devices does not affect patient
outcomes, they indicate how much power is
needed to cool the patient, and greater power
is associated with better outcomes (Murnin et
al. 2014).
Predictors of neurological outcomes must
be well characterised both for designing trials
of individualised treatment strategies and to
provide accurate information to the family.
Attention to cognitive impairments and
emotional difficulties in cardiac arrest survivors
may improve outcomes even in the medium and
long term (Moulaert et al. 2015).
Conclusion
Although recent efforts have chiefly targeted the
first three links in the chain of survival (Becker
et al. 2015), we must keep in mind that TTM is
the only intervention proven to favourably affect
the fourth link. Huge knowledge gaps still exist
regarding all aspects of patient management
during TTM. Further trials are needed to fill these
gaps and to provide the information needed to
develop individualised treatment strategies.
Acknowledgements
Becker LB, Aufderheide TP, Graham R (2015) Strategies
to improve survival from cardiac arrest: A report from the institute of
medicine. JAMA, 314(3): 223-4.
Bernard SA, Gray TW, Buist MD et al. (2002) Treatment
of comatose survivors of out-of-hospital cardiac arrest with induced
hypothermia. N Engl J Med, 346(8): 557-63.
Bisschops L, van der Hoeven JG, Mollnes TE et al. (2014)
Seventy-two hours of mild hypothermia after cardiac arrest is associated with a
lowered inflammatory response during rewarming in a prospective observational
study. Crit Care, 18(5): 546.
Bjelland TW, Ola D, Kjell K et al. (2012) Propofol and
remifentanil versus midazolam and fentanyl for sedation during therapeutic
hypothermia after cardiac arrest: a randomised trial. Intensive Care Med, 38(6):
959-67.
Camp-Rogers TR, Sawyer KN, McNicol DR et al. (2013) An
observational study of patient selection criteria for post-cardiac arrest
therapeutic hypothermia. Resuscitation, 84(11): 1536-9.
Deye N, Cariou A, Girardie P et al. (2015) Endovascular
versus external targeted temperature management for out-of-hospital cardiac
arrest patients: a randomized controlled study. Circulation, 132(3): 182-93.
Drennan IR, Lin S, Thorpe KE et al. (2014) The effect
of time to defibrillation and targeted temperature management on functional
survival after out-of-hospital cardiac arrest. Resuscitation, 85(11): 1623-8.
Dumas F, White L, Stubbs BA et al. (2012) Long-term
prognosis following resuscitation from out of hospital cardiac arrest: role of
percutaneous coronary intervention and therapeutic hypothermia. J Am Coll Cardiol,
60(1): 21-7.
Friberg H, Cronberg T, Dünser MW et al. (2015) Survey
on current practices for neurological prognostication after cardiac arrest.
Resuscitation, 90: 158-62.
Frydland M, Kjaergaard J, Erlinge D et al. (2015)
Target temperature management of 33°C AND 36°C in patients with out-of-hospital
cardiac arrest with initial non-shockable rhythm. A TTM sub-study.
Resuscitation, 89:142-8.
Gagnon DJ, Nielsen N, Fraser GL et al. (2015)
Prophylactic antibiotics are associated with a lower incidence of pneumonia in
cardiac arrest survivors treated with targeted temperature management.
Resuscitation, 92: 154-9.
Hypothermia after Cardiac Arrest Study Group (2002)
Mild therapeutic hypothermia to improve the neurologic outcome after cardiac
arrest. N Engl J Med, 346(8): 549-56.
Kagawa E, Inoue I, Kawagoe T et al. (2010) Who benefits most from mild therapeutic hypothermia in coronary
intervention era? A retrospective and propensity-matched study. Crit Care, 14(4):
R155.
Kim F, Nichol G, Maynard C et al. (2014) Effect of
prehospital induction of mild hypothermia on survival and neurological status
among adults with cardiac arrest: a randomized clinical trial. JAMA, 311(1):
45-52.
Kjaergaard J, Nielsen N, Winther-Jensen M et al. (2015)
Impact of time to return of spontaneous circulation on neuroprotective effect
of targeted temperature management at 33 or 36 degrees in comatose survivors of
out-of hospital cardiac arrest. Resuscitation, 96:
310-6.
