ICU Management & Practice, Volume 17 - Issue 2, 2017
Inspired by the Difficult Airway Society Guidelines and the Vortex Cognitive Tool
One of the main recommendations of the 4th National Audit Project of the UK Royal College of Anaesthetists and the Difficult Airway Society was that every intensive care unit (ICU) should have access to a difficult airway trolley, which should have the same content and layout as the one found in the operating department (Cook et al. 2011). At Royal North Shore Hospital in Sydney, Australia, we designed trolleys with standardised equipment for use in the ICU, emergency and operating departments.
The trolley consists of 4 drawers corresponding to Plans A, B, C and D of the Difficult Airway Society guidelines for the management of unanticipated difficult intubation (Frerk et al. 2015). The symbols used to depict these Plans are from the Vortex cognitive aid (vortexapproach.org) (Chrimes 2016).
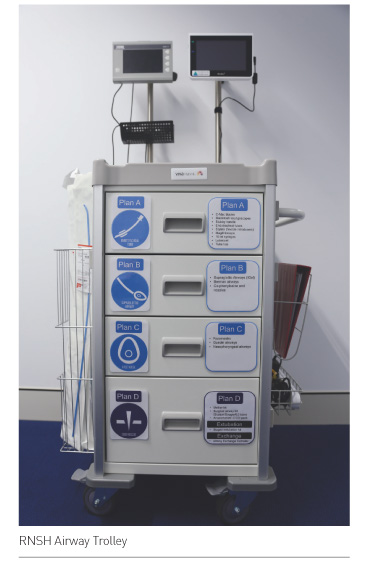
The first drawer (Plan A, Endotracheal Tube) contains all the equipment necessary for endotracheal intubation by laryngoscopy, including Storz C-Mac® blades for use with the monitor attached to one of the upright poles on the back of the trolley.
The second drawer (Plan B, Supraglottic Airway Device, SAD) contains secondgeneration SADs (igel®, Intersurgical) for airway rescue. If circumstances allow (i.e the patient can be oxygenated via the SAD, and it is thought appropriate), the SAD can be converted to an endotracheal tube with the use of the Ambu® aScope™, using the monitor attached to the other upright pole, with or without the Aintree Intubating Catheter (AIC, Cook®). The AICs and bronchoscopes are located in the side baskets.
The third drawer (Plan C, Facemask) contains facemasks, nasopharyngeal and oropharyngeal airways of various sizes.
The fourth drawer (Plan D, CICO* rescue) contains equipment for cannula, surgical and Seldinger cricothyroidotomy techniques. It also contains an Airway Exchange Catheter and Staged Extubation Kit (Cook®).
For intensive care and emergency clinicians, the goal is almost always endotracheal intubation. We appreciate that this is not the case in the operating department, where a SAD may be the first choice. The drawers are arranged in the order outlined above for the sake of standardisation across the hospital.
On the side of the trolley is a file containing our Emergency Intubation Checklist and Emergency Airway Cognitive Tool, which combines the DAS and Vortex approaches to difficult airway management. We believe that the DAS guidelines should be used for forward planning and to help with the choice of techniques, while the Vortex cognitive aid helps the team with decision making, such as when to abandon a technique and move onto the next.
A detailed description of the airway trolley, checklist and cognitive tool mentioned above can be found at ccam.net.au, a website which serves as the pre-reading for the Critical Care Airway Management Course, a not-for-profit course run at our hospital twice a year.
*CICO = Can’t Intubate, Can’t Oxygenate
References:
Chrimes N (2016) The Vortex: a universal ‘highacuity implementation tool’ for emergency airway management. Br J Anaesth, 117 Suppl 1: i20-i27.
Cook TM, Woodall N, Harper J et al. (2011) Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 2: intensive care and emergency departments. Br J Anaesth, 106(5): 632-42.
Frerk C, Mitchell VS, McNarry AF et al. (2015) Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. Br J Anaesth, 115(6): 827-48.