Lascarrou JB, Meziani F, Le Gouge A et al. (2015) Therapeutic hypothermia after nonshockable cardiac
arrest: the HYPERION multicenter, randomized, controlled, assessor-blinded,
superiority trial. Scand J T Resusc Emerg Med, 23: 26.
Lascarrou JB, Le Gouge A, Dimet J et al. (2014) Neuromuscular blockade during therapeutic hypothermia
after cardiac arrest: observational study of neurological and infectious
outcomes. Resuscitation, 85(9): 1257-62.
Lin S, Scales DC, Dorian P et al. (2014) Targeted
temperature management processes and outcomes after out-of-hospital cardiac
arrest: an observational cohort study*. Crit Care Med,
42(12): 2565-74.
Lopez-de-Sa
E, Rey JR, Armada E et al. (2012)
Hypothermia in comatose survivors from out-of-hospital cardiac arrest: pilot
trial comparing 2 levels of target temperature. Circulation, 126(24): 2826-33.
Moulaert VR, van Heugten CM, Winkens B et al. (2015)
Early neurologically-focused follow-up after cardiac arrest improves quality of
life at one year: A randomised controlled trial. Int J Cardiol, 193: 8-16.
Murnin MR, Sonder P, Janssens GN, et al. (2014)
Determinants of heat generation in patients treated with therapeutic
hypothermia following cardiac arrest. JAm Heart Assoc, 3(3): e000580.
Nair SU, Lundbye JB (2013) The occurrence of shivering
in cardiac arrest survivors undergoing therapeutic hypothermia is associated
with a good neurologic outcome. Resuscitation, 84(5): 626-9.
Nau R, Prange HW, Klingelhofer J et al. (1992) Results
of four technical investigations in fifty clinically brain dead patients.
Intensive Care Med, 18(2): 82-8.
Nielsen N, Wetterslev J, Cronberg T et al. (2013)
Targeted temperature management at 33 degrees C versus 36 degrees C after
cardiac arrest. N Engl J Med, 369(23): 2197-206.
Nolan JP, Soar J, Cariou A et al. (2015) European
Resuscitation Council and European Society of Intensive Care Medicine guidlines
for post-resuscitation care 2015: section 5 of the European Resuscitation
Council guidelines for Resuscitation 2015. Resuscitation, Oct 2015, 202-22.
Nordberg P, Taccone FS, Castren M et al. (2013) Design
of the PRINCESS trial: pre-hospital resuscitation intra-nasal cooling
effectiveness survival study (PRINCESS). BMC Emerg Med, 13: 21.
Orban JC, Cattet F, Lefrant JY et al. (2012) The
practice of therapeutic hypothermia after cardiac arrest in France: a national
survey. PLoS One, 7(9): e45284.
Perbet S, Mongardon N, Dumas F et al. (2011) Early
onset pneumonia after cardiac arrest: characteristics, risk factors and
influence on prognosis. Am J Respir Crit Care Med, 184(9): 1048-54.
Salciccioli JD, Cocchi MN, Rittenberger JC et al.
(2013) Continuous neuromuscular blockade is associated with decreased mortality
in post-cardiac arrest patients. Resuscitation, 84(12): 1728-33.
Staer-Jensen H, Sunde K, Olasveengen TM et al. (2014)
Bradycardia during therapeutic hypothermia is associated with good neurologic
outcome in comatose survivors of out-of-hospital cardiac arrest. Crit Care Med,
42(11): 2401-8.
Sunde K, Pytte M, Jacobsen D et al. (2007)
Implementation of a standardised treatment protocol for post resuscitation care
after out-of-hospital cardiac arrest. Resuscitation, 73(1): 29-39.
Testori
C, Sterz F, Holzer M et al. (2012) The beneficial effect of mild therapeutic
hypothermia depends on the time of complete circulatory standstill in patients
with cardiac arrest. Resuscitation, 83(5): 596-601.
Thomsen
JH, Hassager C, Bro-Jeppesen J et al. (2015) Sinus bradycardia during
hypothermia in comatose survivors of out-of-hospital cardiac arrest - a new
early marker of favorable outcome? Resuscitation, 89: 36-42.
Wong
MK, Morrison LJ, Qiu F et al. (2014) Trends in short- and long-term survival
among out-of-hospital cardiac arrest patients alive at hospital arrival.
Circulation, 130(21): 1883-90.








